What is Psoriatic Arthritis?
Blue indicates link
Psoriatic arthritis is a form of arthritis that affects some people who have psoriasis — a condition that features red patches of skin topped with silvery scales. Most people develop psoriasis first and are later diagnosed with psoriatic arthritis, but the joint problems can sometimes begin before skin patches appear.
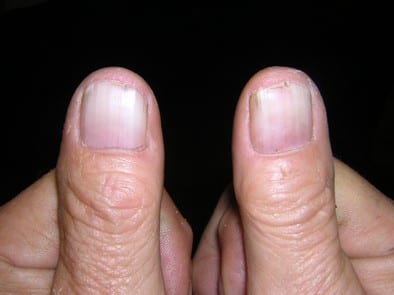
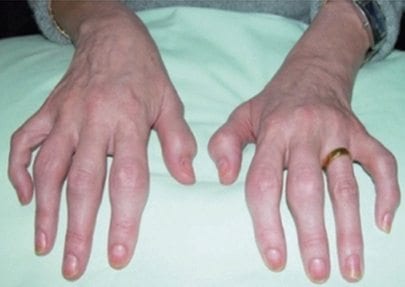
Joint pain, stiffness, and swelling are the main signs and symptoms of psoriatic arthritis. They can affect any part of your body, including your fingertips and spine, and can range from relatively mild to severe. In both psoriasis and psoriatic arthritis, disease flares may alternate with periods of remission.
No cure for psoriatic arthritis exists, so the focus is on controlling symptoms and preventing damage to your joints. Without treatment, psoriatic arthritis may be disabling.
Symptoms
Both psoriatic arthritis and psoriasis are chronic diseases that get worse over time, but you may have periods when your symptoms improve or go into remission alternating with times when symptoms become worse.
Psoriatic arthritis can affect joints on just one side or on both sides of your body. The signs and symptoms of psoriatic arthritis often resemble those of rheumatoid arthritis. Both diseases cause joints to become painful, swollen, and warm to the touch.
However, psoriatic arthritis is more likely to also cause:
- Swollen fingers and toes. Psoriatic arthritis can cause painful, sausage-like swelling of your fingers and toes. You may also develop swelling and deformities in your hands and feet before having significant joint symptoms.
- Foot pain. Psoriatic arthritis can also cause pain at the points where tendons and ligaments attach to your bones — especially at the back of your heel (Achilles tendinitis) or in the sole of your foot (plantar fasciitis).
- Lower back pain. Some people develop a condition called spondylitis as a result of psoriatic arthritis. Spondylitis mainly causes inflammation of the joints between the vertebrae of your spine and in the joints between your spine and pelvis (sacroiliitis).
Causes
Psoriatic arthritis occurs when your body’s immune system begins to attack healthy cells and tissue. The abnormal immune response causes inflammation in your joints as well as overproduction of skin cells.
It’s not entirely clear why the immune system attacks healthy tissue, but it seems likely that both genetic and environmental factors play a role. Many people with psoriatic arthritis have a family history of either psoriasis or psoriatic arthritis. Researchers have discovered certain genetic markers that appear to be associated with psoriatic arthritis.
Physical trauma or something in the environment — such as a viral or bacterial infection — may trigger psoriatic arthritis in people with an inherited tendency.
Risk factors
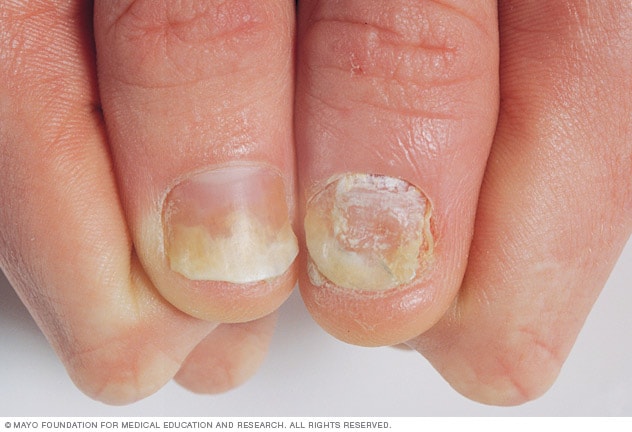
Psoriasis on the nails opens a pop-up dialog box
Several factors can increase your risk of psoriatic arthritis, including:
- Psoriasis. Having psoriasis is the single greatest risk factor for developing psoriatic arthritis. People who have pitted, deformed nails are especially likely to develop psoriatic arthritis.
- Your family history. Many people with psoriatic arthritis have a parent or a sibling with the disease.
