Best Treatment for Pneumonia. Similarities To COVID-19
What is Pneumonia?
Blue indicates link
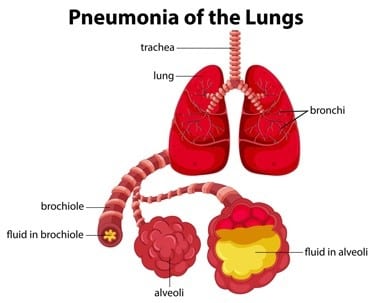
Pneumonia is an inflammatory condition of the lung affecting primarily the small air sacs known as alveoli. Typically, symptoms include some combination of productive or dry cough, chest pain, fever, and difficulty breathing. The severity of the condition is variable.
Pneumonia is a lung infection that can range from mild to so severe that you have to go to the hospital.
It happens when an infection causes the air sacs in your lungs (your doctor will call them alveoli) to fill with fluid or pus. That can make it hard for you to breathe in enough oxygen to reach your bloodstream.
Anyone can get this lung infection. But infants younger than age 2 and people over age 65 are at higher risk. That’s because their immune systems might not be strong enough to fight it.
You can get pneumonia in one or both lungs. You can also have it and not know it. Doctors call this walking pneumonia. Causes include bacteria, viruses, and fungi. If your pneumonia results from bacteria or a virus, you can spread it to someone else.
Lifestyle habits, like smoking cigarettes and drinking too much alcohol, can also raise your chances of getting pneumonia.
Some cases of pneumonia are life-threatening. Around 50,000 people die each year of pneumonia in the U.S. Although anyone of any age can be affected, pneumonia is more common in elderly people and often occurs when the immune system becomes weakened via a prior infection or another condition.
Pneumonia is generally more serious when it affects older adults, infants, and young children, those with chronic medical conditions, or those with weakened immune function.
Types of Pneumonia:
If you get pneumonia, it means you have an infection in your lungs caused by bacteria, viruses, and other germs. Learning the type you have helps your doctor suggest a treatment.
Doctors describe the type of pneumonia you have based on where you came down with your infection. You may hear health pros use these terms:
Hospital-acquired pneumonia. You catch this type during a stay in a hospital. It can be serious because the bacteria causing pneumonia can be resistant to antibiotics.
You’re more likely to get this type if:
- You’re on a breathing machine
- You can’t cough strongly enough to clear your lungs
- You have a tracheostomy (trach) tube to help you breathe
- Your immune system — your body’s defense against germs — is weak from disease or treatment
Community-acquired pneumonia. It’s a fancy way of saying you got infected somewhere other than a hospital or long-term care facility. Community-acquired pneumonia can be caused by bacteria, viruses, and fungi. Vaccines can help protect against the flu virus and certain bacteria that can also cause pneumonia.
Community-acquired pneumonia also includes aspiration pneumonia, which you get if you breathe food, fluid, or vomit into your lungs. It’s more likely to happen if you have problems swallowing or coughing. If you can’t cough up the material you took in, bacteria can multiply in your lungs.
Doctors also break down the kinds of pneumonia by the causes of the disease: bacteria, viruses, or fungi.
Bacterial Pneumonia:
Bacteria cause most cases of community-acquired pneumonia in adults.
You can catch pneumonia when someone who is infected coughs or sneezes. Bacteria-filled droplets get into the air, where you can breathe them into your nose or mouth.
If you have a weakened immune system, your chances of getting pneumonia are greater. You’re also more likely to get it if you have a condition like asthma, emphysema, or heart disease.
You may notice symptoms like:
- A cough that brings up mucus
- Fever over 100.4 F
- Fast breathing
- Shortness of breath
- Chest pain
- Fatigue
Viral Pneumonia:
Viral pneumonia is an infection of your lungs caused by a virus. The most common cause is the flu, but you can also get viral pneumonia from the common cold and other viruses. These nasty germs usually stick to the upper part of your respiratory system. But the trouble starts when they get down into your lungs. Then the air sacs in your lungs get infected and inflamed, and they fill up with fluid.
