What is Asthma?
Blue indicates link
Asthma is a condition in which your airways narrow and swell and may produce extra mucus. This can make breathing difficult and trigger coughing, a whistling sound (wheezing) when you breathe out, and shortness of breath.
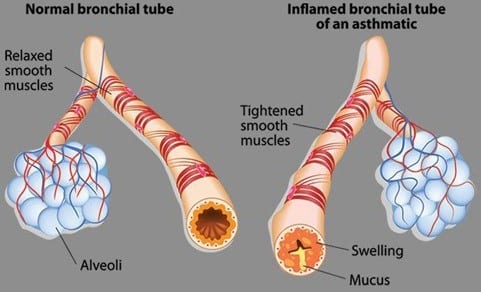
For some people, asthma is a minor nuisance. For others, it can be a major problem that interferes with daily activities and may lead to a life-threatening asthma attack.
Asthma can’t be cured, but its symptoms can be controlled. Because asthma often changes over time, it’s important that you work with your doctor to track your signs and symptoms and adjust your treatment as needed.
- Asthma is a persistent inflammatory disease.
- Asthma is incurable, but it can be regulated with proper measures.
- It is vital to recognize allergens and avoid exposure.
- Various medical treatments are available to ease “living with asthma.”
- Seeking advice from a medical practitioner is recommended to help control the underlying inflammation and the symptoms.
Symptoms
Asthma symptoms vary from person to person. You may have infrequent asthma attacks, have symptoms only at certain times — such as when exercising — or have symptoms all the time.
Asthma signs and symptoms include:
- Shortness of breath
- Chest tightness or pain
- Wheezing when exhaling, which is a common sign of asthma in children
- Trouble sleeping caused by shortness of breath, coughing or wheezing
- Coughing or wheezing attacks that are worsened by a respiratory virus, such as a cold or the flu
Signs that your asthma is probably worsening include:
- Asthma signs and symptoms that are more frequent and bothersome
- Increasing difficulty breathing, as measured with a device used to check how well your lungs are working (peak flow meter)
- The need to use a quick-relief inhaler more often
For some people, asthma signs and symptoms flare up in certain situations:
- Exercise-induced asthma, which may be worse when the air is cold and dry
- Occupational asthma, triggered by workplace irritants such as chemical fumes, gases, or dust
- Allergy-induced asthma is triggered by airborne substances, such as pollen, mold spores, cockroach waste, or particles of skin and dried saliva shed by pets (pet dander)
Why and when to see your doctor
- If you think you have asthma. If you have frequent coughing or wheezing that lasts more than a few days or any other signs or symptoms of asthma, see your doctor. Treating asthma early may prevent long-term lung damage and help keep the condition from getting worse over time.
- To monitor your asthma after diagnosis. If you know you have asthma, work with your doctor to keep it under control. Good long-term control helps you feel better from day to day and can prevent a life-threatening asthma attack.
- If your asthma symptoms get worse. Contact your doctor right away if your medication doesn’t seem to ease your symptoms or if you need to use your quick-relief inhaler more often. Don’t take more medication than prescribed without consulting your doctor first. Overusing asthma medication can cause side effects and may make your asthma worse.
- To review your treatment. Asthma often changes over time. Meet with your doctor regularly to discuss your symptoms and make any needed treatment adjustments.
Causes
It isn’t clear why some people get asthma and others don’t, but it’s probably due to a combination of environmental and inherited (genetic) factors.
Asthma triggers
Exposure to various irritants and substances that trigger allergies (allergens) can trigger signs and symptoms of asthma. Asthma triggers are different from person to person and can include:
- Airborne allergens, such as pollen, dust mites, mold spores, pet dander, or particles of cockroach waste
- Respiratory infections, such as the common cold
- Physical activity
- Cold air
- Air pollutants and irritants, such as smoke
- Certain medications, including beta-blockers, aspirin, and nonsteroidal anti-inflammatory drugs, such as ibuprofen (Advil, Motrin IB, others) and naproxen sodium (Aleve)
- Strong emotions and stress
- Sulfites and preservatives are added to some types of foods and beverages, including shrimp, dried fruit, processed potatoes, beer, and wine
- Gastroesophageal reflux disease (GERD), is a condition in which stomach acids back up into your throat
Risk factors
A number of factors are thought to increase your chances of developing asthma. They include:
- Having a blood relative with asthma, such as a parent or sibling
- Having another allergic condition, such as atopic dermatitis — which causes red, itchy skin — or hay fever — which causes a runny nose, congestion, and itchy eyes
- Being overweight
- Being a smoker
- Exposure to secondhand smoke
- Exposure to exhaust fumes or other types of pollution
- Exposure to occupational triggers, such as chemicals used in farming, hairdressing, and manufacturing
Complications
Asthma complications include:
- Signs and symptoms that interfere with sleep, work, and other activities
- Sick days from work or school during asthma flare-ups
- A permanent narrowing of the tubes that carry air to and from your lungs (bronchial tubes), which affects how well you can breathe
- Emergency room visits and hospitalizations for severe asthma attacks
- Side effects from long-term use of some medications used to stabilize severe asthma
The proper treatment makes a big difference in preventing both short-term and long-term complications caused by asthma.
