What is Celiac Disease?
Blue indicates link
Celiac disease, sometimes called celiac sprue or gluten-sensitive enteropathy, is an immune reaction to eating gluten, a protein found in wheat, barley, and rye.
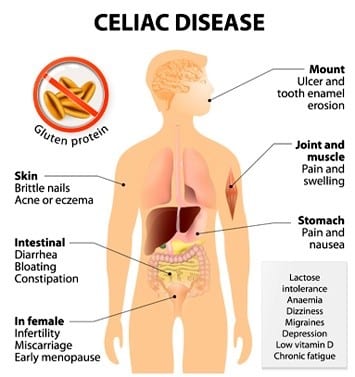
If you have celiac disease, eating gluten triggers an immune response in your small intestine. Over time, this reaction damages your small intestine’s lining and prevents it from absorbing some nutrients (malabsorption). The intestinal damage often causes diarrhea, fatigue, weight loss, bloating, and anemia, and can lead to serious complications.
In children, malabsorption can affect growth and development, besides causing the symptoms seen in adults.
There’s no cure for celiac disease — but for most people, following a strict gluten-free diet can help manage symptoms and promote intestinal healing.
Celiac disease is a serious autoimmune disease that occurs in genetically predisposed people where the ingestion of gluten leads to damage in the small intestine. It is estimated to affect 1 in 100 people worldwide. Two and one-half million Americans are undiagnosed and are at risk for long-term health complications.
When people with celiac disease eat gluten (a protein found in wheat, rye, and barley), their body mounts an immune response that attacks the small intestine. These attacks lead to damage to the villi, small finger-like projections that line the small intestine, that promote nutrient absorption. When the villi get damaged, nutrients cannot be absorbed properly into the body.
Celiac disease is hereditary, meaning that it runs in families. People with a first-degree relative with celiac disease (parent, child, sibling) have a 1 in 10 risk of developing celiac disease.
Celiac disease can develop at any age after people start eating foods or medicines that contain gluten. Left untreated, celiac disease can lead to additional serious health problems.
Symptoms:
The signs and symptoms of celiac disease can vary greatly and differ in children and adults. Digestive signs and symptoms for adults include:
- Diarrhea
- Fatigue
- Weight loss
- Bloating and gas
- Abdominal pain
- Nausea and vomiting
- Constipation
However, more than half the adults with celiac disease have signs and symptoms unrelated to the digestive system, including:
- Anemia, usually from iron deficiency
- Loss of bone density (osteoporosis) or softening of the bone (osteomalacia)
- Itchy, blistery skin rash (dermatitis herpetiformis)
- Mouth ulcers
- Headaches and fatigue
- Nervous system injury, including numbness and tingling in the feet and hands, possible problems with balance, and cognitive impairment
- Joint pain
- Reduced functioning of the spleen (hyposplenism)
Children
Children with celiac disease are more likely than adults to have digestive problems, including:
- Nausea and vomiting
- Chronic diarrhea
- Swollen belly
- Constipation
- Gas
- Pale, foul-smelling stools
The inability to absorb nutrients might result in:
- Failure to thrive for infants
- Damage to tooth enamel
- Weight loss
- Anemia
- Irritability
- Short stature
- Delayed puberty
- Neurological symptoms, including attention-deficit/hyperactivity disorder (ADHD), learning disabilities, headaches, lack of muscle coordination, and seizures
Dermatitis herpetiformis:
Gluten intolerance can cause this itchy, blistering skin disease. The rash usually occurs on the elbows, knees, torso, scalp, and buttocks. This condition is often associated with changes to the lining of the small intestine identical to those of celiac disease, but the skin condition might not cause digestive symptoms.
Doctors treat dermatitis herpetiformis with a gluten-free diet medication, or both, to control the rash.
When to see a doctor:
Consult your doctor if you have diarrhea or digestive discomfort that lasts for more than two weeks. Consult your child’s doctor if your child is pale, irritable, or failing to grow or has a potbelly and foul-smelling, bulky stools.
Be sure to consult your doctor before trying a gluten-free diet. If you stop or even reduce the amount of gluten you eat before you’re tested for celiac disease, you can change the test results.
