What is a mini-stroke?
Blue indicates link
A mini-stroke is often considered a warning sign of a true stroke in the future if preventive measures are not taken. About 200,000 to 500,000 mini-strokes take place every year in the US. A mini-stroke is also commonly referred to as TIA or little stroke.
A stroke is an attack that occurs within the brain cells. The brain controls a wide range of activities such as talking, eating, and walking, and needs a continuous supply of oxygen through the blood.
Any condition that causes a lack of blood supply to the brain cells can lead to a stroke attack. Several of the day-to-day activities controlled by the brain may be affected in case of a stroke. Mini-stroke symptoms are commonly seen on only one side of the body as the functions of the left and right sides of the body are controlled by one specific side of the brain.
There are many mini-stroke symptoms that must not be ignored when they arise. A mini-stroke can be very dangerous if it is not treated immediately, as it can lead to a full-fledged stroke in some cases.
Knowing how to recognize the various symptoms of a mini-stroke is crucial because it is usually a sign of an impending, full-fledged stroke. A mini-stroke, or even a full stroke, occurs when the blood flow to the brain gets obstructed or halts completely, thus rendering an individual unable to do anything. Severe cases can even lead to an unexpected death, so this is something one should be aware of.
Also, known as a Transient Ischemic Attack (TIA), it needs to be treated within 24 hours of its happening. Failure to do so can lead to some severe consequences. Various neurological processes function simultaneously in the brain and are in fact controlled directly by it. So, if the blood flow to the brain is disrupted, all day-to-day activities become impossible to perform.
What causes a mini-stroke?
A mini-stroke can be caused by a wide variety of factors, although the most common reason leading to stroke is a lack of blood supply to the brain cells. Such a lack of blood supply can occur due to problems associated with the blood vessels of the brain or with that of the heart (the heart pumps blood and any abnormality that affects this action can lead to a lack of blood supply everywhere in the body, including the brain).
The occurrence of a mini-stroke is generally associated with the formation or dislodgement of a clot within the blood vessels of the brain or with the narrowing of the blood vessels of the brain. In some rare instances, a brain stroke or mini-stroke can occur due to conditions that affect the heart, the presence of blood disorders characterized by thickening of the blood, or inflammatory conditions of the blood vessels.
There are many factors that lead to the disruption of the blood flow to the cells located in the brain. Some of these factors are out of our control and can occur unknowingly at any point in time, but some factors can be avoided and even foreseen. The human heart is the organ that pumps blood to various parts of the body, so an inherent problem with the heart is a clear reason for the surfacing of various symptoms.
In most cases though, when the blood vessels of the brain narrow down, a clot is formed in these vessels. This is what prevents the blood from flowing to the brain, and inadvertently leads to a mini-stroke. Here are some commonly found causes that lead to it in women and men of all ages.
- When a blood clot is formed in the arteries of the brain, it is known as thrombosis.
- Atherosclerosis is the narrowing of these blood vessels, and it is similar to the narrowing that occurs in the arteries of the heart before a heart attack.
- An embolus is a blood clot that travels downstream from the heart and gets stuck somewhere along the vessel.
- An embolus is formed as a result of atrial fibrillation, which occurs when the heart does not beat in a coordinated manner.
- Debris and other foreign materials can also get stuck in the arteries at any point in time.
- An intracerebral hemorrhage occurs when a blood vessel bursts, and causes bleeding to reach the brain tissues.
All these causes can be quite dangerous in their own way, and if they are not treated soon, they can cause some serious damage. If a person suffers a mini-stroke, the chances of getting a full-fledged stroke in the next couple of days rise exponentially.
What are the signs and symptoms of mini-stroke?
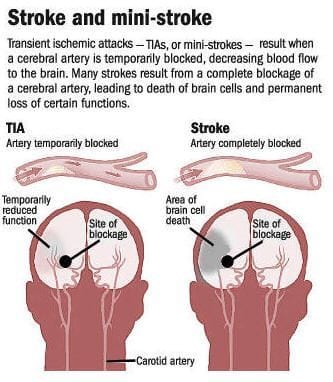
Mini-stroke signs and symptoms can vary with the duration and severity of the attack. They may also vary to some extent in women when compared to men. A wide variety of signs and symptoms may be noted in individuals suffering from a mini-stroke.