Anything that weakens your body’s defenses (immune system) can raise your chances of getting pneumonia.
Other Classifications:
Other classification systems for pneumonia describe the way the inflammatory cells infiltrate the lung tissue or the appearance of the affected tissue (see the following examples).
- Bronchopneumonia causes scattered, patchy infiltrates of inflammation in the air sacs throughout the lungs. It is more diffuse than lobar pneumonia.
- Lobar pneumonia causes inflammation of one lobe of a lung and typically involves all the airspaces in a single lobe.
- Lipoid pneumonia is characterized by the accumulation of fats within the airspaces. It can be caused by aspiration of oils or associated with airway obstruction.
Am I More Likely to Get It?
You have a higher chance of getting viral pneumonia if you:
- Are 65 or older
- Have chronic (ongoing) conditions like asthma, diabetes, or heart disease
- Are recovering from surgery
- Don’t eat right or get enough vitamins and minerals
- Have another condition that weakens your body’s defenses
- Smoke
- Drink too much alcohol
- Are HIV positive
- Recently had an organ transplant
- Have leukemia, lymphoma, or severe kidney disease
Symptoms of Viral Pneumonia
Viral pneumonia usually moves in steadily over a few days. On the first day, it feels like the flu, with symptoms like:
- Fever
- Dry cough
- Headache
- Sore throat
- Loss of appetite
- Muscle pain
After a day or so your fever might get worse. You might also feel like you can’t catch your breath. If your lungs are invaded with bacteria, you might also get some of the same symptoms as bacterial pneumonia, like:
- A wet, gunky cough that produces green, yellow, or bloody mucus
- Chills that make you shake
- Fatigue (feeling very tired)
- Low appetite
- Sharp or stabby chest pain, especially when you cough or take a deep breath
- Sweating a lot
- Fast breathing and heartbeat
- Blue lips and fingernails
- Confusion, especially if you’re older
Can I Prevent Viral Pneumonia?
You can do these things to help lower your odds of getting viral pneumonia:
- Get a flu shot every year.
- Wash your hands regularly, especially after you go to the bathroom and before you eat.
- Eat right, with plenty of fruits and vegetables.
- Exercise.
- Get enough sleep.
- Don’t smoke.
- Stay away from people who are sick.
Walking Pneumonia:
“Walking Pneumonia” sounds like it could be the name of a sci-fi horror flick. But it’s actually the least scary kind of pneumonia. It can be milder than the other types, and you usually don’t have to stay in the hospital. You could have walking pneumonia and not even know it.
It Might Feel Like a Cold:
Walking pneumonia is how some people describe a mild case of pneumonia. Your doctor might call it “atypical pneumonia” because it’s not like more serious cases.
Lung infection is often to blame. Lots of things can cause it, including:
- Bacteria
- Viruses
- Fungi
- Chemicals
- Inhaled food
Walking pneumonia usually is due to a bacterium called Mycoplasma pneumoniae.
If you have this condition, you probably won’t have to stay in bed or in the hospital. You might even feel good enough to go to work and keep up your regular routine, just as you might with a cold.
Who Gets It?
Anyone can get it. Walking pneumonia from mycoplasma is most common in children, military recruits, and adults younger than 40.
People who live and work in crowded places — such as schools, dorms, military barracks, and nursing homes — are more likely to be exposed to it.
Late summer and fall are the most common times of the year for you to get walking pneumonia. But infections can happen throughout the year.
Is It Contagious?
Yes. It spreads through sneezes or coughs. But it spreads slowly. If you get it, you could be contagious (which means you could spread it to other people) for up to 10 days.
Researchers think it takes a lot of close contact with an infected person for you to develop walking pneumonia. Still, there are widespread outbreaks every four to eight years.