Treatment

Prevention and long-term control are key to stopping asthma attacks before they start. Treatment usually involves learning to recognize your triggers, taking steps to avoid triggers, and tracking your breathing to make sure your medications are keeping symptoms under control. In case of an asthma flare-up, you may need to use a quick-relief inhaler.
Medications
The right medications for you depend on a number of things — your age, symptoms, asthma triggers, and what works best to keep your asthma under control.
Preventive, long-term control medications reduce the swelling (inflammation) in your airways that leads to symptoms. Quick-relief inhalers (bronchodilators) quickly open swollen airways that are limiting breathing. In some cases, allergy medications are necessary.
Long-term asthma control medications, generally taken daily, are the cornerstone of asthma treatment. These medications keep asthma under control on a day-to-day basis and make it less likely you’ll have an asthma attack. Types of long-term control medications include:
- Inhaled corticosteroids. These medications include fluticasone propionate (Flovent HFA, Flovent Diskus, Xhance), budesonide (Pulmicort Flexhaler, Pulmicort Respules, Rhinocort), ciclesonide (Alvesco), beclomethasone (Qvar Redihaler), mometasone (Asmanex HFA, Asmanex Twisthaler), and fluticasone furoate (Arnuity Ellipta). You may need to use these medications for several days to weeks before they reach their maximum benefit. Unlike oral corticosteroids, inhaled corticosteroids have a relatively low risk of serious side effects.
- Leukotriene modifiers. These oral medications — including montelukast (Singulair), zafirlukast (Accolate), and zileuton (Zyflo) — help relieve asthma symptoms. Montelukast has been linked to psychological reactions, such as agitation, aggression, hallucinations, depression, and suicidal thinking. Seek medical advice right away if you experience any of these reactions.
- Combination inhalers. These medications — such as fluticasone-salmeterol (Advair HFA, Airduo Digihaler, others), budesonide-formoterol (Symbicort), formoterol-mometasone (Dulera), and fluticasone furoate-vilanterol (Breo Ellipta) — contain a long-acting beta-agonist along with a corticosteroid.
- Theophylline. Theophylline (Theo-24, Elixophyllin, Theochron) is a daily pill that helps keep the airways open by relaxing the muscles around the airways. It’s not used as often as other asthma medications and requires regular blood tests.
Quick-relief (rescue) medications are used as needed for rapid, short-term symptom relief during an asthma attack. They may also be used before exercise if your doctor recommends it. Types of quick-relief medications include:
- Short-acting beta-agonists. These inhaled, quick-relief bronchodilators act within minutes to rapidly ease symptoms during an asthma attack. They include albuterol (ProAir HFA, Ventolin HFA, others) and levalbuterol (Xopenex, Xopenex HFA). Short-acting beta-agonists can be taken using a portable, hand-held inhaler or a nebulizer, a machine that converts asthma medications to a fine mist. They’re inhaled through a face mask or mouthpiece.
- Anticholinergic agents. Like other bronchodilators, ipratropium (Atrovent HFA) and tiotropium (Spiriva, Spiriva Respimat) act quickly to immediately relax your airways, making it easier to breathe. They’re mostly used for emphysema and chronic bronchitis but can be used to treat asthma.
- Oral and intravenous corticosteroids. These medications — which include prednisone (Prednisone Intensol, Rayos) and methylprednisolone (Medrol, Depo-Medrol, Solu-Medrol) — relieve airway inflammation caused by severe asthma. They can cause serious side effects when used long-term, so these drugs are used only on a short-term basis to treat severe asthma symptoms.
If you have an asthma flare-up, a quick-relief inhaler can ease your symptoms right away. But you shouldn’t need to use your quick-relief inhaler very often if your long-term control medications are working properly.
Keep a record of how many puffs you use each week. If you need to use your quick-relief inhaler more often than your doctor recommends, see your doctor. You probably need to adjust your long-term control medication.
Allergy medications may help if your asthma is triggered or worsened by allergies. These include:
- Allergy shots (immunotherapy). Over time, allergy shots gradually reduce your immune system reaction to specific allergens. You generally receive shots once a week for a few months, then once a month for a period of three to five years.
- Biologics. These medications — which include omalizumab (Xolair), mepolizumab (Nucala), dupilumab (Dupixent), reslizumab (Cinqair), and benralizumab (Fasenra) — are specifically for people who have severe asthma.