In general, mini-stroke symptoms may appear suddenly, last for only a short period (a few minutes to 24 hours), and then disappear completely. These symptoms may recur at a later time.
While a TIA or mini-stroke is different from an actual stroke, the signs and symptoms of a mini-stroke are often identical. However, it should be noted that while the symptoms of an actual stroke tend to last for a long duration, mini-stroke symptoms do not last for more than 24 hours.
Patients who have a diagnosis of TIA are at an increased risk of future ischemic stroke and 15% to 30% of ischemic strokes are preceded by TIA symptoms, often on the same day.
The risk of stroke is highest within the first 24 hours, so prompt and accurate diagnosis is critical, and misdiagnosis can expose patients to unnecessary investigation and long-term secondary prevention treatment, as well as anxiety.
Some of the commonly noted mini-stroke symptoms have been listed below. These symptoms may often be noted on only one side of the body:
- Muscle weakness in the muscles of the face, arm, or leg on one side of the body may be noted. This may or may not be accompanied by numbness or tingling sensations.
- When the speech centers in the brain are affected, one may have trouble speaking or understanding what others are speaking or trying to speak. In some instances, other senses such as eyesight, touch, pain, temperature, pressure, hearing, and taste may be affected.
- Changes in alertness, mood, or emotions may also be noted in some cases. Some tend to suffer from confusion or a transient loss of memory while others may have difficulty writing or reading, clumsiness, trouble walking, and dizziness.
A mini-stroke can be difficult to identify, but a few symptoms may indicate that you’ve had one. The symptoms may be fleeting.
The most common symptoms of a mini-stroke are:
- Dysphasia, a language disorder
- dysarthria, or physical difficulty when speaking
- vision changes
- confusion
- balance issues
- tingling
- an altered level of consciousness
- dizziness
- passing out
- severe headache
- an abnormal sense of taste
- an abnormal sense of smell
- weakness or numbness on just the right or left side of the face or body, determined by the location of the blood clot in the brain
Call your local emergency services or go to the emergency room (ER) if you’re having any of these symptoms.
Dysphasia:
People with a mini-stroke may temporarily find themselves unable to speak. After a mini-stroke, people may tell their doctor that they had difficulty recalling words during the event. Other speech problems may include trouble saying a word or trouble understanding words.
This condition is known as dysphasia. In fact, dysphasia is sometimes the only symptom of a mini-stroke.
Trouble speaking indicates that the blockage or blood clot that caused the mini-stroke occurred in the dominant brain hemisphere.
Temporary blindness in one eye:
Sometimes a mini-stroke manifests as a particular visual disturbance known as amaurosis fugax. Amaurosis fugax is also known as transient monocular blindness (TMB).
In amaurosis fugax, a person’s vision in one eye becomes suddenly dimmed or obscured. The world turns gray or objects look blurry. This may last for seconds or minutes. Exposure to bright light can aggravate amaurosis fugax. You may not be able to read words on white pages.
How long does a mini-stroke last?
The symptoms of a mini-stroke can last as briefly as one minute. By definition, mini-strokes last for fewer than 24 hours.
Often, the symptoms are gone by the time you get to a doctor. Your symptoms may not be present while a doctor evaluates you, so you have to describe the event after your symptoms have disappeared.
Duration aside, symptoms of a mini-stroke are the same as symptoms of an ischemic stroke. An ischemic stroke is the most common type of stroke.
What should you do if someone’s having a stroke?
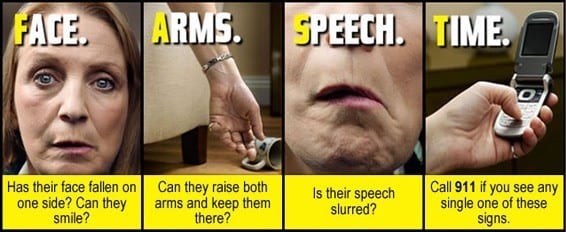
Symptoms that come on suddenly and without warning could signify a stroke. “FAST” is an abbreviation to help you recognize some common stroke symptoms.