Symptoms:
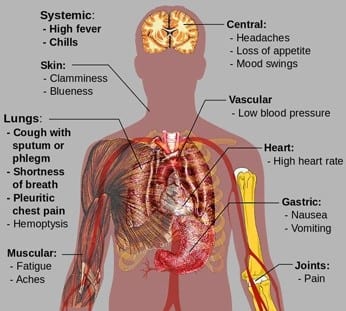
Symptoms generally start 15 to 25 days after you’re exposed to mycoplasma and slowly worsen over two to four days. You might have:
- Chest pain when you take a deep breath in
- Cough that may come in violent spasms
- Mild flu-like symptoms such as fever and chills
- Sore throat
- Headache
- Tiredness
- Lingering weakness that may last after other symptoms go away
Some people with walking pneumonia may also have an ear infection, anemia, or a skin rash.
What Causes Pneumonia?
Many germs can cause pneumonia. The most common are bacteria and viruses in the air we breathe. Your body usually prevents these germs from infecting your lungs. But sometimes these germs can overpower your immune system, even if your health is generally good.
Bacteria and viruses are the main causes of pneumonia. Pneumonia-causing germs can settle in the alveoli and multiply after a person breathes them in.
Pneumonia can be contagious. The bacteria and viruses that cause pneumonia are usually inhaled.
They can be passed on through coughing and sneezing or spread onto shared objects through touch.
The body sends white blood cells to attack the infection. This is why the air sacs become inflamed. The bacteria and viruses fill the lung sacs with fluid and pus, causing pneumonia.
The most common cause of viral pneumonia in adults is the influenza virus. A number of different respiratory viruses cause pneumonia in children, such as a respiratory syncytial virus (RSV). While viral pneumonia tends to be less severe than bacterial pneumonia, there is a risk of developing secondary bacterial pneumonia when viral pneumonia is present. Influenza viruses and respiratory syncytial viruses (RSV), however, may cause serious problems in some patients.
Other virus types that can cause pneumonia include measles and varicella (chickenpox) viruses. Rarely, certain viruses may cause lethal types of pneumonia such as SARS (severe acute respiratory syndrome) or MERS (Middle East respiratory syndrome); both diseases are caused by different coronaviruses.
Is Pneumonia an Airborne Disease?
Pneumonia is caused by infectious agents that can spread to others depending upon the type of organism causing pneumonia. Usually, the organisms spread from person to person by contact with an infected person’s mouth or when small droplets become airborne from coughing or sneezing. In addition, once pneumonia develops in the lungs, it may spread to other lobes of the lung, or even to the other lung. In severe cases, the organisms causing pneumonia may spread to other organs of the body and cause damage or even death.
Usually, the organisms spread from person to person by contact with an infected person’s mouth or when small droplets become airborne from coughing or sneezing.
They may also spread via air-borne droplets from a cough or sneeze.
Personal Note:
Pneumonia is not considered an airborne disease, BUT it seems this is not a definitive answer. It is communicated through droplets when someone sneezes or coughs. The transmission is very similar to the Covid-19 that has put the world into a crisis mode.
What is Airborne Transmission?
Airborne transmission occurs when bacteria or viruses travel on dust particles or on small respiratory droplets that may become aerosolized when people sneeze, cough, laugh, or exhale. They hang in the air much like invisible smoke. They can travel on air currents over considerable distances. These droplets are loaded with infectious particles.
With airborne transmission, direct contact with someone who is infected is not necessary to become ill.
The amount of exposure necessary varies from disease to disease. With chickenpox, a child could easily catch it from another aisle in a supermarket. With tuberculosis, closer contact and less air circulation are often needed.
Many common infections can spread by airborne transmission, at least in some cases, including Anthrax (inhalational) Chickenpox, Influenza, Measles, Pertussis, (whooping cough) Smallpox, and Tuberculosis.
Diagnosis:
Your doctor will start by asking about your medical history and doing a physical exam, including listening to your lungs with a stethoscope to check for abnormal bubbling or crackling sounds that suggest pneumonia.