Prevention
While there’s no way to prevent asthma, you and your doctor can design a step-by-step plan for living with your condition and preventing asthma attacks.
- Follow your asthma action plan. With your doctor and health care team, write a detailed plan for taking medications and managing an asthma attack. Then be sure to follow your plan. Asthma is an ongoing condition that needs regular monitoring and treatment. Taking control of your treatment can make you feel more in control of your life.
- Get vaccinated for influenza and pneumonia. Staying current with vaccinations can prevent flu and pneumonia from triggering asthma flare-ups.
- Identify and avoid asthma triggers. A number of outdoor allergens and irritants — ranging from pollen and mold to cold air and air pollution — can trigger asthma attacks. Find out what causes or worsens your asthma, and take steps to avoid those triggers.
- Monitor your breathing. You may learn to recognize warning signs of an impending attack, such as slight coughing, wheezing, or shortness of breath. But because your lung function may decrease before you notice any signs or symptoms, regularly measure and record your peak airflow with a home peak flow meter. A peak flow meter measures how hard you can breathe out. Your doctor can show you how to monitor your peak flow at home.
- Identify and treat attacks early. If you act quickly, you’re less likely to have a severe attack. You also won’t need as much medication to control your symptoms. When your peak flow measurements decrease and alert you to an oncoming attack, take your medication as instructed. Also, immediately stop any activity that may have triggered the attack. If your symptoms don’t improve, get medical help as directed in your action plan.
- Take your medication as prescribed. Don’t change your medications without first talking to your doctor, even if your asthma seems to be improving. It’s a good idea to bring your medications with you to each doctor’s visit. Your doctor can make sure you’re using your medications correctly and taking the right dose.
- Pay attention to increasing quick-relief inhaler use. If you find yourself relying on your quick-relief inhaler, such as albuterol, your asthma isn’t under control. See your doctor about adjusting your treatment.
Always consult your doctor first if you feel any symptoms of asthma.
Herbal Remedies For Asthma
1. Oregano
Oregano is a powerful herb for treating asthma. Along with anti-inflammatory properties, it contains carvacrol, flavonoids, and terpenes that work as lung-cleansing elements.
This herb can reduce inflammation of the respiratory tract and bronchial tubes, thus providing relief from asthma symptoms.
- Drink 2 to 3 cups of oregano tea daily when suffering from asthma. To make the tea, steep 3 teaspoons of oregano in 1 cup of hot water for 5 to 10 minutes. Strain, add honey as per taste, and drink it.
- Alternatively, take 1 tablespoon of juice extracted from fresh oregano leaves a few times a day to relieve asthma symptoms and chronic coughs.
2. Ginkgo Biloba
Ginkgo biloba contains an antihistamine and anti-inflammatory properties that help treat asthma.
A 2007 study published in the Journal of Huazhong University of Science and Technology (Medical Sciences) found that extracts of this herb helped decrease the infiltration of inflammatory cells in the asthmatic airway and relieved airway inflammation.
It is readily available in the market in supplement form.
Note: Ginkgo biloba may interact with certain medications, so consult your doctor before taking this supplement.
3. Ginger
Another well-known herb used for treating asthma is ginger. It has anti-inflammatory properties that help reduce airway inflammation and inhibit airway contraction.
According to a study presented at the American Thoracic Society 2013 International Conference, several compounds in ginger may help relax the smooth muscle tissue in the airways, which is constricted during asthma attacks. Further studies, however, are still required
- Drink 2 to 3 cups of ginger tea daily. To make the tea, add 1 inch of ginger (cut into small pieces) to a pot of boiling water. Simmer for 10 minutes, strain, allow it to cool, and drink it.
- Another option is to mix equal amounts of ginger juice, pomegranate juice, and honey. Consume 1 tablespoon of this mixture 2 or 3 times a day.
- You can also take ginger supplements after consulting your doctor.
4. Garlic
According to traditional Chinese medicine, garlic is a popular medicinal herb used to treat asthma. Its anti-inflammatory properties help clear congestion in the lungs. In addition, its antibiotic and antiviral properties help boost immunity and fight infections that can trigger asthma.
- Boil 2 to 3 garlic cloves in ¼ cup of milk. Allow it to cool to room temperature and drink it once daily.
- Alternatively, eat 2 garlic cloves with 1 teaspoon each of raw, unfiltered apple cider vinegar and honey each morning before breakfast.
- Another option is to eat 1 to 2 crushed raw garlic cloves daily to boost immunity and prevent asthma attacks.
- You can also take garlic supplements after consulting your doctor.
5. Slippery Elm
Slippery elm is another effective herb for asthma. It has anti-inflammatory properties that help thin the mucus that clogs the airways.
It also provides relief from coughing and tightening of the chest. In addition to asthma, it can help treat bronchitis, sore throats, and coughs.