- Your age. Although anyone can develop psoriatic arthritis, it occurs most often in adults between the ages of 30 and 50.
Complications
A small percentage of people with psoriatic arthritis develop arthritis mutilans — a severe, painful, and disabling form of the disease. Over time, arthritis mutilans destroy the small bones in the hands, especially the fingers, leading to permanent deformity and disability.
People who have psoriatic arthritis sometimes also develop eye problems such as pinkeye (conjunctivitis) or uveitis, which can cause painful, reddened eyes and blurred vision. They are also at higher risk of cardiovascular disease.
Diagnosis
During the exam, your doctor may:
- Closely examine your joints for signs of swelling or tenderness
- Check your fingernails for pitting, flaking, and other abnormalities
- Press on the soles of your feet and around your heels to find tender areas
No single test can confirm a diagnosis of psoriatic arthritis. However, some types of tests can rule out other causes of joint pain, such as rheumatoid arthritis or gout.
Imaging tests
- X-rays. Plain X-rays can help pinpoint changes in the joints that occur in psoriatic arthritis but not in other arthritic conditions.
- Magnetic resonance imaging (MRI). MRI uses radio waves and a strong magnetic field to produce very detailed images of both hard and soft tissues in your body. This type of imaging test may be used to check for problems with the tendons and ligaments in your feet and lower back.
Laboratory tests
- Rheumatoid factor (RF). RF is an antibody that’s often present in the blood of people with rheumatoid arthritis, but it’s not usually in the blood of people with psoriatic arthritis. For that reason, this test can help your doctor distinguish between the two conditions.
- Joint fluid test. Using a needle, your doctor can remove a small sample of fluid from one of your affected joints — often the knee. Uric acid crystals in your joint fluid may indicate that you have gout rather than psoriatic arthritis.
Treatment
No cure exists for psoriatic arthritis, so treatment focuses on controlling inflammation in your affected joints to prevent joint pain and disability.
Medications
Drugs used to treat psoriatic arthritis include:
- NSAIDs. Nonsteroidal anti-inflammatory drugs (NSAIDs) can relieve pain and reduce inflammation. Over-the-counter NSAIDs include ibuprofen (Advil, Motrin IB, others) and naproxen sodium (Aleve). Stronger NSAIDs are available by prescription. Side effects may include stomach irritation, heart problems, and liver and kidney damage.
- Disease-modifying antirheumatic drugs (DMARDs). These drugs can slow the progression of psoriatic arthritis and save the joints and other tissues from permanent damage. Common DMARDs include methotrexate (Trexall, Otrexup, others), leflunomide (Arava), and sulfasalazine (Azulfidine). Side effects vary but may include liver damage, bone marrow suppression, and severe lung infections.
- Immunosuppressants. These medications act to tame your immune system, which is out of control in psoriatic arthritis. Examples include azathioprine (Imuran, Azasan) and cyclosporine (Gengraf, Neoral, Sandimmune). These medications can increase your susceptibility to infection.
- Biologic agents. Also known as biologic response modifiers, this newer class of DMARDs includes abatacept (Orencia), adalimumab (Humira), certolizumab (Cimzia), etanercept (Enbrel), golimumab (Simponi), infliximab (Remicade), ixekizumab (Taltz), secukinumab (Cosentyx), tofacitinib (Xeljanz) and ustekinumab (Stelara). These medications target specific parts of the immune system that trigger inflammation and lead to joint damage. These drugs can increase the risk of infections. Higher doses of tofacitinib can increase the risk of blood clots in the lungs. Biologic agents can be used alone or combined with DMARDs, such as methotrexate.
- Newer oral medication. Apremilast (Otezla) decreases the activity of an enzyme in the body that controls the activity of inflammation within cells. Potential side effects include diarrhea, nausea, and headaches.
Surgical and other procedures
- Steroid injections. This type of medication reduces inflammation quickly and is sometimes injected into an affected joint.
- Joint replacement surgery. Joints that have been severely damaged by psoriatic arthritis can be replaced with artificial prostheses made of metal and plastic.
Lifestyle and home remedies
- Protect your joints. Changing the way you carry out everyday tasks can make a tremendous difference in how you feel. For example, you can avoid straining your finger joints by using gadgets such as jar openers to twist the lids from jars, by lifting heavy pans or other objects with both hands, and by pushing doors open with your whole body instead of just your fingers.
- Maintain a healthy weight. Maintaining a healthy weight places less strain on your joints, leading to reduced pain and increased energy and mobility. Losing weight if needed can also help your medications work better. Some psoriatic arthritis medications are less effective in people who have a body mass index of 25.0 to 29.9 (overweight). The best way to increase nutrients while limiting calories is to eat more plant-based foods — fruits, vegetables, and whole grains.