If pneumonia is suspected, your doctor may recommend the following tests:
- Blood tests. Blood tests are used to confirm an infection and to try to identify the type of organism causing the infection. However, precise identification isn’t always possible.
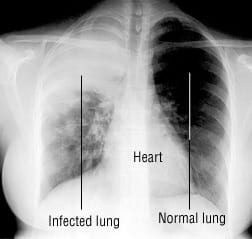
- Chest X-ray. This helps your doctor diagnose pneumonia and determine the extent and location of the infection. However, it can’t tell your doctor what kind of germ is causing pneumonia.
- Pulse oximetry. This measures the oxygen level in your blood. Pneumonia can prevent your lungs from moving enough oxygen into your bloodstream.
- Sputum test. A sample of fluid from your lungs (sputum) is taken after a deep cough and analyzed to help pinpoint the cause of the infection.
Your doctor might order additional tests if you’re older than age 65, are in the hospital, or have serious symptoms or health conditions. These may include:
- CT scan. If your pneumonia isn’t clearing as quickly as expected, your doctor may recommend a chest CT scan to obtain a more detailed image of your lungs.
- Pleural fluid culture. A fluid sample is taken by putting a needle between your ribs from the pleural area and analyzed to help determine the type of infection.
Treatment:
Treatment for pneumonia involves curing the infection and preventing complications. People who have community-acquired pneumonia usually can be treated at home with medication. Although most symptoms ease in a few days or weeks, the feeling of tiredness can persist for a month or more.
Specific treatments depend on the type and severity of your pneumonia, your age, and your overall health. The options include:
- Antibiotics. These medicines are used to treat bacterial pneumonia. It may take time to identify the type of bacteria causing your pneumonia and to choose the best antibiotic to treat it. If your symptoms don’t improve, your doctor may recommend a different antibiotic.
- Cough medicine. This medicine may be used to calm your cough so that you can rest. Because coughing helps loosen and move fluid from your lungs, it’s a good idea not to eliminate your cough completely. In addition, you should know that very few studies have looked at whether over-the-counter cough medicines lessen coughing caused by pneumonia. If you want to try a cough suppressant, use the lowest dose that helps you rest.
- Fever reducers/pain relievers. You may take these as needed for fever and discomfort. These include drugs such as aspirin, ibuprofen (Advil, Motrin IB, others), and acetaminophen (Tylenol, others).
Hospitalization:
You may need to be hospitalized if:
- You are older than age 65
- You are confused about time, people, or places
- Your kidney function has declined
- Your systolic blood pressure is below 90 millimeters of mercury (mm Hg) or your diastolic blood pressure is 60 mm Hg or below
- Your breathing is rapid (30 breaths or more a minute)
- You need breathing assistance
- Your temperature is below normal
- Your heart rate is below 50 or above 100
You may be admitted to the intensive care unit if you need to be placed on a breathing machine (ventilator) or if your symptoms are severe.
Children may be hospitalized if:
- They are younger than age 2 months
- They are lethargic or excessively sleepy
- They have trouble breathing
- They have low blood oxygen levels
- They appear dehydrated
Other Treatment Methods.
Always consult with your doctor first.
1) Pleurisy Root
Pleurisy root is really a favorite herbal remedy utilized in fighting pneumonia since it will help reduce inflammation of the pleural membranes in the lungs, enhance the secretion of healthful lung fluids, and is really a lymphatic system stimulant. Pleurisy root has been utilized to take care of many different illnesses, including pleurisy, pneumonia, bronchitis, influenza, and chronic coughing.
2) Baikal Skullcap
With this herb, it is recommended that you mix the skullcap, which is often acquired in Chinese herb shops, together with several other antibiotic herbs such as barberry, goldenseal, Oregon grape, and yellow root. However, always keep in mind that pneumonia is a possibly life-threatening disease and shouldn’t be taken lightly. Everyone should pay their primary healthcare provider a visit to ascertain whether herbal treatments make sense as either an alternative or complementary therapy in their overall pneumonia treatment.
