What is Athlete’s Foot?
Blue indicates link
In this article, we’ll cover what tinea pedis is, its causes, symptoms, diagnosis, and treatments.
Athlete’s foot may be contagious and affects the skin on the feet. It also can spread to the toenails and therefore the hands. The mycosis is named athlete’s foot because it’s commonly seen in athletes.
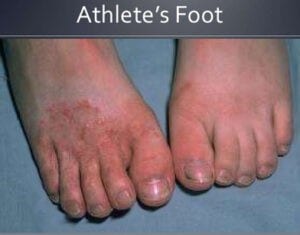
Athlete’s foot isn’t serious, but sometimes it’s hard to cure. If you’ve got diabetes or a weakened system and suspect you’ve got athlete’s foot, you ought to call your doctor directly.
It commonly occurs in people whose feet become very sweaty while confined within tight-fitting shoes.
Signs and symptoms of athlete’s foot include a scaly rash that sometimes causes itching, stinging, and burning. Athlete’s foot is contagious and may be spread via contaminated floors, towels, or clothing.
Athlete’s foot is closely associated with other fungal infections like ringworm and tinea cruris. It is often treated with over-the-counter antifungal medications, but the infection often recurs. Prescription medications also are available.
As its name indicates, an athlete’s foot commonly affects people who play sports, but you don’t need to be an athlete to urge it. Nail fungus may be a common complication also. Both conditions are caused by an equivalent sort of fungus called dermatophytes, which thrive in warm, moist places and sleep in dead skin tissue. These fungi also cause ringworm and jock itch. Athlete’s foot is a skin infection, while onychomycosis is an infection of the nail itself.
Athlete’s foot may be a term given to almost any inflammatory disease of the skin that affects only the foot and therefore the skin between the toes. It is usually scaly and should be a red, raw-appearing eruption with weeping and oozing with small blisters. It affects the feet of athletes and non-athletes alike. Although it’s frequently caused by a mycosis, other causes could also be indistinguishable without proper testing.
Types of Athlete’s Foot
If your feet are burning or itchy all the time, and if you see what seems like a rash on the skin, you’ll have athlete’s foot. But did you know that there’s more than one type?
A fungus causes this infection. One of the foremost common ways to select it up is to steer barefoot in places where germs hang around, like public pools or gym locker rooms.
You can also catch on if you share socks, bath towels, or bed sheets with someone who already has it.
The exact symptoms of an athlete’s foot depend upon which specific sort of infection you’ve got. Some types cause rashes that are red and blistery. With others, your skin could seem thick and scaly.
So which one might you have?
Toe Web Infection
Your doctor may call this an interdigital infection. That just means it’s between the fingers or toes.
It usually starts on the skin between your fourth and fifth toes. Sometimes bacteria take hold and make the mycosis worse.
Symptoms:
You may feel a burning sensation between your toes. The skin could also be red, peeling, or scaly, and therefore the rash may smell or give off the discharge. In very bad cases, your skin may combat a green color.
Moccasin Infection
If the fungus covers the sole of your foot, it’s called a moccasin infection. You may see the rash spread along your heel and up the side of your foot.
Symptoms:
At first, your feet may feel sore, dry, or slightly itchy. After a short time, the skin thickens, cracks, or peels. If the infection advances to your nails, your toenails can also get thick and crumbly. Sometimes the nails even come out.
Vesicular Infection
Vesicles are the medical term for blisters, and that’s exactly what marks this sort of infection. If the blisters burst, you’ll get a bacterial infection and wish antibiotics.
Symptoms:
Vesicular infections happen anywhere on your foot. But the tiny, red blisters usually crop up on your soles or between your toes. The rash may feel itchy or painful. It can be worse in the summer.
Ulcerative Infection
It’s unusual, but sometimes feet develop open sores or ulcers. Those ulcers also are a hospitable infection by bacteria. You’ll need antibiotics to treat this.
Symptoms:
In addition to sores which will ooze discharge, your skin gets very inflamed and discolored. This type of infection is usually very painful.
Symptoms:
An athlete’s foot usually causes a scaly red rash. The rash typically begins in between the toes. Itching is usually the worst right after you take off your shoes and socks. Some sorts of tinea pedis feature blisters or ulcers. The moccasin sort of tinea pedis causes chronic dryness and scaling on the soles that extend up the side of the foot. It can be mistaken for eczema or dry skin. The infection can affect one or both feet and may spread to your hand — especially if you scratch or pick at the infected parts of your feet.