Celiac disease tends to run in families. If someone in your family has the condition, ask your doctor if you should be tested. Also ask your doctor about testing if you or someone in your family has a risk factor for celiac disease, such as type 1 diabetes.
Diagnosis:
In recent years, an improvement in the overall level of awareness about celiac disease and associated conditions has allowed individuals and health professionals to better suspect and screen for celiac disease. This is particularly true for those groups at high risk.
Celiac disease can be diagnosed through a combination of:
- Blood tests
- Small-bowel biopsy
- Recovery from the symptoms while following a gluten-free diet
Small-bowel biopsy remains the ‘gold standard’ test for celiac disease detection. Testing for the disease should take place before an individual starts a gluten-free diet since the removal of gluten from the diet would interfere with a practitioner’s ability to detect the disease. After 6 to 12 months of maintaining a strict gluten-free diet, symptoms should disappear, blood tests for the disease should become negative, and any small bowel injury should heal completely. It will be important for celiac patients to regularly follow up with their family doctor on their progress in treating the disease.
Causes:
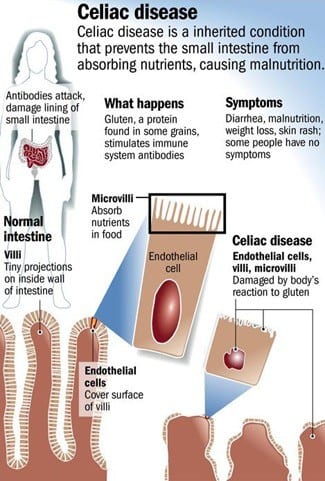
Your genes combined with eating foods with gluten and other factors can contribute to celiac disease, but the precise cause isn’t known. Infant-feeding practices, gastrointestinal infections, and gut bacteria might contribute, as well. Sometimes celiac disease becomes active after surgery, pregnancy, childbirth, viral infection, or severe emotional stress.
When the body’s immune system overreacts to gluten in food, the reaction damages the tiny, hairlike projections (villi) that line the small intestine. Villi absorb vitamins, minerals, and other nutrients from the food you eat. If your villi are damaged, you can’t get enough nutrients, no matter how much you eat.
Risk factors:
Celiac disease tends to be more common in people who have:
- A family member with celiac disease or dermatitis herpetiformis
- Type 1 diabetes
- Down syndrome or Turner syndrome
- Autoimmune thyroid disease
- Microscopic colitis (lymphocytic or collagenous colitis)
- Addison’s disease
Complications:
Untreated, celiac disease can cause:
- Malnutrition. This occurs if your small intestine can’t absorb enough nutrients. Malnutrition can lead to anemia and weight loss. In children, malnutrition can cause slow growth and short stature.
- Bone weakening. Malabsorption of calcium and vitamin D can lead to a softening of the bone (osteomalacia or rickets) in children and a loss of bone density (osteopenia or osteoporosis) in adults.
- Infertility and miscarriage. Malabsorption of calcium and vitamin D can contribute to reproductive issues.
- Lactose intolerance. Damage to your small intestine might cause you abdominal pain and diarrhea after eating or drinking dairy products that contain lactose. Once your intestine has healed, you might be able to tolerate dairy products again.
- Cancer. People with celiac disease who don’t maintain a gluten-free diet have a greater risk of developing several forms of cancer, including intestinal lymphoma and small bowel cancer.
- Nervous system problems. Some people with celiac disease can develop problems such as seizures or a disease of the nerves in the hands and feet (peripheral neuropathy).
Nonresponsive celiac disease:
Some people with celiac disease don’t respond to what they consider to be a gluten-free diet. Nonresponsive celiac disease is often due to contamination of the diet with gluten. Working with a dietitian can help you learn how to avoid gluten.
People with non-responsive celiac disease might have:
- Bacteria in the small intestine (bacterial overgrowth)
- Microscopic colitis
- Poor pancreas function (pancreatic insufficiency)
- Irritable bowel syndrome
- Difficulty digesting sugar found in dairy products (lactose), table sugar (sucrose), or a type of sugar found in honey and fruits (fructose)
- Refractory celiac disease
Refractory celiac disease:
In rare instances, the intestinal injury of celiac disease doesn’t respond to a strict gluten-free diet. This is known as refractory celiac disease. If you still have signs and symptoms after following a gluten-free diet for six months to one year, you might need further testing to look for other explanations for your symptoms.
