Pandemic vs Epidemic
The WHO declares the outbreak of the new coronavirus is a pandemic.
WHO: World Health Organization
This is the first pandemic since H1N1
On March 11th, 2020, the World Health Organization officially changed its designation of COVID-19, the illness caused by a coronavirus, from an epidemic to a pandemic. This shift prompted a considerable number of people to turn to the dictionary, in order to ascertain the difference between the two endemics. What is the difference between an epidemic and a pandemic?
Epidemic vs. Pandemic:
An epidemic is defined as “an outbreak of disease that spreads quickly and affects many individuals at the same time.” A pandemic is a type of epidemic (one with greater range and coverage), an outbreak of a disease that occurs over a wide geographic area and affects an exceptionally high proportion of the population. While a pandemic may be characterized as a type of epidemic, you would not say that an epidemic is a type of pandemic.
A pandemic is a disease epidemic that has spread across a large region, for instance, multiple continents, or worldwide. A widespread endemic disease with a stable number of infected people is not a pandemic. Further, flu pandemics generally exclude recurrences of seasonal flu. Throughout history, there have been a number of pandemics of diseases such as smallpox and tuberculosis.
One of the most devastating pandemics was the Black Death, which killed an estimated 75–200 million people in the 14th century. Current pandemics include HIV/AIDS and the 2019 coronavirus disease. Other notable pandemics include the 1918 influenza pandemic (Spanish flu) and the 2009 flu pandemic (H1N1).
HIV originated in Africa and spread to the United States via Haiti between 1966 and 1972. AIDS is currently a pandemic, with infection rates as high as 25% in southern and eastern Africa. In 2006, the HIV prevalence rate among pregnant women in South Africa was 29%. Effective education about safer sexual practices and bloodborne infection precautions training have helped to slow down infection rates in several African countries sponsoring national education programs.
Coronavirus disease 2019 (COVID-19)
2019–20 Coronavirus Declared Pandemic
People queuing outside a Wuhan pharmacy to buy face masks and medical supplies
A new coronavirus was first identified in Wuhan, Hubei, China, in late December 2019, as causing a cluster of cases of acute respiratory disease, now referred to as coronavirus disease 2019 (COVID-19), which had been identified in December 2019. According to the media report, more than 116 countries and territories have been affected, with major outbreaks in central China, Italy, South Korea, and Iran. On March 11, 2020, the World Health Organization characterized the spread of COVID-19 as a pandemic.
Cholera
Cholera outbreaks and pandemics
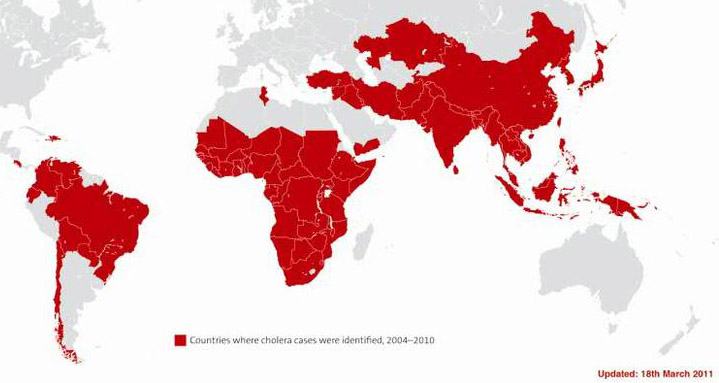
Since it became widespread in the 19th century, cholera has killed tens of millions of people.
1817–1824 cholera pandemic. Previously restricted to the Indian subcontinent, the pandemic began in Bengal, then spread across India by 1820. 10,000 British troops and countless Indians died during this pandemic. It extended as far as China, Indonesia (where more than 100,000 people succumbed to the island of Java alone) and the Caspian Sea before receding. Deaths in the Indian subcontinent between 1817 and 1860 are estimated to have exceeded 15 million persons. Another 23 million died between 1865 and 1917. Russian deaths during a similar period exceeded 2 million.