3) Garlic
Among garlic’s added advantages as an antibiotic is its selectivity. Garlic appears to focus on bad germs without also killing the good bacteria that are required for the human body to work correctly. This works better than most prescription antibiotics that blindly kill good and bad bacteria. Talk with a health practitioner before pursuing this path.
4) Turmeric
Turmeric has a few medicinal properties and is extensively used in treating a host of ailments. Additionally, it aids against pneumonia. Other herbs like fenugreek, black pepper, and ginger will also be advantageous for your lungs when used together with turmeric. It’s possible for you to consume these either cooked or uncooked, your choice.
5) Ginger
Ginger is really a well-known remedy for treating the majority of respiratory diseases.
6) Holy Basil
Holy basil is likewise quite helpful with pneumonia. Add a bit of ground black pepper to a tea or juice from this herb and take it at six hourly intervals.
7) Remove Animal Proteins
Remove excessive quantities of animal protein from your daily diet. Excessive quantities of animal protein might be hard on your digestive tract, particularly should you be ill. When you’re sick, it’s important to keep yourself in a good routine (in the bathroom) and allow whole foods to work fast so that your body is able to consume their nutrients and fight the disease. A wholesome quantity of protein is found in vegetables like artichokes, beets, spinach, cauliflower, peas, eggplant, and potatoes.
8) Drink a Potassium Broth
Have some broth with your lunch. Creating a potassium broth is straightforward. It may be accomplished by juicing 4 cloves of garlic, 2 radishes, 2 big carrots, 2 stalks of celery plus a couple of pinches of parsley. It’s significant to have the maximum amount of potassium as you possibly can throughout a spell with pneumonia. Potassium helps repair damaged tissue within the lungs. When you’ve got a heart illness don’t drink a potassium broth; potassium in excessive amounts could be dangerous with such a condition.
9) Drink Some Carrot Juice
Drink a 12-oz glass of carrot juice with dinner. Add 1 tablespoon of pepper to make it more effective. Carrot juice can help the lungs greatly, and add anti-oxidants to your body’s damaged tissue. Carrot juice, in addition to being an excellent generator of vitamin A, can be rich in potassium, magnesium, calcium, phosphorus, iron, and vitamin B-complex. Cayenne pepper will raise the efficacy of the carrot juice.
10) Get Plenty of Vitamin C
Based on the Mayo Clinic, Vitamin C may play a part in the prevention of pneumonia. However, additional research is required to validate available study results.
11) Drink Water
Drink ample water. It’s normally advised to drink eight 8-oz. glasses daily to support a wholesome hydration level. When dealing with pneumonia, patients should attempt to drink between 8 to 10 eight-ounce glasses at a minimum.
Other Herbal Suggestions/Remedies
Astragalus also known as Huang Quai and milk vetch is a herb that is used for several medicinal purposes. Astragalus has antiviral and anti-inflammatory properties that help boost the proper functioning of the lungs and prevent the occurrence of various disorders like pneumonia and bronchitis. It is available in capsule, tincture, and liquid form. You can even make a tea out of this herb, just steep 2 teaspoons of this dried herb in boiling water. Then strain the water and drink it three times a day.
Pneumonia can be treated well with fenugreek tea. When pneumonia is in the early stage, tea made out of fenugreek seeds helps the body to perspire, dispel toxicity, and reduce fever due to pneumonia. A pneumonia patient should take this tea four times a day. You can reduce the quantity once you feel the difference in your condition. Infuse 15 grams of fenugreek seeds in 250 ml of water. Add a few drops of lemon to flavor the tea.
Tea tree oil has antibacterial and antimicrobial properties that say goodbye to pneumonia. Washcloth with tea tree oil and hot water. Add 4 drops of this tea tree oil to the wash cycle to destroy infectious organisms. Boil 2 cups of water in a saucepan and then remove from the heat. Add 6 drops of tea tree oil. Place a towel over your head and breathe in the steam to get rid of pneumonia symptoms.