Treatment:
At present, there is no permanent cure for CD but it can be effectively treated with a gluten-free diet. The adherence to the gluten-free diet must be STRICT and LIFE-LONG. A gluten-free diet can be challenging and complicated and a consultation with a registered dietitian with expertise in a gluten-free diet is essential.
Individuals with celiac CD need to be vigilant about hidden sources of gluten and cross-contamination in food products. Careful label reading each time when buying products is important.
Since celiac disease is a chronic disorder, regular long-term follow-up with the physician and dietitian is recommended.
The only proper method of treatment for the autoimmune condition related to gluten is a restrictive gluten-free diet. This includes the avoidance of gluten-containing foods as well as those that may come into contact with them. Additionally, cross-reactive edibles are also foods to avoid with celiac disease if symptoms still persist once a gluten-free diet has been started, as products like sugars and dairy may further contribute to symptom formation.
However, it is abundantly important that no dietary changes be made until a celiac disease diagnosis has been made following the appropriate medical tests. This is because if a person commits to eliminating gluten before having lab work done in order to confirm or rule out a celiac disease diagnosis, the test results can be markedly altered and can return incorrect results. Therefore, while diet is an important consideration and the only treatment for celiac disease, it is best only implemented following the advice of a healthcare provider.
Celiac Disease Diet Plan:

Foods to Avoid:
Wheat:
Wheat is one of the major grains of any diet, irrespective of the place. It is the most common food containing gluten, so in spite of its cultural importance, it has to be avoided.
Barley:
Barley is another grain containing gluten. Therefore, people with celiac disease should avoid it at all costs.
Bulgur:
Bulger is a cereal made from the parboiled groats of several wheat species. Although an ideal food for people aiming for weight loss, it is best avoided for people suffering from gluten intolerance.
Oats:
Oats themselves don’t contain gluten but are often processed in facilities that produce gluten-containing grains and may be contaminated. Therefore, be wary of store-bought oats.
Rye:
Rye is a grass grown extensively as a grain, a cover crop, and a forage crop. It is a member of the wheat tribe and is closely related to barley and wheat, therefore it should be avoided.
Seitan:
Often called “wheat protein,” “wheat meat” or “wheat gluten,” seitan (pronounced say-tahn) has a look and texture shockingly similar to meat when it’s cooked, and its alternative namesakes are quite fitting since it’s made from gluten, the main protein found in wheat. It is a complete no-no for people with celiac disease.
Barley malt:
Malted barley is the source of the sugars (principally maltose) which are fermented into beer. The malting process allows the grain to partially germinate, making the seed’s resources available to the brewer.
Chicken broth:
Commercially prepared chicken broth can contain gluten since it is a good thickening agent. Therefore, avoid it and prepare chicken broth at home.
Malt vinegar:
Malt vinegar is not gluten-free because it contains malt which contains barley. The starting material for malt vinegar can include barley, rye, or wheat. Because these kinds of vinegar are made from alcohol that has been fermented and not distilled they are not gluten-free.
Salad dressings:
Again, certain commercially prepared salad dressings might contain gluten, so just check the labels carefully before buying them.
Burgers:
Burger bread is made from wheat, so they are not gluten-free either. However, certain joints might make vegan, gluten-free burgers, so just make sure you check their specifications before ordering your favorite burger.
Soy sauce:
Soy sauce is made with fermented wheat. Flour is often used as a thickener in soups and sauces. An easy solution is to bring your own gluten-free soy sauce.
Seasonings and spice mixes:
Gluten is extensively used in seasonings and spices, so it is no wonder that some people just can’t identify where their gluten intolerance comes from. Make sure you check the labels carefully.
Soba noodles:
Many packaged soba noodles contain wheat flour, so check for the ones that contain buckwheat flour.
Condiments:
A lot of commercially prepared condiments actually contain gluten, so be wary of that.
Graham flour:
Commercially made graham flour contains gluten. The alternative is to make your own graham flour at home.