1826–1837 cholera pandemic. Reached Russia (see Cholera Riots), Hungary (about 100,000 deaths) and Germany in 1831, London in 1832 (more than 55,000 persons died in the United Kingdom), France, Canada (Ontario), and the United States (New York City) in the same year, and the Pacific coast of North America by 1834. It is believed that over 150,000 Americans died of cholera between 1832 and 1849.
1846–1860 cholera pandemic. Deeply affected Russia, with over a million deaths. A two-year outbreak began in England and Wales in 1848 and claimed 52,000 lives. Throughout Spain, cholera caused more than 236,000 deaths in 1854–55. It claimed 200,000 lives in Mexico.
1863–75 cholera pandemic. Spread mostly in Europe and Africa. At least 30,000 of the 90,000 Mecca pilgrims fell victim to the disease. Cholera claimed 90,000 lives in Russia in 1866.
In 1866, there was an outbreak in North America. It killed some 50,000 Americans.
1881–96 cholera pandemic. The 1883–1887 epidemic cost 250,000 lives in Europe and at least 50,000 in the Americas. Cholera claimed 267,890 lives in Russia (1892); 120,000 in Spain; 90,000 in Japan and 60,000 in Persia.
In 1892, cholera contaminated the water supply of Hamburg and caused 8,606 deaths.
1899–1923 cholera pandemic. It had little effect in Europe because of advances in public health, but Russia was badly affected again (more than 500,000 people dying of cholera during the first quarter of the 20th century). The sixth pandemic killed more than 800,000 in India. The 1902–1904 cholera epidemic claimed over 200,000 lives in the Philippines.
1961–75 cholera pandemic. Began in Indonesia, called El Tor after the new biotype responsible for the pandemic, and reached Bangladesh in 1963, India in 1964, and the Soviet Union in 1966. Since then the pandemic has reached Africa, South America, and Central America.
Influenza
Influenza pandemic
So far, the new coronavirus has led to more than 220,000 illnesses and more than 9,300 deaths worldwide. But that’s nothing compared with the flu, also called influenza. In the U.S. alone, the flu has caused an estimated 36 million illnesses, 370,000 hospitalizations, and 22,000 deaths this season, according to the Centers for Disease Control and Prevention (CDC). That is in the United States alone.
Advice (in French and English) for travelers on risks of epidemics abroad. Posters from the Charles De Gaulle airport, Paris.
The Greek physician Hippocrates, the “Father of Medicine”, first described influenza in 412 BC.
The first influenza pandemic was recorded in 1580, and since then, influenza pandemics occurred every 10 to 30 years.
The 1889–1890 flu pandemic, also known as Russian Flu, was first reported in May 1889 in Bukhara, Uzbekistan. By October, it had reached Tomsk and the Caucasus. It rapidly spread west and hit North America in December 1889, South America in February–April 1890, India in February–March 1890, and Australia in March–April 1890. The H3N8 and H2N2 subtypes of the Influenza A virus have each been identified as possible causes. It had a very high attack and mortality rate, causing around a million fatalities.
The “Spanish flu”, 1918–1919. First identified early in March 1918 in US troops training at Camp Funston, Kansas. By October 1918, it had spread to become a worldwide pandemic on all continents, and eventually infected about one-third of the world’s population (or ≈500 million persons). Unusually deadly and virulent, it ended nearly as quickly as it began, vanishing completely within 18 months.
In six months, some 50 million were dead; some estimates put the total of those killed worldwide at over twice that number. About 17 million died in India, 675,000 in the United States, and 200,000 in the UK. The virus that caused Spanish flu was also implicated as a cause of encephalitis lethargica in children. The virus was recently reconstructed by scientists at the CDC studying remains preserved by the Alaskan permafrost. The H1N1 virus has a small, but the crucial structure that is similar to the Spanish flu.
The “Asian Flu”, 1957–58. An H2N2 virus first identified in China in late February 1957, It caused about 2 million deaths globally. The Asian flu spread to the United States by June 1957 and caused about 70,000 deaths in the US.
The “Hong Kong Flu”, 1968–69. An H3N2 virus first detected in Hong Kong in early 1968 and spread to the United States later that year. This pandemic of 1968 and 1969 killed approximately one million people worldwide. It caused about 34,000 deaths in the United States.