Causes
Athlete’s foot is caused by an equivalent sort of fungus that causes ringworm and tinea cruris. Damp socks and shoes and warm, humid conditions favor the organisms’ growth. Athlete’s foot is contagious and may be spread by contact with an infected person or from contact with contaminated surfaces, like towels, floors, and shoes.
Risk factors
You are at higher risk of tinea pedis if you:
Are a man.
Frequently wear damp socks or tightfitting shoes
Share mats, rugs, bed linens, clothes, or shoes with someone who features a mycosis.
Walk barefoot publicly in areas where the infection can spread, like locker rooms, saunas, swimming pools, communal baths, and showers.
Walking barefoot in wet, dark areas frequented by many other individuals like indoor swimming bath decks, communal showers, and locker rooms end in frequent exposure to pathogenic fungi that cause athlete’s foot. Wearing occlusive footwear is assumed to play a big role in the increased frequency of athlete’s foot.
Exposure to moisture either from excessive sweating or from an external source may be a risk factor. Wearing equivalent shoes and socks for an extended period may damage the skin. Patients with diabetes are predisposed to develop athlete’s foot. Some believe that eczema can predispose one to tinea pedis. It appears that many more men have tinea pedis than women. Pedicures performed in contaminated environments can spread disease.
Complications
Your tinea pedis infection can spread to other parts of your body, including:
Your hand. People who scratch or pick at the infected parts of their feet may develop an identical infection in one of their hands.
Your nails. The fungi related to tinea pedis also can infect your toenails, a location that tends to be more immune to treatment.
Your groin. Jock itch is usually caused by an equivalent fungus that leads to tinea pedis. It’s common for the infection to spread from the feet to the groin because the fungus can travel on your hands or on a towel.
Diagnosis
In some cases, your doctor could also be ready to diagnose tinea pedis just by watching it. To help confirm the diagnosis and rule out other conditions, your doctor might take a skin scraping or skin sample from your foot for testing during a lab.
Treatment
If your tinea pedis is mild, your doctor may suggest using an over-the-counter antifungal ointment, cream, powder, or spray. If your tinea pedis doesn’t respond, you’ll need a prescription-strength medication to use on your feet. Severe infections may require antifungal pills that you take by mouth.
Lifestyle and home remedies
These tips can assist you to ease the symptoms of tinea pedis or avoid a recurrence:
Keep your feet dry, especially between your toes. Go barefoot to let your feet air out the maximum amount possible when you’re home. Dry between your toes after a shower or shower.
Change socks regularly. If your feet get very sweaty, change your socks twice each day.
Wear light, well-ventilated shoes. Avoid shoes made from synthetic material, like vinyl or rubber.
Alternate pairs of shoes. Don’t wear an equivalent pair a day in order to you give your shoes time to dry after each use.
Protect your feet in public places. Wear waterproof sandals or shoes around public pools, showers, and locker rooms.
Treat your feet. Use OTC antifungal products as directed daily. For example, creams could also be applied to dry feet twice each day and used every week even after the rash is gone.
Try not to scratch the rash. You can try soothing your wanderlust by soaking them in cool water.
Don’t share shoes. Sharing risks spreading a fungal infection.
In the majority of cases, athlete’s foot symptoms are mild, and therefore the patient doesn’t get to see a doctor.
OTC medications can be bought at pharmacies which are effective in clearing up the infection. In severe cases, a doctor may prescribe a more powerful antifungal medication, which is usually swallowed.
These kill the fungus that causes the symptoms.
Antifungal medications are available as:
tablets
powders
liquids
sprays
creams
Most topical medications can be bought OTC. Topical means it’s applied directly onto the skin. A pharmacist may recommend one of the following antifungal medications:
clotrimazole
econazole
ketoconazole
miconazole
terbinafine
sulconazole
These oral medications could be prescribed by a doctor, either because symptoms are severe, or if the topical medicines didn’t work:
griseofulvin
itraconazole
terbinafine
Antacids can interfere with the absorption of oral antifungals. Oral antifungals can also affect how some anticoagulant drugs work.