Kamut:
Kamut is not among these alternatives, however, as it is an ancient relative of durum wheat. Cereals, bread, and baked goods made with Kamut contain gluten.
Matzo:
The most common form of knaidel, known as the matzo ball, is made from unleavened matzo meal and served in chicken soup in some places. Matzo meal contains wheat, making it unsuitable for those on a gluten-free diet.
Semolina:
People with celiac disease can safely eat many common plants, seeds, grains, bowls of cereal, and flour, including corn, polenta, potatoes, rice, and soya. However, they should avoid semolina as it contains gluten.
Like other forms of wheat, spelt contains gluten protein, and therefore, isn’t safe for those of us who have celiac disease or non-celiac gluten sensitivity. The idea that spelt, spelt flour, and baked goods made with spelt are safe on the gluten-free diet is one of the oldest gluten-free urban myths.
Cracked wheat:
Cracked wheat, or dahlia, is a great option for those aiming for weight loss, but it should be avoided by people with celiac disease.
Beer:
Unfortunately, celiac disease does make beer drinking impossible, unless options that are gluten-free are used instead of traditional brews. There are some gluten-free beers that exist, but they are often more difficult to find and can be pricey. But, based on its malt and barley base, beer is a big no-no for celiac disease sufferers and those with gluten intolerance.
Lunch Meat:
It may seem odd that lunchtime proteins are considered foods to avoid with celiac disease. However, this is not because of their meaty composition, but rather the processing of the lunch meats that can often add in gluten-containing elements. It is best that lunch meats that do not indicate that they are gluten-free be avoided by patients affected by Celiac disease.
Milk Chocolate:
The sweetened candy bar base contains two foods to avoid with celiac disease, sugar, and dairy, which can make existing symptoms worse or bring about new ones. Many people who are unable to ingest gluten also have reactions to protein, and sugar just worsens this. Sugar is one of the most common added contributors to celiac disease symptoms. Thus, milk chocolate that combines both can be even more problematic for Celiac sufferers.
Potatoes:
Potatoes are a starchy part of many healthy diets, but they, alongside other members of the nightshade family tree, can cause digestive troubles for celiac sufferers. Potatoes are high in saponins that can create indigestion-like symptoms from creating extremely tiny intestinal perforations. For existing food sensitivity sufferers, this can lead to worsening or unbearable symptoms.
Overly Processed and Refined Foods:
Over-processed ingestible foods are foods to avoid with celiac disease because their digestion is difficult even in healthy people. They are also packed with sugar which is a cross reactor to celiac disease and can worsen symptoms. Artificial sweeteners are no substitute for high sugar foods though as they come with their own set of side effects for celiac sufferers.
French Fries and Potato Chips:
There are some variants of the favorite side dishes that are gluten-free. However, regular potato chips and fries are not celiac disease-friendly and can lead to symptoms when gluten is consumed.
Foods That Are Gluten-Free.
It might initially seem like a daunting task to compile a list of foods that are gluten-free, especially after reading this list. But worry not, because we are going to make a shortlist of foods that are gluten-free and healthy. They are common foods and self-explanatory, so we are going to just present the names:
- fruits and vegetables
- beans
- seeds
- legumes
- nuts
- eggs
- dairy products
- oils and certain types of vinegar
- corn
- rice
- fish
- lean beef
- chicken
- seafood
All these foods are free from wheat, which contains the protein gluten; therefore they are ideal for those suffering from celiac disease. You can include these foods in your diet without any worry.
Here are some of the healthiest gluten-free foods:
Fruits and vegetables not only are an important part of any healthy diet, but they are also naturally gluten-free. They provide valuable essential nutrients, fiber, and antioxidants. Furthermore, eating them will help raise immune function.
Healthy Fats
Try avocado, virgin coconut, grape seed, virgin olive, flaxseed, avocado, hemp, and pumpkin oils.
Nuts and Seeds
These are also good sources of healthy fats. Furthermore, they’re high in fiber, omega-3 fats, and minerals. Try almonds, walnuts, flax seeds, hemp, chia seeds, pumpkin, sesame, and sunflower seeds.