The “Swine Flu”, 2009–10. An H1N1 virus first detected in Mexico in early 2009 and spread to the United States later that year. This pandemic killed around half a million people worldwide. It caused about 12,000 deaths in the United States.
H5N1 (Avian Flu)
Influenza A virus subtype H5N1
In February 2004, the avian influenza virus was detected in birds in Vietnam, increasing fears of the emergence of new variant strains. It is feared that if the avian influenza virus combines with a human influenza virus (in a bird or a human), the new subtype created could be both highly contagious and highly lethal in humans. Such a subtype could cause a global influenza pandemic, similar to the Spanish flu, or the lower mortality pandemics such as the Asian Flu and the Hong Kong Flu.
From October 2004 to February 2005, some 3,700 test kits of the 1957 Asian Flu virus were accidentally spread around the world from a lab in the US.
In May 2005, scientists urgently called upon nations to prepare for a global influenza pandemic that could strike as much as 20% of the world’s population.
In October 2005, cases of the avian flu (the deadly strain H5N1) were identified in Turkey. EU Health Commissioner Markos Kyprianou said: “We have received now confirmation that the virus found in Turkey is an avian flu H5N1 virus. There is a direct relationship with viruses found in Russia, Mongolia, and China.” Cases of bird flu were also identified shortly thereafter in Romania, and then Greece. Possible causes of the virus have also been found in Croatia, Bulgaria, and the United Kingdom.
By November 2007, numerous confirmed cases of the H5N1 strain had been identified across Europe. However, by the end of October, only 59 people had died as a result of H5N1, which was atypical of previous influenza pandemics.
Avian flu cannot yet be categorized as a “pandemic”, because the virus cannot yet cause sustained and efficient human-to-human transmission. Cases so far are recognized to have been transmitted from bird to human, but as of December 2006, there have been very few (if any) cases of proven human-to-human transmission. Regular influenza viruses establish infection by attaching to receptors in the throat and lungs, but the avian influenza virus can only attach to receptors located deep in the lungs of humans, requiring close, prolonged contact with infected patients, and thus limiting person-to-person transmission.
Influenza A (H3N2) viruses still circulate today.
Typhus:
Typhus is sometimes called “camp fever” because of its pattern of flaring up in times of strife. (It is also known as “gaol fever” and “ship fever”, for its habits of spreading wildly in cramped quarters, such as jails and ships.) Emerging during the Crusades, it had its first impact in Europe in 1489, in Spain. During fighting between the Christian Spaniards and the Muslims in Granada, the Spanish lost 3,000 to war casualties, and 20,000 to typhus. In 1528, the French lost 18,000 troops in Italy and lost supremacy in Italy to the Spanish. In 1542, 30,000 soldiers died of typhus while fighting the Ottomans in the Balkans.
During the Thirty Years’ War (1618–1648), about 8 million Germans were killed by bubonic plague and typhus. The disease also played a major role in the destruction of Napoleon’s Grande Armée in Russia in 1812. During the retreat from Moscow, more French military personnel died of typhus than were killed by the Russians. Of the 450,000 soldiers who crossed the Neman on 25 June 1812, fewer than 40,000 returned. More military personnel were killed from 1500–1914 by typhus than from military action.
In early 1813, Napoleon raised a new army of 500,000 to replace his Russian losses. In the campaign of that year, over 219,000 of Napoleon’s soldiers died of typhus. Typhus played a major factor in the Irish Potato Famine. During World War I, typhus epidemics killed over 150,000 in Serbia. There were about 25 million infections and 3 million deaths from epidemic typhus in Russia from 1918 to 1922. Typhus also killed numerous prisoners in the Nazi concentration camps and Soviet prisoner of war camps during World War II. More than 3.5 million Soviet POWs died out of the 5.7 million in Nazi custody.
Smallpox:
Smallpox was a contagious disease caused by the variola virus. The disease killed an estimated 400,000 Europeans per year during the closing years of the 18th century. During the 20th century, it is estimated that smallpox was responsible for 300–500 million deaths. As recently as the early 1950s, an estimated 50 million cases of smallpox occurred in the world each year.
After successful vaccination campaigns throughout the 19th and 20th centuries, the WHO certified the eradication of smallpox in December 1979. To this day, smallpox is the only human infectious disease to have been completely eradicated, and one of two infectious viruses ever to be eradicated along with rinderpest.
