What is Prostate Cancer?
Blue indicates link
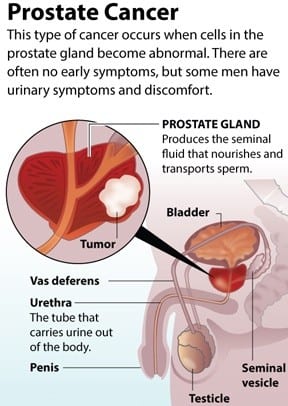
Prostate cancer starts in the cells of the prostate. A cancerous (malignant) tumor is a group of cancer cells that can grow into and destroy nearby tissue. It can also spread (metastasize) to other parts of the body. Prostate cancer is the most common cancer in Canadian men. Many older men have this disease without knowing it. It usually grows slowly and can often be completely removed or successfully managed when it is diagnosed. Older men with prostate cancer often die of other causes.
The prostate is part of a man’s reproductive and urinary systems. It is a walnut-sized gland just below the bladder and in front of the rectum. It surrounds part of the urethra, which is the tube that carries urine and semen through the penis. The prostate makes mucus and prostatic fluid, which mixes with sperm and other fluids to make semen.
Personal Note:
I was asked to go for a prostate exam but felt awkward and even a bit embarrassed. When weighing the odds I realized I was being childlike and a bit foolish. I mean this is one of the few types of cancer that can be cured or eliminated. Please if you are anything like me, put all those things aside and do get checked out. It was a burden lifted off my shoulders, once I went through the procedure which I imagined to be more embarrassing than what it was.
What Is The Prostate?
The prostate (or prostate gland) is part of a man’s reproductive and urinary systems. It is about the size of a walnut in younger men, but it starts to get larger when men reach their late 40’s and early 50’s.
The prostate is deep inside a man’s pelvis, below the bladder, and in front of the rectum. It wraps around the upper part of the urethra (called the prostatic urethra). The urethra is a tube that carries urine from the bladder, through the prostate and penis, and out of the body.
The prostate is close to parts of the digestive, urinary, and reproductive systems. As a result, prostate cancer and its treatments can affect these systems. For example, an enlarged prostate can press on and block the urethra, which can cause problems urinating. Radiation therapy for prostate cancer can affect the rectum and cause bowel problems. Surgery to remove prostate cancer can affect nerves that supply the bladder and penis, which can affect urinary and sexual function.
What is Prostate Cancer?
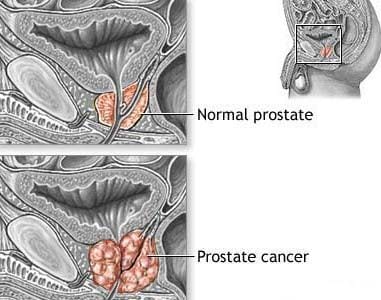
Prostate cancer is the development of cancer cells in the prostate gland (a gland that produces fluid for semen). It is the most common cancer in men; some cancers grow very slowly while others are very aggressive and spread quickly to other organs.
Prostate cancer is cancer that occurs in the prostate — a small walnut-shaped gland in men that produces the seminal fluid that nourishes and transports sperm.
Like all cancers, prostate cancer begins when a mass of cells has grown out of control and begins invading other tissues. Cells become cancerous due to the accumulation of defects, or mutations, in their DNA.
Most of the time, cells are able to detect and repair DNA damage. If a cell is severely damaged and cannot repair itself, it undergoes so-called programmed cell death or apoptosis. Cancer occurs when damaged cells grow, divide, and spread abnormally instead of self-destructing as they should.
Prostate cancer is one of the most common types of cancer in men. Usually, prostate cancer grows slowly and is initially confined to the prostate gland, where it may not cause serious harm. However, while some types of prostate cancer grow slowly and may need minimal or even no treatment, other types are aggressive and can spread quickly.
Prostate cancer that’s detected early — when it is still confined to the prostate gland — has a better chance of successful treatment.
Symptoms:
Prostate cancer may cause no signs or symptoms in its early stages.
Prostate cancer that’s more advanced may cause signs and symptoms such as:
- Trouble urinating
- Decreased force in the stream of urine
- Blood in semen
- Discomfort in the pelvic area
- Bone pain
- Erectile dysfunction
Causes:
Prostate gland:
It’s not clear what causes prostate cancer.
Doctors know that prostate cancer begins when some cells in your prostate become abnormal. Mutations in the abnormal cells’ DNA cause the cells to grow and divide more rapidly than normal cells do. The abnormal cells continue living when other cells die. The accumulating abnormal cells form a tumor that can grow to invade nearby tissue. Some abnormal cells can also break off and spread (metastasize) to other parts of the body.
Risk factors:
Factors that can increase your risk of prostate cancer include:
- Age. Your risk of prostate cancer increases as you age.
- Race. For reasons not yet determined, black men carry a greater risk of prostate cancer than men of other races. In black men, prostate cancer is also more likely to be aggressive or advanced.
- Family history. If men in your family have had prostate cancer, your risk may be increased. Also, if you have a family history of genes that increase the risk of breast cancer (BRCA1 or BRCA2) or a very strong family history of breast cancer, your risk of prostate cancer may be higher.