F: For Face. If you notice a droop or uneven smile on a person’s face, this is a warning sign.
A: For Arms. Arm numbness or weakness can be a warning sign. You can ask the person to raise their arms if you’re unsure. It’s a warning sign if the arm drops down or isn’t steady.
S: For speech difficulty. Ask the person to repeat something. Slurred speech can indicate that the person is having a stroke.
T: For, time. Act fast if someone is experiencing stroke symptoms. It’s time to call 911 or your local emergency services.
Call 911 or your local emergency services if you or someone around you has any of these symptoms.
What are the risk factors for mini-stroke and stroke?
High blood pressure is a major risk factor. It can damage the inner walls of the arteries, resulting in atherosclerosis. This plaque buildup can rupture and lead to blood clots in these arteries. These abnormalities can lead to a mini-stroke and stroke.
If you’ve received a high blood pressure diagnosis from your doctor, it’s important to keep track of your blood pressure on a routine basis. You should invest in a home blood pressure monitor to check your blood pressure.
Sometimes people have what’s called white coat syndrome. This means that your blood pressure can be higher than usual in your doctor’s office due to anxiety about having your blood pressure checked.
Keeping track of your blood pressure at home can give your doctor a more accurate assessment of your typical blood pressure. This information helps them adjust their blood pressure medications more effectively.
If you have an at-home machine, you should check your blood pressure immediately if you experience any of the following:
- vertigo
- dizziness
- lack of coordination
- gait disturbance
If you don’t have a way to check your blood pressure at home, you should call your doctor immediately or go to a local urgent care center or ER.
Shop for a home blood pressure monitor.
Other risk factors:
Other risk factors for mini-stroke and stroke include:
How is a mini-stroke diagnosed?
A mini-stroke doesn’t lead to permanent brain damage, but you still need an urgent medical examination if you have symptoms of a mini-stroke.
That’s because the symptoms are identical to the symptoms of a stroke. It isn’t possible for you to tell whether they’re related to a mini-stroke or a stroke. The distinction requires a medical evaluation.
Unlike mini-stroke symptoms, stroke symptoms are permanent and do result in permanent damage to brain tissue. However, stroke symptoms may improve with time. Having a mini-stroke puts you at risk of a stroke because mini-strokes and strokes have the same causes.
The only way to tell the difference between a mini-stroke and a stroke is by having a doctor look at an image of your brain with either a CT scan or an MRI scan.
If you’ve had a stroke, it’s likely that it won’t show up on a CT scan of your brain for 24 to 48 hours. An MRI scan usually shows a stroke sooner.
In evaluating the cause of the mini-stroke or stroke, your doctor will likely order an ultrasound to see if there’s significant blockage or plaque in your carotid arteries. You’ll also need an echocardiogram to look for blood clots in your heart.
Your doctor may also take an electrocardiogram (ECG or EKG) and chest X-ray.
How are mini-strokes treated?
Several treatment options are available. Mini strokes don’t cause lasting brain tissue damage or disabilities, but they can be an early warning sign of a stroke. Treatment for mini-strokes focuses on starting or adjusting medications that improve blood flow to the brain.
It also requires identifying abnormalities that your doctor can fix to reduce your risk of future mini-strokes or strokes.
Treatment options include drugs, medical procedures, and lifestyle changes.
Antiplatelet drugs:
Antiplatelet drugs make your platelets less likely to stick together to prevent blood clots. These medications include:
- aspirin
- clopidogrel (Plavix)
- prasugrel (Effient)
- aspirin-dipyridamole (Aggrenox)
Anticoagulants:
These medications prevent blood clots by targeting proteins that cause clotting, rather than targeting the platelets. This category includes:
- Warfarin (Coumadin)
- rivaroxaban (Xarelto)
- apixaban (Eliquis)
If you’re taking warfarin, you’ll need close monitoring with blood tests to make sure you have the correct dosage. Drugs such as rivaroxaban and apixaban don’t require monitoring.