- Add 2 teaspoons of the inner bark of slippery elm to 2 cups of boiling water. Cover and simmer for 5 minutes. Strain, add honey as per taste, and drink this tea twice daily when suffering from asthma.
- You can also enjoy some slippery elm lozenges that are readily available in the market to reduce inflammation of the bronchial tubes.
Note: Pregnant or breastfeeding women should not take slippery elm.
6. Licorice
The herb licorice also helps in the treatment of asthma. Licorice has a systemic anti-inflammatory effect on the lungs, which helps reduce inflammation of the bronchial tubes, calm the airways, and restore normal breathing. In addition, it has immune-stimulant properties.
- Add 2 teaspoons of licorice root powder to a cup of hot water. Cover and steep for 10 minutes. Strain, add honey as per taste, and drink it once daily when suffering from asthma.
- You can also take this herb in supplement form.
Note: Licorice is not suitable for people who have diabetes, high blood pressure, adrenal disease, or reduced kidney or liver functioning.
7. Turmeric
Turmeric is a powerful herb to prevent asthma attacks and other allergies. It contains the active ingredient curcumin, a powerful antioxidant and anti-inflammatory compound that helps fight asthma symptoms.
- Mix 1 teaspoon of turmeric powder in 1 cup of milk and boil it. Allow it to cool and drink it twice daily.
- You can also take curcumin supplements after consulting a doctor.
8. Lemongrass
Lemongrass is widely used in traditional medicines for treating asthma, coughs, and other respiratory disorders. It has anti-inflammatory, antibacterial, and antifungal properties that help reduce inflammation and fight infections. In addition, it has vitamin C that boosts your immune system.
- Add 2 teaspoons of dried lemongrass to 2 cups of water ½ teaspoon of grated ginger, 2 cloves, and a small piece of a cinnamon stick.
- Bring it to a boil, then simmer for 5 to 10 minutes.
- Strain, add a little lemon juice and honey, and drink it once daily when suffering from asthma.
9. Stinging Nettle
Stinging nettle is an excellent treatment for allergy-related asthma. This herb contains natural antihistamines and anti-inflammatory properties that help open up constricted bronchial and nasal passages to relieve asthma symptoms. In addition, it is rich in butyric acid, which helps maintain a healthy immune system and metabolism.
- Add 1 tablespoon of dried stinging nettle root or leaves to a cup of hot water. Cover and steep for 5 minutes. Strain, add honey as per taste, and drink it. You can drink this herbal tea a few times per day when suffering from asthma.
- You can also take nettle supplements after consulting your doctor.
Note: This herb may not be suitable for pregnant women and young children.
10. Bishop’s Weed
Bishop’s weed also called carom seeds or ajwain is also useful for treating asthma. It exerts a strong antispasmodic effect on the inflamed bronchioles, which in turn relieves asthma symptoms.
It can even help prevent or ease asthma attacks. Bishop’s weed can also treat bronchitis, emphysema, and whooping cough, as well as cardiovascular disorders. The seeds of this herb are primarily used in asthma treatment.
- Mix together 1 teaspoon each of bishop’s weed seeds and jaggery. Take this mixture twice daily.
- You can also chew some roasted bishop’s weed seeds with water to get relief from asthma symptoms.
Avoiding asthma triggers and tips.
- Try to identify your asthma triggers and avoid them.
- Avoid exposure to cigarette smoke, indoor and outdoor pollution, and other common allergens.
- Include some aerobic exercise, resistance training, and stretching or yoga in your daily routine.
- Do not exercise in cold, dry air, and always warm up before exercising.
- Maintain optimal humidity levels. If needed, use a dehumidifier.
- Clean your home at least once a week. Always wear a mask while cleaning.
- Cover your nose and mouth if you need to go out in the cold.
- Avoid food additives, processed foods, refined carbohydrates, fried foods, and artificial sweeteners.
- Eat foods high in vitamin B12.
- Take omega-3 supplements after consulting a doctor to help decrease inflammation.
- Eat foods high in antioxidants to reduce free radical activity, which tends to stimulate inflammation.
Thank you for reading.
Michael
Comments are welcome
My mother has asthma and I’ve always wondered how exactly it happens. This really is an in depth explanation! I had no idea how much it truly has an effect on the lungs. I do see that there are some natural remedies or treatments to help ease the symptoms of Asthma. I appreciate you sharing this because now I will have some new helpful things I can tell her about to maybe ease her problem. She already is prescribed inhalers but she really likes to experiment with all-natural supplements from time to time to help with different ailments. Anyway, thanks for an interesting read!
Hi Shyla,
Thank you for your comments. Much appreciated. I am glad you found the article helpful. Just remind your mum that there may be certain remedies that may have side effects.
Wishing you and your mum all the best,
Michael