- Exercise regularly. Exercise can help keep your joints flexible and your muscles strong. Types of exercises that are less stressful on joints include biking, swimming, and walking.
- Stop smoking. Smoking is associated with a higher risk of developing psoriasis and with more severe symptoms of psoriasis.
- Limit alcohol use. Alcohol can increase your risk of psoriasis, decrease the effectiveness of your treatment, and increase side effects from some medications, such as methotrexate.
- Pace yourself. Battling pain and inflammation can leave you feeling exhausted. In addition, some arthritis medications can cause fatigue. The key isn’t to stop being active entirely but to rest before you become too tired. Divide exercise or work activities into short segments. Find time to relax several times throughout the day.
Coping and support
Psoriatic arthritis can be particularly discouraging because the emotional pain that psoriasis can cause is compounded by joint pain and, in some cases, disability.
The support of friends and family can make a tremendous difference when you’re facing the physical and psychological challenges of psoriatic arthritis. For some people, support groups can offer the same benefits.
A counselor or therapist can help you devise coping strategies to reduce your stress levels. The chemicals your body releases when you’re under stress can aggravate both psoriasis and psoriatic arthritis.
Weight Loss Diet
This is any basic diet that helps you shed pounds, which is a good thing. Being overweight can raise your risk for psoriatic disease. Losing weight can make psoriasis less severe. Doctors aren’t sure why this is, but they do know that fat tissue releases proteins that cause swelling. In a weight loss diet, you limit fats, sugars, and carbohydrates. You eat more fruits, vegetables, lean meats, and low-fat dairy items. When you lose weight, you’ll not only feel better — you’ll lower your risk of getting other diseases, too, like diabetes and high blood pressure.
Anti-Inflammatory Diet
Foods like fatty red meats, dairy, refined sugars, processed foods, and possibly vegetables like potatoes, tomatoes, and eggplants (you might hear them called nightshades) may all cause inflammation. Avoid them and choose fish, like mackerel, tuna, and salmon, which have omega-3 fatty acids. Those have been shown to reduce inflammation. Carrots, sweet potatoes, spinach, kale, and blueberries are good choices, too.
Autoimmune Protocol (AIP) Diet
This plan has an official-sounding name, but it’s really an offshoot of the paleo diet. You’ll cut back on gluten and refined sugar. There’s an elimination phase where you’ll avoid grains, legumes, nightshades, dairy, eggs, coffee, alcohol, sugar, oil, and food additives. The idea is to get rid of anything that might cause inflammation while bulking up on nutrient-dense foods, bone broth, fermented foods, and exercise. You can work the excluded foods back in slowly, figuring out what works for you and what doesn’t. This plan may help people with colitis and Crohn’s disease achieve remission. That’s promising news, though there are no studies on how it works with psoriatic arthritis.
Gluten-Free Diet
Research shows that as many as 25% of people with psoriasis may be sensitive to this protein that’s found in wheat and barley. You won’t find it in fruits and vegetables, rice, meat, beans, potatoes, and dairy. Talk to your doctor before you start this diet. They may test your blood to see if you’re allergic to gluten.
While doctors say there’s no such thing as a leaky gut or a specific diet for it, you’re still likely to hear about it. People who believe it say that bacteria and toxins enter your bloodstream through openings that result from Crohn’s disease or taking too much aspirin. In fact, research shows that a little bit of a leaky gut (your doctor might call it intestinal permeability) can help you absorb water and nutrients.
- Fad diets have popped up telling you to stay away from foods with high sugar content (whether they’re fruits or processed products) or that things like yeast, gluten, and lactose can damage your intestinal wall. If you have problems with these things, not eating them will make you feel better, as will cutting back on sugary, processed foods. Never trust anyone trying to sell you leaky gut diet products.
- Low-FODMAP DietAnother eating plan that works well for people with irritable bowel syndrome might be worth a try. FODMAP is a nickname for a group of carbohydrates called fermentable oligo-saccharides, disaccharides, monosaccharides, and polyols that are hard to digest. They’re found in fruits, honey, some dairy, wheat, onions, garlic, legumes, and artificial sweeteners. Though there’s no proof it works for psoriatic arthritis, you can cut them from your diet for 4 to 6 weeks, then gradually work them back in and see if you feel better.