- Obesity. Obese men diagnosed with prostate cancer may be more likely to have an advanced disease that’s more difficult to treat.
Complications:
Complications of prostate cancer and its treatments include:
- Cancer that spreads (metastasizes). Prostate cancer can spread to nearby organs, such as your bladder, or travel through your bloodstream or lymphatic system to your bones or other organs. Prostate cancer that spreads to the bones can cause pain and broken bones. Once prostate cancer has spread to other areas of the body, it may still respond to treatment and may be controlled, but it’s unlikely to be cured.
- Incontinence. Both prostate cancer and its treatment can cause urinary incontinence. Treatment for incontinence depends on the type you have, how severe it is, and the likelihood it will improve over time. Treatment options may include medications, catheters, and surgery.
- Erectile dysfunction. Erectile dysfunction can result from prostate cancer or its treatment, including surgery, radiation, or hormone treatments. Medications, vacuum devices that assist in achieving an erection, and surgery are available to treat erectile dysfunction.
Prevention:
You can reduce your risk of prostate cancer if you:
- Choose a healthy diet full of fruits and vegetables. Avoid high-fat foods and instead focus on choosing a variety of fruits, vegetables, and whole grains. Fruits and vegetables contain many vitamins and nutrients that can contribute to your health. Whether you can prevent prostate cancer through diet has yet to be conclusively proven. However, eating a healthy diet with a variety of fruits and vegetables can improve your overall health.
- Choose healthy foods over supplements. No studies have shown that supplements play a role in reducing your risk of prostate cancer. Instead, choose foods that are rich in vitamins and minerals so that you can maintain healthy levels of vitamins in your body.
- Exercise most days of the week. Exercise improves your overall health, helps you maintain your weight, and improves your mood. There is some evidence that men who don’t exercise have higher PSA levels, while men who exercise may have a lower risk of prostate cancer. Try to exercise most days of the week. If you’re new to exercise, start slow, and work your way up to more exercise time each day.
- Maintain a healthy weight. If your current weight is healthy, work to maintain it by exercising most days of the week. If you need to lose weight, add more exercise, and reduce the number of calories you eat each day. Ask your doctor for help to create a plan for healthy weight loss.
- Talk to your doctor about the increased risk of prostate cancer. Men with a high risk of prostate cancer may consider medications or other treatments to reduce their risk. Some studies suggest that taking 5-alpha reductase inhibitors, including finasteride (Propecia, Proscar) and dutasteride (Avodart), may reduce the overall risk of developing prostate cancer. These drugs are used to control prostate gland enlargement and hair loss in men. However, some evidence indicates that men taking these medications may have an increased risk of getting a more serious form of prostate cancer (high-grade prostate cancer). If you’re concerned about your risk of developing prostate cancer, talk with your doctor.
By the way:
There are many myths about why prostate cancer develops. However, there is no evidence that “too much sex,” masturbation, benign prostatic hyperplasia (BPH), or a vasectomy increases the risk or causes prostate cancer. Current research is investigating if STDs, prostatitis, or alcohol use increase the risk of developing prostate cancer.
Note:
Talk to your Doctor. There are different tests that can be done to perform a diagnosis.
The Stages of Prostate Cancer:
In terms of prostate cancer, the cancer stages are as follows:
- Stage I: The cancer is small and still contained within the prostate gland.
- Stage II: The cancer is more advanced, but is still confined within the prostate gland.
- Stage III: Cancer has spread to the outer part of the prostate and to the nearby seminal vesicles.
- Stage IV: Cancer has spread to lymph nodes, other nearby organs, or tissues such as the rectum or bladder, or to distant sites such as the lungs or bones.
- Aggressive prostate cancer often reaches stage IV but others that are less aggressive may never progress past stage I, II, or III.
Screening for prostate cancer:
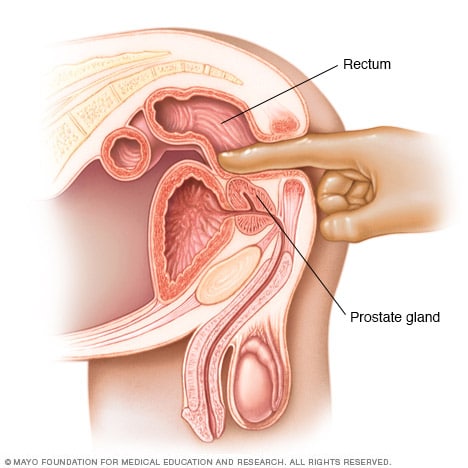
Digital rectal exam:
Whether to test healthy men with no symptoms for prostate cancer is controversial. Medical organizations don’t agree on the issue of screening and whether it delivers benefits.
Some medical organizations recommend men consider prostate cancer screening in their 50s, or sooner for men who have risk factors for prostate cancer.
Discuss your particular situation and the benefits and risks of screening with your doctor. Together, you can decide whether prostate cancer screening is right for you.
Prostate screening tests might include:
- Digital rectal exam (DRE). During a DRE, your doctor inserts a gloved, lubricated finger into your rectum to examine your prostate, which is adjacent to the rectum. If your doctor finds any abnormalities in the texture, shape, or size of the gland, you may need further tests.