Olive leaf has antibacterial and antimicrobial properties that help to fight off lung infections. Oleuropein is one of the active ingredients present in an olive leaf that helps to treat pneumonia. Other important compounds present in the olive leaf are Verbascoside, Caffeic acid, 4-0-glucoside, 7-0-glucoside, and Luteolin. Thanks to such important constituents that help to attack the organisms that cause fungal and bacterial infections. Just steep olive leaf in boiling water and drink it when it cools down.
Basil is an excellent herb that has anti-inflammatory properties that help to treat pneumonia. It is truly suggested to take beverages extracted from 7 to 8 basil leaves merged with black pepper to combat pneumonia. This decoction helps to soothe pneumonia symptoms. Take this infusion every 5 hours for the desired result. Apart from the above, Berries, garlic, sage, mullein, peppermint, apple cider vinegar, and cranberry juice also help to treat pneumonia.
The World Health Organization. Pneumonia Statics:
Pneumonia is the single largest infectious cause of death in children worldwide. Pneumonia killed 808 694 children under the age of 5 in 2017, accounting for 15% of all deaths of children under five years old. Pneumonia affects children and families everywhere but is most prevalent in South Asia and sub-Saharan Africa. Children can be protected from pneumonia, it can be prevented with simple interventions, and treated with low-cost, low-tech medication and care.
2.56 million people died from pneumonia in 2017. Almost a third of all victims were children younger than 5 years, it is the leading cause of death for children under five.
1. Pneumococcal disease can be very serious.
- Pneumococcal pneumonia causes an estimated 150,000 hospitalizations each year in the United States.
- Pneumococcal meningitis and bacteremia killed approximately 3,600 people in the United States in 2017.
WHY ARE THESE STATICS NOT BEING UPDATED? IF THEY ARE I SURE WOULD LIKE TO SEE THEM.
History
As early as the 1930s, scientists were reporting types of pneumonia that were “atypical” compared to characteristics seen in “typical” types of pneumonia. Patients with atypical pneumonia tended to be not as sick, have symptoms for longer, and not respond to some antibiotics used for treating “typical” pneumonia. In 1944, scientists discovered the agent that causes “atypical” pneumonia, later named Mycoplasma pneumoniae.
They first thought it was a virus or fungus so they chose the name “mycoplasma,” which is Greek for “fungus-formed.” Eventually, scientists learned that it is a bacterium with many unique characteristics. For example, it does not have a rigid cell wall, which affects the types of antibiotics that work well against it. It is also the smallest organism capable of living and reproducing on its own. Smaller germs, like viruses, have to live and reproduce inside cells.
Fast Forward from December 2019 to March 2020
Coronavirus (COVID-19)
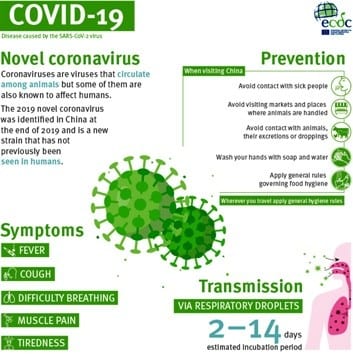
The similarities to Coronavirus (Covid-19) are scary. The same precautions are caused by droplets, coughing, and sneezing. It affects your respiratory system and lungs.
The need for social distancing. Wearing face masks.
Pneumonia goes as far back as the 1930s. Covid-19. December 2019.
Social Distancing goes as far back as 700 years.
The Spanish Flu Pandemic 1918. Attacked the respiratory system.
What have we learned?
Also known as SARS-CoV-2, nCov, 2019 Novel Coronavirus.
A novel coronavirus outbreak was first documented in Wuhan, Hubei Province, China in December 2019.
COVID-19 is a new illness that can affect your lungs and airways. It’s caused by a virus called coronavirus. Symptoms of coronavirus (COVID-19) are a cough, high temperature, and shortness of breath. Simple measures like washing your hands often with soap and water can help stop viruses like coronavirus (COVID-19) from spreading. It’s not known exactly how coronavirus (COVID-19) spreads from person to person, but similar viruses are spread in cough droplets. There’s no specific treatment for coronavirus (COVID-19). Treatment aims to relieve the symptoms until you recover.