Minimally invasive carotid intervention:
This is a surgical procedure that involves accessing the carotid arteries with a catheter.
The catheter is inserted through the femoral artery in your groin. The doctor uses a balloon-like device to open up clogged arteries. They’ll place a stent or small wire tube inside the artery at the point of narrowing to improve blood flow to the brain.
Surgery:
You may need surgery to prevent future strokes. If you have a severe narrowing of the carotid artery in your neck and aren’t a candidate for carotid angioplasty and stenting, your doctor may recommend a surgery called a carotid endarterectomy.
In the procedure, your doctor clears the carotid arteries of fatty deposits and plaques. This can reduce the risk of another mini-stroke or a stroke.
Lifestyle changes:
Lifestyle changes may be necessary to reduce your risk of future mini-strokes or strokes. Medications and other medical interventions may not be enough.
These lifestyle changes include:
- exercising
- losing weight
- eating more fruits and vegetables
- reducing your intake of fried or sugary foods
- getting enough sleep
- reducing stress
- improving your control of other medical conditions, including diabetes, high blood pressure, and high cholesterol
How can you prevent a mini-stroke?
Ministrokes and other types of strokes are sometimes unavoidable, but you can take precautions to help prevent mini-strokes.
Follow these mini-stroke and stroke prevention tips:
- Don’t smoke.
- Avoid secondhand smoke.
- Eat a balanced diet with more fruits and vegetables.
- Maintain a healthy weight.
- Exercise regularly.
- Limit your alcohol intake.
- Don’t use illicit drugs.
- Control your diabetes.
- Limit your cholesterol and fat intake, especially saturated and trans fats.
- Make sure your blood pressure is under good control.
- Reduce stress.
Related stories
More on Preventing Stroke:
Each year, twice as many women die from stroke as they do breast cancer. That’s why it’s important to remain vigilant about your health. To help prevent a future stroke, you can:
- eat a balanced diet
- maintain a healthy weight
- get regular exercise
- quit smoking
- Take up a hobby, such as knitting or yoga, to help better manage stress
Women should also take added precautions because of the unique risk factors they face. This means:
- monitoring blood pressure during and after pregnancy
- screening for atrial fibrillation (AFib) if over 75 years old
- Screening for high blood pressure before starting birth control
Outlook:
Stroke recovery can vary from person to person. Physical therapy may be able to help you relearn any lost skills. Some people may be able to relearn how to walk or talk within a matter of months. Others may need more time to recover.
During this time, it’s important to stay on track with rehabilitation and maintain or develop a healthy lifestyle. In addition to aiding your recovery, this may help prevent future strokes.
TIA or Mini-Stroke:
Although a mini-stroke will clear up on its own, it should be taken as a serious warning sign of what’s to come. Ignoring a mini-stroke can mean the difference between life and death. A mini-stroke can last for a few moments or last all day, but in either case, seek emergency medical attention.
Why are the symptoms of mini-stroke different in women?
While some mini-stroke symptoms are common in both men and women, a few symptoms and signs are specifically noted in women. Studies have reported that when compared to men, women are 43% more likely to report many of the nontraditional symptoms of a stroke. These studies reported that symptoms such as pain, change in mental status, a feeling of lightheadedness, headache, or other associated symptoms were common in women experiencing a mini-stroke.
Women experiencing a mini-stroke can experience abrupt pain in the face and arm or the leg (generally on one side of the body). In some instances, they have sudden hiccups that do not subside after drinking water. A few feel nauseated, while others abruptly start feeling tired. A mini-stroke is also known to cause sudden chest pain or pounding or racing heartbeats. Sudden shortness of breath has also been reported in a few cases.
The Women’s Health Study examined aspirin as a primary prevention agent for cardiovascular disease in healthy women over age 45 years and the risk of ischemic stroke was reduced by 24%. However, no benefit was found for cardiac risk.