Elderly patients and young children shouldn’t tend to some sort of antifungals. Check with a pharmacist, doctor, or nurse, or read the leaflet that comes with the medication carefully.
Dosages may be different for children. Some of the medications are metabolized by the liver and may require blood work to make sure the patient’s liver is healthy before taking them.
Some antifungals shouldn’t be taken during pregnancy, while others may interfere with the male and feminine reproductive systems. Individuals who are pregnant, or planning to have children, should check with a doctor.
Hydrocortisone
If the skin is extremely sore and there is a lot of swelling, the doctor may recommend using hydrocortisone. Low-dose hydrocortisone medications can be bought OTC or online – higher doses will require a prescription.
Herbal and Natural Remedies
Add 40 drops of Organic Tea Tree Oil to a foot bath and soak your feet for 10 minutes. After soaking and thoroughly drying the feet, massage a couple of drops of the oil directly into the affected area. Tea tree oil has properties that will help destroy the fungus in heavily infested areas and deter it from spreading to unaffected areas.
Himalayan Crystal Salt and Apple Cider Vinegar
Soak your feet in 2 tablespoons of Himalayan Crystal salt and ½ cup Organic Apple vinegar solution mixed with some warm water. Vinegar creates a really acidic environment in which fungus cannot live. You can also spray your feet or wipe them down with a cloth soaked in this solution after you shower, just confirm you get them completely dry afterward. You can also wipe down the insides of shoes and sandals to help prevent the fungus from clinging there.
Make your feet stinkier by placing slices of fresh garlic, or some crushed garlic, between your toes and leaving them there for the day. Allicin, the active compound in garlic, inhibits the expansion of the fungus, the foremost common explanation for athlete’s foot. You can also add garlic to foods you eat or take a garlic supplement for an equivalent effect, but it’s going to take a touch bit longer.
Neem Oil
Organic neem oil, sometimes used as a pesticide, is another all-natural oil that is toxic to harmful organisms. Apply to clean, dry feet with a cotton ball.
Corn Starch and Baking Soda
Sprinkle your toes with a touch little bit of organic corn starch or bicarbonate of soda before putting on your socks in the morning. The corn starch or baking soda won’t stop the itch, but it will help soak up moisture. Baking soda within the shoes also absorbs a number of that not-so-pleasant sweaty foot smell.
Oregano Oil
Oregano contains essential oils that act against harmful organisms. Make a tea of 4 ounces of oregano leaves and just enough water to cover your feet. Soak your feet 2-3 times daily in this mixture. Some people say that you can reuse this tea for a week, but I recommend making it fresh each day.
Sesame and Coconut Oil
Both sesame and raw virgin coconut oil have antifungal properties and can be applied directly to the feet. Swab liberally on clean, dry feet with a cotton ball twice daily.
Ginger
You can also use organic ginger, just an ounce of fresh chopped ginger added to a cup of boiling water and simmered for 20 minutes. Once cooled, apply twice daily to clean feet. Ginger is a strong antifungal, and your feet will have a pleasantly spicy smell.
Ozonated Olive Oil
A relatively new therapy, ozonated olive oil, can also help with athlete’s foot. Ozone is a proven antifungal agent and can help heal damaged skin. Apply the paste to clean, dry feet each morning and night. This should clear up the fungus within two to four days and can discourage future outbreaks. I recommend an ozonated oil paste made with organic, cold-pressed olive oil such as O2-Zap®.
Colloidal Silver
Colloidal Silver is another common remedy for athlete’s foot with known antifungal properties. Spray or apply to your feet and let it fully dry. Alternatively, you can spray and leave the silver on your feet overnight. There are a lot of hucksters peddling shoddy colloidal silver. Only buy a high-quality product from a reputable company.
Always consult with your doctor before using alternative treatment methods.
Thank you for reading.
Michael
Comments are welcome.
This article helps me realize how I got fungi in my toenails and now I am bit less worried how to cure it through different remedies either OTC or oral anti-fungal medications. It is quite amazing that home remedies that we can find in our kitchen can also help cure the fungus. Thank you for this wonderful informations.
Hi Rose,
Thank you for your comments. Like you say it is amazing what certain things we have in our kitchen can be used as a remedy to many health issues.
All the best,
Michael