Measles:
Historically, measles was prevalent throughout the world, as it is highly contagious. According to the U.S. National Immunization Program, 90% of people were infected with measles by age 15. Before the vaccine was introduced in 1963, there were an estimated 3–4 million cases in the U.S. each year. Measles killed around 200 million people worldwide over the last 150 years. In 2000 alone, measles killed some 777,000 worldwide out of 40 million cases globally.
Measles is an endemic disease, meaning that it has been continually present in a community, and many people develop resistance. In populations that have not been exposed to measles, exposure to a new disease can be devastating. In 1529, a measles outbreak in Cuba killed two-thirds of the natives who had previously survived smallpox. The disease had ravaged Mexico, Central America, and the Inca civilization.
Tuberculosis:
TB is one of the top ten leading causes of death worldwide and the leading cause of a single infectious agent, ranking above HIV/AIDS. In 2018 the TB statistics show that there were a total of 1,491,000 TB-related deaths, 1.24 million among HIV negative people, and an additional 251,000 among HIV positive people.
Statics According to The World Health Organization 2019
10,000,000 Fell ill with TB 2018
1,500,000 Died as a result of TB 2018
The WHO says fatality rates have previously varied between 25 percent and 95 percent in previous outbreaks.
In 2007, the prevalence of TB per 100,000 people was highest in Sub-Saharan Africa and was also relatively high in Asian countries like India.
One-quarter of the world’s current population has been infected with Mycobacterium tuberculosis, and new infections occur at a rate of one per second. About 5–10% of these latent infections will eventually progress to active disease, which, if left untreated, kills more than half of its victims. Annually, 8 million people become ill with tuberculosis, and 2 million people die from the disease worldwide.
In the 19th century, tuberculosis killed an estimated one-quarter of the adult population of Europe; by 1918, one in six deaths in France were still caused by tuberculosis. During the 20th century, tuberculosis killed approximately 100 million people. TB is still one of the most important health problems in the developing world.
Leprosy:
Leprosy, also known as Hansen’s disease, is caused by a bacillus, Mycobacterium leprae. It is a chronic disease with an incubation period of up to five years. Since 1985, 15 million people worldwide have been cured of leprosy.
Historically, leprosy has affected people since at least 600 BC. Leprosy outbreaks began to occur in Western Europe around 1000 AD. Numerous leprosaria, or leper hospitals, sprang up in the Middle Ages; Matthew Paris estimated that in the early 13th century, there were 19,000 of them across Europe.
Malaria:
Past and current malaria prevalence in 2009
Malaria is widespread in tropical and subtropical regions, including parts of the Americas, Asia, and Africa. Each year, there are approximately 350–500 million cases of malaria. Drug resistance poses a growing problem in the treatment of malaria in the 21st century, since resistance is now common against all classes of antimalarial drugs, except for the artemisinins.
Malaria was once common in most of Europe and North America, where it is now for all purposes non-existent. Malaria may have contributed to the decline of the Roman Empire. The disease became known as “Roman fever”. Plasmodium falciparum became a real threat to colonists and indigenous people alike when it was introduced into the Americas along with the slave trade.
Malaria devastated the Jamestown colony and regularly ravaged the South and Midwest of the United States. By 1830, it had reached the Pacific Northwest. During the American Civil War, there were over 1.2 million cases of malaria among soldiers of both sides. The southern U.S. continued to be afflicted with millions of cases of malaria into the 1930s.
Yellow fever:
Yellow fever has been a source of several devastating epidemics. Cities as far north as New York, Philadelphia, and Boston were hit with epidemics. In 1793, one of the largest yellow fever epidemics in U.S. history killed as many as 5,000 people in Philadelphia—roughly 10% of the population. About half of the residents had fled the city, including President George Washington. In colonial times, West Africa became known as “the white man’s grave” because of malaria and yellow fever.
Ebola outbreak 2019:
Ebola has claimed the lives of more than 1,600 people in the last year since a new outbreak spread in the Democratic Republic of Congo (DRC). The World Health Organization (WHO) issued an international emergency declaration this week after the first case of Ebola spread to the first major urban population in Goma last Sunday. The city is home to more than a million people and sits near to an international airport. Health officials hope by announcing the emergency declaration that more funds will become available to fight the latest outbreak.