Symptoms of a Mini Stroke in Women
Though most of the symptoms are the same for men and women, there are some that are unique to women. According to studies, women are 43% more likely to display some unique symptoms
- The individual feels a restriction on the ability to speak and move as normal.
- Vision is also affected suddenly.
- There is general confusion, and an inability to follow instructions as well.
- Dizziness, loss of balance, and loss of coordinated movement will also be noted.
- The person may fall suddenly without actually losing consciousness.
Apart from these common symptoms, here are some others that are observed only in women.
- Pain
- Change in mental state
- Headache
- Lightheadedness
- Sudden pain on one side of the body
- Sudden hiccups
- Nausea and fatigue
- Shortness of breath
- Chest pain
- Increased heartbeat
These symptoms can often be confused for a multitude of other diseases and conditions, so it is imperative to pay attention to them and act accordingly. Failure to do so can inevitably lead to a full stroke, and the damage can be permanent in some cases.
Recognizing all the symptoms in women, and even in men for that matter, is something that can be achieved after doing some extensive reading on the subject. Being prepared for such emergencies is vitally important, as is immediate action.
Your Road To Recovery. Helpful Remedies to Consider:
Black or green tea:
Tea contains plant nutrients called flavonoids, which can help decrease cholesterol and blood pressure. Drinking at least 3 cups of black or green tea per day may help reduce your risk of stroke. Researchers in one study found that people who drank this amount of green or black tea had far fewer incidences of repeated stroke.
Black tea may be especially helpful for diabetes management. The compounds in black tea mimic the effects of insulin and prevent starch from turning into sugar.
Fruits and vegetables:
Fruits and vegetables aren’t just good for your physical health. Researchers in a 2016 study found that eating more fruit may increase happiness and well-being as quickly as the next day. Eating eight portions per day may increase life satisfaction and help lower stress levels.
Pomegranate:
Pomegranate concentrate is high in antioxidants and phytosterols, which are plant steroids that lower cholesterol. Taking pomegranate concentrate on low-dose statin therapy or the regular use of cholesterol-lowering drugs can help reduce cholesterol, according to the Israeli Institute of Technology. It may also lessen statin’s side effects, such as muscle pain.
Yoga is a good option for low-impact exercise.
According to the Harvard Health Blog, research findings suggest that yoga may improve stroke recovery, especially for people with balance issues or fear of falling. Yoga promotes smooth physical movements, improved breathing, and mental focus that may have been lost after a stroke.
Another popular exercise for stroke prevention and recovery is tai chi. Tai chi is a Chinese exercise consisting of slow and graceful movements practiced in a semi-squatting position.
Research from 2015 showed that tai chi helps improve body balance and reduces depression and anxiety. In 2017, many of those same researchers published a study suggesting that tai chi has a role as a protective measure against ischemic stroke in older adults.
Maintaining a healthy weight, and a healthy body fat ratio or body mass index (BMI), is a good way to manage many risk factors for stroke.
If most of a person’s body fat rests around the waist instead of the hips, then they have a greater risk of heart disease and type 2 diabetes. Women with a waist size greater than 35 inches and men with a waist size greater than 40 inches also have a higher risk of these conditions, according to the National Heart, Lung, and Blood Institute (NHLBI).
The NHLBI states that weight loss can:
- improve blood pressure readings
- lower cholesterol
- lower risk of type 2 diabetes
- decrease body fat
Visit your doctor to find out your ideal healthy weight.
High levels of stress are linked to a significantly increased risk of stroke, according to the American Heart Association (AHA). Learn relaxation techniques to reduce tension in your mind and body.
Massages:
Massages can help increase blood flow to an affected area, especially for stroke-related muscle problems. In one study, massages decreased pain, increased health, and improved movement after stroke.
A few studies in China also found that external counterpulsation (ECP) treatments might encourage recovery in people who’ve had an ischemic stroke.
ECP treatments involve wrapping cuffs around the hips, thighs, and calves. These cuffs inflate and deflate, creating a massage-like sensation and helping blood flow to the brain.