Legumes, Beans, and Gluten-Free Whole Grains
These include all beans, wild or brown rice, gluten-free oats, buckwheat, quinoa, teff, and amaranth. Generally speaking, it’s best to properly prepare beans and grains by soaking, sprouting, and fermenting them. Sprouting them helps improve nutrient intake. Additionally, it reduces the presence of anti-nutrients that can cause digestive issues. Sprouting also makes proteins more digestible.
Gluten-Free Flours
These include baking flours. You’ll want to check out brown rice flour, potato or cornmeal, or quinoa flour. You might also like almond flour, coconut flour, chickpea flour, tapioca flour/starch, cassava, and other gluten-free blends. In particular, make sure the product you purchase is certified as gluten-free. It should state so on the label.
Gluten-Free Alcohol
If you want to consume alcohol, go for something that does not have gluten in it. Most, but not all wines and hard liquors are good options.
Other Gluten-Free Condiments, Spices, and Herbs
This includes real sea salt, cocoa, and apple cider vinegar. It also includes fresh herbs and spices, however, make sure they are labeled as gluten-free. You can also try raw honey and organic stevia.
Natural Remedies and Herbs for Celiac Disease
Though there is no cure for celiac disease, there are a number of celiac disease natural remedies to help ease symptoms. If you’re looking for a celiac disease natural treatment try the following herbal remedies:
- Aloe Vera – Aloe vera has natural anti-inflammatory health benefits that can help to treat and heal the damage done to the small intestine.
- Dandelion – With natural anti-inflammatory benefits, dandelion is a celiac disease natural remedy to help treat digestive problems.
- Papain -Papain supplements help to stimulate digestive enzymes which can help to prevent autoimmune attacks from celiac disease.
- Horsetail – Horsetail is a natural anti-inflammatory that directly targets the digestive system to help alleviate celiac disease symptoms.
- Paprika – The anti-inflammatory health benefits of paprika make it an important celiac disease natural treatment to ease painful digestive symptoms.
- Echinacea – Echinacea is an effective celiac disease natural remedy because it is an immune booster that helps to treat the inflammation in the intestinal lining that occurs during an immune attack from gluten consumption.
Diet is the most crucial factor in living with Celiac Disease. I realize how restricted your diet has to be, but it is so important.
Please Always Check With Your Doctor If You Are Suffering From Celiac Disease Symptoms.
Thank you for reading.
Michael.
Comments are welcome.
Such a great and comprehensive review with everything you need to know about celiac disease. My mum started developing a mild case of it and, considering the taste of gluten free pasta, it was quite sad to see! But with a healthy diet with more plant based foods and complex carbohydrates we were able to turn it around.
Hi Kit,
Thank you for your comments. I am glad your mum was able to turn things around.
Best wishes,
Michael
What an exemplary piece of information. It is a must read for a person who is suffering from this disease, or knows someone who is suffering from it. The author has written about this topic so well. Every detail about it has been covered perfectly. All the aspects, that are so important, have been perfectly included. Everything, starting from the description of the disease, symptoms, treatments; prevention, has been highlighted flawlessly. I have forwarded the link to the page to a few of my family members! The author has done a really good job here.
Hi Kiran,
Thank you for your comments.
Best wishes,
Michael
What an exemplary piece of information. It is a must-read for a person who is suffering from this disease or knows someone who is suffering from it. The author has written about this topic so well. Every detail about it has been covered perfectly. All the aspects, that are so important, have been perfectly included. Everything, starting from the description of the disease, symptoms, treatments; prevention, has been highlighted flawlessly. I have forwarded the link to the page to a few of my family members! The author has done a really good job here.
Hi Samantha,
Thank you for your comments. Much appreciated. Also thank you for forwarding my link to your family members.
Best wishes,
Michael
Hey nice article you have there. This is the exact article a friend of mine will be pleased to have, their child has been combating with Celiac disease for some time now, having gone through this article to see the recommendations, medications and the type of diet to engage in such situation, I am convinced it will be helpful to them, I will definitely refer the to this article for more clarity. Regards.
Hi,
Thank you for your comments. I am glad you found this article to be helpful for your friend. I appreciate you sharing it.
Best wishes,
Michael