Latest numbers as of 16 March 2020
Total of 3444 cases (3310 confirmed & 134 probable), including 2264 deaths, 1169 survivors, and patients still under care.
Ebola was transmitted to humans by wild animals but can be passed from person to person.
Figure 1: Confirmed and probable Ebola virus disease cases by week of illness onset, data as of 5 February 2019 (n=789)1
The WHO says the virus can be spread “via direct contact through broken skin or mucous membranes”.
A person who has come into with a person with Ebola or has touched a contaminated object that has body fluids from the sick person can be infected.
Zika virus:
2015–16 Zika virus epidemic, Zika virus, and Zika fever.
An outbreak of the Zika virus began in 2015 and strongly intensified throughout the start of 2016, with over 1.5 million cases across more than a dozen countries in the Americas. The World Health Organization warned that Zika had the potential to become an explosive global pandemic if the outbreak was not controlled.
Antibiotic resistance:
Antibiotic-resistant microorganisms sometimes referred to as “superbugs”, may contribute to the re-emergence of diseases that are currently well controlled. For example, cases of tuberculosis that are resistant to traditionally effective treatments remain a cause of great concern to health professionals. Every year, nearly half a million new cases of multidrug-resistant tuberculosis (MDR-TB) are estimated to occur worldwide. China and India have the highest rate of multidrug-resistant TB.
The World Health Organization (WHO) reports that approximately 50 million people worldwide are infected with MDR TB, with 79 percent of those cases resistant to three or more antibiotics. In 2005, 124 cases of MDR TB were reported in the United States. Extensively drug-resistant tuberculosis (XDR TB) was identified in Africa in 2006 and subsequently discovered to exist in 49 countries, including the United States. There are about 40,000 new cases of XDR-TB per year, the WHO estimates.
In the past 20 years, common bacteria including Staphylococcus aureus, Serratia marcescens, and Enterococcus, have developed resistance to various antibiotics such as vancomycin, as well as whole classes of antibiotics, such as the aminoglycosides and cephalosporins. Antibiotic-resistant organisms have become an important cause of healthcare-associated (nosocomial) infections (HAI). In addition, infections caused by community-acquired strains of methicillin-resistant Staphylococcus aureus (MRSA) in otherwise healthy individuals have become more frequent in recent years.
Viral hemorrhagic fevers:
Viral hemorrhagic fevers such as Ebola virus disease, Lassa fever, Rift Valley fever, Marburg virus disease, and Bolivian hemorrhagic fever are highly contagious and deadly diseases, with the theoretical potential to become pandemics. Their ability to spread efficiently enough to cause a pandemic is limited, however, as the transmission of these viruses requires close contact with the infected vector and the vector only has a short time before death or serious illness.
Furthermore, the short time between a vector becoming infectious and the onset of symptoms allows medical professionals to quickly quarantine vectors, and prevent them from carrying the pathogen elsewhere. Genetic mutations could occur, which could elevate their potential for causing widespread harm; thus close observation by contagious disease specialists is merited.
Coronaviruses:
Coronaviruses (CoV) are a large family of viruses that cause illness ranging from the common cold to more severe diseases such as Middle East Respiratory Syndrome (MERS-CoV) and Severe Acute Respiratory Syndrome (SARS-CoV). A new strain of coronavirus (SARS-CoV-2) causes Coronavirus disease in 2019.
Some coronaviruses are zoonotic, meaning they are transmitted between animals and people. Detailed investigations found that SARS-CoV was transmitted from civet cats to humans and MERS-CoV from dromedary camels to humans. Several known coronaviruses are circulating in animals that have not yet infected humans. Common signs of infection include respiratory symptoms, fever, cough, shortness of breath, and breathing difficulties.
In more severe cases, an infection can cause pneumonia, severe acute respiratory syndrome, kidney failure, and even death. Standard recommendations to prevent infection spread include regular hand washing, covering mouth and nose when coughing and sneezing, thoroughly cooking meat and eggs and avoiding close contact with anyone showing symptoms of respiratory illness such as coughing and sneezing.