Researchers at the S.H. Ho Cardiovascular Disease and Stroke Centre in Hong Kong found that one-hour ECP treatments for 35 days increased blood pressure by 13 percent, heart function by 74 percent, and blood flow to the brain by 9 percent.
Other techniques:
Other ways you can relax include:
- aromatherapy
- fun hobbies, such as reading or playing board games
- positive self-talk
- meditation
- getting enough rest
Acupuncture involves a practitioner inserting small needles into specific points of the body. It’s known to help ease pain and manage other muscle problems affected by stroke. A similar therapy is acupressure, which uses pressure instead of needles on the same points as acupuncture.
There isn’t enough scientific evidence on acupuncture’s effectiveness for stroke prevention. However, some research has revealed overall improvements in people’s quality of life, including positive effects on mobility.
Acupuncture is considered safe when an experienced and licensed practitioner applies it.
Check your acupuncturist’s certifications if you’re interested in this therapy. A licensed acupuncturist will have a Master of Acupuncture, Master of Acupuncture and Oriental Medicine, or Doctor of Oriental Medicine certification. Look for the title licensed acupuncturist (LAc) too. Licensed acupuncturists have the training and skills to use acupuncture for health issues, such as:
- certain chronic diseases
- pain
- rehabilitation
- injured muscles
Boost prevention or recovery:
It’s suggested certain vitamins or supplements may help with risk factors such as high cholesterol and blood vessel damage. However, rigorous studies are still needed to support such claims.
Some supplements may cause negative side effects when used with certain medications. Check with your doctor before taking any extra nutritional or herbal supplements.
Vitamins and nutrients
Little scientific evidence exists that indicates supplements can prevent stroke directly. However, some research suggests that they can help reduce risk and improve recovery. You may find benefits from taking the following:
- Folic acid, vitamin B-6, and vitamin B-12. Certain B vitamins could help to lower levels of the amino acid homocysteine. High levels of homocysteine are linked with an increased risk of stroke.
- Betaine. Research shows that the amino acid betaine may lower levels of homocysteine.
- Vitamin C. This vitamin may aid in repairing blood vessel damage and reducing plaque buildup in the arteries.
- Vitamin D. Supplements of this vitamin may be beneficial because low vitamin D levels are associated with an increased risk of artery-blocking strokes, especially in people with high blood pressure.
- Vitamin E. Taking supplements of vitamin E may help with memory impairment.
- Omega-3 fatty acids. In general, omega-3 fatty acids may improve cholesterol levels. One type of omega-3 fatty acid, alpha-lipoic acid (ALA), may also prevent cell damage, according to a study performed on rats.
- Magnesium. The mineral magnesium may lower blood pressure, according to a study in the journal Hypertension.
Herbal supplements:
Herbal supplements are a popular choice for people who prefer natural remedies. The following herbal supplements may improve blood circulation in the brain and help prevent another stroke:
- Ashwagandha. Also known as Indian ginseng, ashwagandha has antioxidant properties that may prevent and treat stroke. A 2015 study explored its effect on mice.
- Bilberry. This berry may improve cholesterol and lower blood sugar.
- Garlic. Preventing blood clotting and destroying plaque are two potential benefits of garlic.
- Asian ginseng. A staple of Chinese medicine, Asian ginseng is said to improve memory.
- Gotu kola. This herb has been shown to boost cognitive function in people who’ve had strokes.
- Turmeric. A spice, turmeric may lower cholesterol levels and help prevent blockages in arteries.
- For online links to the herbal supplements please click on the products.
You’ll want to avoid these supplements if you’re taking warfarin (Coumadin), aspirin, or any other blood-thinning medications. They’ll thin your blood even more. Always ask your doctor first before taking any additional supplements.
More Related Information:
Always consult with a doctor if you feel any symptoms or notice any differences in you. F.A.S.T.
Thank you for reading.