The Spanish flu pandemic of 1918, the deadliest in history, infected an estimated 500 million people worldwide—about one-third of the planet’s population—and killed an estimated 20 million to 50 million victims, including some 675,000 Americans. The 1918 flu was first observed in Europe, the United States, and parts of Asia before swiftly spreading around the world. At the time, there were no effective drugs or vaccines to treat this killer flu strain. Citizens were ordered to wear masks, schools, theaters, and businesses were shuttered and bodies piled up in makeshift morgues before the virus ended its deadly global march.
Spanish Flu Symptoms:
The first wave of the 1918 pandemic occurred in the spring and was generally mild. The sick, who experienced such typical flu symptoms as chills, fever, and fatigue, usually recovered after several days, and the number of reported deaths was low.
However, a second, highly contagious wave of influenza appeared with a vengeance in the fall of that same year. Victims died within hours or days of developing symptoms, their skin turning blue and their lungs filling with fluid that caused them to suffocate. In just one year, 1918, the average life expectancy in America plummeted by a dozen years.
Although the death toll attributed to the Spanish flu is often estimated at 20 million to 50 million victims worldwide, other estimates run as high as 100 million victims—around 3 percent of the world’s population. The exact numbers are impossible to know due to a lack of medical record-keeping in many places.
Officials in some communities imposed quarantines, ordered citizens to wear masks, and shut down public places, including schools, churches, and theaters. People were advised to avoid shaking hands and to stay indoors, libraries put a halt on lending books, and regulations were passed banning spitting.
https://www.history.com/topics/world-war-i/1918-flu-pandemic
Social Distancing and Quarantine Were Used in Medieval Times to Fight the Black Death

Almost 700 years ago, the overwhelmed physicians and health officials fighting a devastating outbreak of bubonic plague in medieval Italy had no notion of viruses or bacteria, but they understood enough about the Black Death to implement some of the world’s first anti-contagion.
Really does anything written here sound familiar?
I do not want to be a provider of gloom and doom but it is important we know the facts.
PLEASE ALWAYS SEEK MEDICAL ADVICE.
SOCIAL DISTANCING WAS USED 700 YEARS AGO. PLEASE KEEP YOUR DISTANCE AND TAKE THE NECESSARY PRECAUTIONS.
Thank you for reading,
Michael.
Comments are welcome.
I really appreciate your post. In this time of panic and great fear, we don’t seem to get the right information. I have learned more from your post about covid-19 than in any other newspaper or expert interview.
I am going to share your post with others and hopefully, many people will be educated on this matter.
Thanks for sharing
Hi Adyns68,
Thank you for your comments. The post was mainly on pneumonia, and the close similarities to covid-19. If you want to know more about the corona virus virus, and covid-19, I do have several posts relating to it. Appreciate you wanting wanting to share this post, but I think your friends will find the other posts more helpful.
Best wishes,
Michael
Few years ago, I began to do a lot of research and came across HERBAL HEALTHPOINT (ww w. herbalhealthpoint. c om) and their COPD HERBAL TREATMENT. After seeing positive reviews from other patients, I quickly started on the treatment, i experienced significant recovery from symptoms, including the shortness of breath. Its been over 2 years since treatment, i live symptom free
Hi Lisa,
Thank you for your comments. I am glad to hear you are symptom-free of COPD. I am a strong advocate of herbal remedies. COPD was/is one of the top ten global health risks in 2019.
Unfortunately, these statics are on the rise. 10 TEN THREATS TO GLOBAL HEALTH IN 2019. Respiratory diseases are on the rise and have been around for thousand’s of years. Of course,
if you were a smoker you have given that up. Lisa, I see two comments from you that are duplicates. No big deal. Herbal Healthpoint seems to be helping a lot of people. Stay healthy
and safe.
Best wishes,
Michael