Severe acute respiratory syndrome. (SARS):
In 2003 the Italian physician Carlo Urbani (1956–2003) was the first to identify severe acute respiratory syndrome (SARS) as a new and dangerously contagious disease, although he became infected and died. It is caused by a coronavirus dubbed SARS-CoV. Rapid action by national and international health authorities such as the World Health Organization helped to slow transmission and eventually broke the chain of transmission, which ended the localized epidemics before they could become a pandemic. However, the disease has not been eradicated and could re-emerge. This warrants monitoring and reporting of suspicious cases of atypical pneumonia.
Economic consequences:
In 2016, the Commission on a Global Health Risk Framework for the Future estimated that pandemic disease events would cost the global economy over $6 trillion in the 21st century—over $60 billion per year. The same report also recommended spending $4.5 billion annually on global prevention and response capabilities to reduce the threat posed by pandemic events.
As of March 16, 2020, the outbreak of the coronavirus disease (COVID-19) had been confirmed in over 100 countries or territories. The virus had infected 167,511 people worldwide, and the number of deaths had totaled 6,606. The most severely affected countries outside of China include Italy, Iran, Spain, and South Korea.
Coronavirus Now:
Daily COVID-19 Updates for March 17
Confirmed cases of COVID-19 now number at more than 183,000 around the world as of March 17, 2020, including more than 4,500 cases in the United States alone. Once referred to as novel coronavirus, COVID-19 has disrupted lives across the globe, while the CDC is advising Americans to be prepared in case the virus spreads in their communities.
Here’s an update on the latest news about the coronavirus, including confirmed cases and deaths. The first section of this article will have the most recent news updates. The next two sections have maps and statistics on confirmed cases and deaths around the world.
There has been considerable controversy over the past year, particularly in Europe, over whether the World Health Organization (WHO) changed its definition of pandemic influenza in 2009 after novel H1N1 influenza was identified. Some have argued that not only was the definition changed but that it was done to pave the way for declaring a pandemic. Others claim that the definition was never changed and that this allegation is completely unfounded.
Such polarized views have hampered our ability to draw important conclusions. This impasse, combined with concerns over potential conflicts of interest and doubts about the proportionality of the response to the H1N1 influenza outbreak, has undermined the public trust in health officials and our collective capacity to effectively respond to future disease threats.
WHO did not change its definition of pandemic influenza for the simple reason that it has never formally defined pandemic influenza. While WHO has put forth many descriptions of pandemic influenza, it has never established a formal definition and the criteria for declaring a pandemic caused by the H1N1 virus derived from “pandemic phase” definitions, not from a definition of “pandemic influenza”.
The fact that despite ten years of pandemic preparedness activities no formal definition of pandemic influenza has been formulated reveals important underlying assumptions about the nature of this infectious disease. In particular, the limitations of “virus-centric” approaches merit further attention and should inform ongoing efforts to “learn lessons” that will guide the response to future outbreaks of novel infectious diseases.
In 2009, governments throughout the world mounted large and costly responses to the H1N1 influenza outbreak. These efforts were largely justified on the premise that H1N1 influenza and seasonal influenza required different management, a premise reinforced by the decision on the part of the World Health Organization (WHO) to label the H1N1 influenza outbreak a “pandemic”.
However, the outbreak had far less serious consequences than experts had predicted, a fact that led many to wonder if the public health responses to H1N1 had not been disproportionately aggressive.1–3 In addition, concern over ties between WHO advisers and industry fueled suspicion about the independence and appropriateness of the decisions made at the national and international levels.
Central to this debate has been the question of whether H1N1 influenza should have been labeled a “pandemic” at all. The Council of Europe voiced serious concerns that the declaration of a pandemic became possible only after WHO changed its definition of pandemic influenza. It also expressed misgivings over the WHO’s decision to withhold publication of the names of its H1N1 advisory Emergency Committee.3 WHO, however, denied having changed any definitions and defended the scientific validity of its decisions, citing “numerous safeguards” for handling potential conflicts of interest.