Michael
Comments are welcome






Thank you for your information filled article about mini-strokes. I know that I need to read through an article such as yours at least one time a year to remind me of the symptoms, the ones beyond the FAST warning we are familiar with. Mimi strokes are serious business and often a bit difficult to correctly diagnose. This is another reason to refresh and remind yourself of the symptoms, to better prepare yourself to help your Dr. should this happen to you.
The writer of this article has provided symptom descriptions, and how to describe them to your Dr We are also provided the descriptions of the treatments as well as some preventive treatment we can do ourselves. There is also a list of suggested food supplements and diet changes to help prevent strokes.
As a mature female I appreciate having this information to review should I find myself questioning what a mini-stroke is. This article is well worth the read for anyone who is interested in keeping themselves healthy. Thanks, Sami
Hi Sami,
Thank you for your comments. Being aware can save lives. FAST is a great way to diagnose a mini-stroke/stroke, and proceed with immediate action such as calling 911 and seeking immediate medical attention.
Best wishes,
Michael
This article is so important and educative. I never knew that altering you lifestyle such as; exercising and changing a few bad habits has a way of reducing the risk of having a mini stroke.
I already saved this post so I could go over it again as well as share to friends. Thanks for sharing this with me.
Hi Awinikistevie,
Thank you for your comments. Exercise, diet, and weight control are all important factors to avoid mini-strokes and strokes. I appreciate you sharing this post. It could save a life, and prevent permanent disabilities.
Best wishes,
Michael
very informative article on the diagnosis and symptoms of stroke and mini stroke. You have provided a comprehensive stroke education for anyone to read and to become familiar with the signs and ways to prevent this from happening. I especially like the FAST method of quickly diagnosing a possible stroke or TIA.
Hi Dave M.
Thank you for your comments. I did not know about the “F.A.S.T method of diagnosing a mini-stroke/stroke until I started to research mini-strokes. It is so important to get help if you notice any one of these signs as soon as possible.
Best wishes,
Michael
So much information on mini stroke symptoms in women. When I see any victim of strokes it really baffles me what the causes may be. I have basically learnt a whole lot of things about mini stroke symptoms. I never even knew that high cholesterol, diabetes, smoking, obesity and atrial fibrillation are risk factors for Mini stroke. Thanks this piece is really helpful.
Hi Sheddy Ovb,
Thank you for your comments. It is important to maintain a healthy weight, do exercises on a regular basis, and eat healthily. Please if you see anyone with symptoms of a mini-stroke call 911. Immediate help is a life changer.
Best wishes,
Michael
Hello there, thanks so much for the post.
From your post I realized how important exercises are. I don’t really do much of exercises, I believe the stress is just enough to do the work of the exercises! But the truth is one can avoid many sicknesses and diseases through excercises.
Thanks for enlightening us on the ” warning signs of mini stroke”. It is appreciated.
Hi Lizzychris,
Thank you for your comments. Just as important as exercise is a healthy diet. We can save lives, and change some of the disabilities a mini-stroke can cause. We just got to recognize the symptoms in time.
Best wishes,
Michael
amazing article on putting these tips on how to treat mini strokes and also symptoms to look out for in other to treat mini strokes at an early stage…it’s very important that we take measures to avoid every bit of pain that could be prevented from coming our ways.
Thansk for these Great tips given here…I look forward to seeing more of your post
Hi evans,
Thank you for your comments. Someone I loved very much showed the symptoms of a mini-stroke. She had a beautiful smile, and when I looked over some photographs I noticed her smile was only partial. If I only knew she may not have fallen victim to a heart attack.
All the best,
Michael
Hey nice article you have there. A ministroke is also known as a transient ischemic attack .It occurs when part of the brain experiences a temporary lack of blood flow. This causes stroke-like symptoms that resolve within 24 hours. Unlike a stroke,a ministroke on its own doesn’t cause permanent disabilities. Thanks do hope it helps.
Hi edahnewton1,
Thank you for your comments. You are absolutely right. A mini-stroke is also known as TIA. If it is caught in time it will not cause permanent disabilities. It is almost like a traffic light turning orange. It could change to red or green treating and acknowledging the symptoms are key to the outcome.
Best wishes,
Michael