- Prostate-specific antigen (PSA) test. A blood sample is drawn from a vein in your arm and analyzed for PSA, a substance that’s naturally produced by your prostate gland. It’s normal for a small amount of PSA to be in your bloodstream. However, if a higher-than-normal level is found, it may indicate prostate infection, inflammation, enlargement, or cancer.
PSA testing combined with DRE helps identify prostate cancers at their earliest stages. Hence, the debate continues surrounding prostate cancer screening.
Diagnosing prostate cancer:
If a DRE or PSA test detects an abnormality, your doctor may recommend further tests to determine whether you have prostate cancer, such as:
- Ultrasound. If other tests raise concerns, your doctor may use transrectal ultrasound to further evaluate your prostate. A small probe, about the size and shape of a cigar, is inserted into your rectum. The probe uses sound waves to create a picture of your prostate gland.
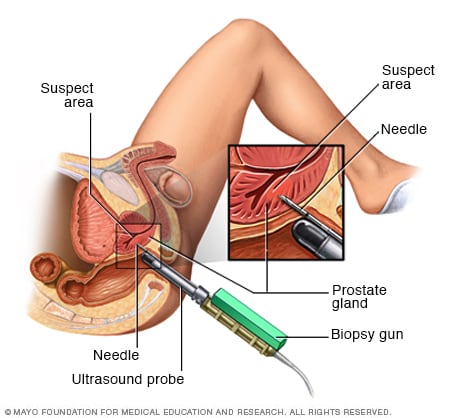
- Collecting a sample of prostate tissue. If initial test results suggest prostate cancer, your doctor may recommend a procedure to collect a sample of cells from your prostate (prostate biopsy). A prostate biopsy is often done using a thin needle that’s inserted into the prostate to collect tissue. The tissue sample is analyzed in a lab to determine whether cancer cells are present.
- MRI fusion. While still being developed worldwide, MRI fusion to assist in prostate biopsy and diagnosis is being used more and more.
Determining how far cancer has spread:
Transrectal biopsy of the prostate:
Once a prostate cancer diagnosis has been made, your doctor works to determine the extent (stage) of cancer. If your doctor suspects your cancer may have spread beyond your prostate, one or more of the following imaging tests may be recommended:
- Bone scan
- Ultrasound
- Computerized tomography (CT) scan
- Magnetic resonance imaging (MRI)
- Positron emission tomography (PET) scan
Immediate treatment may not be necessary:
For men diagnosed with low-risk prostate cancer, treatment may not be necessary right away. Some men may never need treatment. Instead, doctors sometimes recommend active surveillance.
In active surveillance, regular follow-up blood tests, rectal exams, and possibly biopsies may be performed to monitor the progression of your cancer. If tests show your cancer is progressing, you may opt for a prostate cancer treatment such as surgery or radiation.
Active surveillance may be an option for cancer that isn’t causing symptoms, is expected to grow very slowly, and is confined to a small area of the prostate. Active surveillance may also be considered for someone who has another serious health condition or who is of an advanced age that makes cancer treatment more difficult.
Active surveillance carries a risk that cancer may grow and spread between checkups, making cancer less likely to be cured.
Conclusion:
Please do not take chances when it comes to your life. There are several ways of dealing with Prostate Cancer when you have it diagnosed in its early stages. I do not find the necessity of listing the different procedures as we all are individuals. What works for one person may not be the best choice for someone else.
If you are in your 40’s or 50’s please go for that examination.
Thank you for reading,
Michael
Comments are welcome.
Thank you for your post. It is useful for men with advanced age and you raise the awareness of prostate cancer. It is a common cancer among men. I have friend died of prostate cancer recently.
I particularly like you description on prevention. It sounds easy for most of men since we just need to have healthy diet (with a lot of fruits and vegetables), exercise, and maintain optimal weight.
It is good idea to have preventive measures if you think you are in high risk of this cancer. Of course you need to get your doctor’s advice before taking any medication of preventing prostate cancer.
It is kind of you sharing this useful information with us, which has the potential of saving life.
Hi Anthony,
Thank you for your comments. I think that when men reach the age of 40 and above, if not sooner should get checked out for prostate cancer. No one has to die from this form of cancer. I am sorry to hear about your friend.
Best wishes,
Michael
This has been a very helpful post. You have described the symptoms and even addressed that childish Idea that some men have not wanting to go to the doctor to be checked.. It’s so much better to discover something on time.
The graphics also helped me understand were prostate is inside our body and which are its functions.
Hi Abel,
Thank you for your comments. You are absolutely right. Men have to get over that uncomfortable feeling, and have themselves checked. Better safe than sorry.
Best wishes,
Michael
Thanks on such an amazing post. It is very important for adults(MEN) to know what Proscate Cancer is all about. This article has just made me know the importance of eating good fruits and vegetables to keep you healthy and maintain good weight. I deeply appreciate you sharing this amazing and teaching article.
Hi Perryline,
Thank you for your comments. It is also a good idea to have yourself checked after you are in your 40’s.
Best wishes,
Michael