At stake in this debate are the public trust in health officials and our collective capacity to respond effectively to future disease threats. Understanding this controversy entails acknowledging that both parties are partially correct, and to resolve it we must re-evaluate how emerging threats should be defined in a world where the simple act of labeling a disease has enormous social, economic, and political implications.
Since 2003, the top of the WHO Pandemic Preparedness homepage has contained the following statement: “An influenza pandemic occurs when a new influenza virus appears against which the human population has no immunity, resulting in several simultaneous epidemics worldwide with enormous numbers of deaths and illness.” However, on 4 May 2009, scarcely one month before the H1N1 pandemic was declared, the web page was altered in response to a query from a CNN reporter.
The phrase “enormous numbers of deaths and illness” had been removed and the revised web page simply read as follows: “An influenza pandemic may occur when a new influenza virus appears against which the human population has no immunity.” Months later, the Council of Europe would cite this alteration as evidence that WHO changed its definition of pandemic influenza to enable it to declare a pandemic without having to demonstrate the intensity of the disease caused by the H1N1 virus.
We hope to learn every day. Make our world a better place but are we doing this. I hope no one takes this article as a gloom and doom post. That is not what it is meant to be. Sometimes when we are driving, our focus stays on what is in front of us. What about the peripheral vision? Are we aware of what is next to us or behind us? Most accidents are caused by a lack of attention to our surroundings. I think that is what is happening here with Covid19. We are so absorbed with it, the media is constantly talking about the Coronavirus. To the people who are dying from other diseases, I feel I owe you an apology.
Thank you for reading,
Michael
Comments are welcome

There have been so much deaths from different types of epidemic and pandemic over the years but not so many people know all about this. I am very happy to see you give so much details as you have given about this different diseases. The one I am more current with is the Ebola virus that spread alst year. I am happy it has been contained and I hope that this Corona virus will also be a thing of the past.
Hi Henderson,
Thank you for your comments. I am pretty sure the corona virus will be a thing of the past soon. The other diseases I listed have been around for centuries, and that is sad. We still have not found vaccines or cures for them.
Best wishes,
Michael
Hi Micheal,
Wow you have done your homework. This is getting pretty scary now. I am currently on lockdown in my home in the French Alps. We are not allowed to go outside unless it is for food, light exercise or medicine. There are still people faulting the rules 3 days in and the police and military are getting serious, and rightly so.
Luckily, we have no symptoms, but we know people that have got corona virus. I hope the rest of the world gets on board with the lockdowns asap.
Hi Tom.
Thank you for your comments. When people break the isolation rules, it feels like a form of disrespect to me. I am glad you are not having any symptoms, and are doing the right thing.
Best wishes,
Michael
Hi Michael – This is an informative history of the various epidemics and pandemics of the world. Regarding the controversy over declaring a novel infectious disease as a pandemic, perhaps there should be a category called a “potential” pandemic to trigger the proper protocol to avoid it from becoming a pandemic. This is what the WHO alteration seems to reflect. I wonder, when it comes to diseases and lives is there such a thing as an over response? Sometimes there is too much emphasis on money over lives To focus on your last paragraph, I think the covid19 virus is getting the attention it is getting is because it is highly contagious with no cure with basically no way to control it and people are dying as a result. Other diseases are more individual and non contagious.
Hi Nathaniel,
Thank you for your comments. You have hit on some key points. The emphasis on money, over lives always comes first. That is only my opinion. I think covid19 has similarities, “to over-response”. The coronavirus is affecting all these money-making countries. What about the third world countries where for instance, the mosquito-borne disease, “Dengue” is killing millions. This has been going on for so long without a vaccine, (well 1 vaccine that has been recalled so many times) and there is no cure.
Best wishes,
Michael
You make a fair point Michael. I hadn’t even heard of “Dengue.” Just know that there’s a reason the money-making countries are getting hit.
Thanks for responding!
The fact that i have come to learn something tangible from this post is satisfying. The make of your website is nice and the simplicity of the color selection makes it beautiful. there are some places in the world that has not been affected by this epidermic of covid 19.there is much hope for us
Hi Smoochi,
Thank you for your comments. Yes there are some places in the world that have not been affected by covid19. North Korea is one of them. I appreciate your comments on my website also, I know it is simple looking.
All the best,
Michael