- Mediterranean diet 2014 study showed that eating a diet high in extra-virgin olive oil could make psoriasis symptoms less severe. That’s because it has omega-3s. It also contains oleocanthal, which relieves swelling. If you choose this way of eating, you’ll get to have lots of cold-water fish, whole grains, fruits, and vegetables. Pagano Diet People with psoriasis said their symptoms improved while eating this plan, which calls for boosting fruits and veggies while cutting back on nightshades and junk food. But keep in mind that self-reported results are not the same as scientifically tested and proven results. Positive changes often follow when you add healthier foods to the menu. Paleo diet also called the caveman diet, this way of eating favors meat, fish, eggs, fruits, and vegetables. You’ll avoid all grains, beans, sugary snacks, and dairy. Doctors have no proof that the paleo diet stops PsA symptoms. But you could have less swelling because you’re not eating fatty foods and dairy products. Don’t get started with any of these diets until you get your doctor’s OK. They can keep track of the changes you’re making and determine whether they’ll help or worsen your PsA symptoms. Also, get exercise along with any food changes you make. It’s good for your joints and will also ease swelling and arthritic pain.
Foods to Avoid if You Have Psoriatic Arthritis
When you have psoriatic arthritis, you want to stay away from foods that can make the inflammation in your body worse. These include:
- Alcohol: It makes your liver work harder and disrupts the way your organs work together.
- Sugar: It sends out things called cytokines that create inflammation in your body.
- Processed foods: They contain trans fats that can start inflammation throughout your body.
- Diet soda: If it’s sweetened with aspartame, your body might think that’s a foreign substance and start an immune response.
- Fried foods: They contain trans fats that can start inflammation throughout your body.
- Processed meats: They contain saturated fats, which can make inflammation worse.
- Red meat: It contains saturated fats, which can make inflammation worse.
- Dairy: These foods contain saturated fats, which can make inflammation worse.
Anti-Inflammatory Foods for Psoriatic Arthritis
You can add these foods in place of the ones above to help keep inflammation in check:
-
- Fruits and vegetables: Go for berries and dark, leafy greens. They’re high in antioxidants, which keep your immune system healthy and may fight inflammation.
- Beans and whole grains: They’re high in fiber, which keeps levels of C-reactive protein (CRP) in your blood in check. High CRP can mean you have inflammation.
- Fatty fish, avocados, flaxseed oil, and olive oil: They’re high in omega-3 fatty acids, which cut the number of inflammatory proteins in your body.
- Turmeric, ginger, and cayenne: These spices all keep inflammation in check.
- Green, white, and black teas: They’re high in polyphenols, which rev your immune system.
Herbal/Alternative Remedies:
1. Turmeric (curcumin)
Turmeric is a yellow-colored spice used in a variety of cuisines, especially Indian food. The spice is well-known for its anti-inflammatory properties.
You can eat foods with turmeric, like Indian curries, or make turmeric tea. You can also take turmeric in pill form.
Look for supplements containing curcumin, an active ingredient in turmeric. Curcumin has been shown to block cytokines and enzymes that cause inflammation.
A 2016 review of several published studies found evidence supporting the effectiveness of turmeric (roughly 1,000 mg/day of curcumin) for improving arthritis symptoms like pain and stiffness.
High doses of turmeric can thin the blood. It’s recommended that you don’t take turmeric or curcumin if:
- You’re on blood thinners like warfarin (Coumadin)
- You’re having surgery
- you’re pregnant
2. Fish oil supplements
Fish oil is high in omega-3 fatty acids, which are anti-inflammatory.
A 2018 study showed that taking a fish oil daily supplement may improve joint tenderness and stiffness enough to help people with psoriatic arthritis reduce their dependence on NSAIDs.
Fish oil supplements might also improve heart function and protect against heart disease, according to a 2016 study. This could be an important finding since people with psoriatic arthritis are at higher risk for heart disease.
To add more omega-3s to your diet, increase your intake of fatty fish, like salmon, tuna, halibut, and cod, or take a fish oil supplement.
High levels of fish oil can interfere with some medications, such as warfarin (Coumadin), so talk to your doctor before taking a supplement.
Due to potentially dangerous levels of mercury, those who are pregnant or trying to conceive should avoid eating certain fish like:
- shark
- swordfish
- king mackerel
- albacore tuna
Taking vitamin D hasn’t been found to improve psoriatic arthritis, but some people with psoriatic arthritis have a vitamin D deficiency. Whether a supplement can help isn’t yet clear.
Vitamin D is important for general health, especially bone health. You can get this vitamin through sun exposure and from fortified foods like:
- milk
- orange juice
- cereal
Ask your doctor if you should also take a supplement.
4. Probiotics and prebiotics
Healthy bacteria called probiotics are believed to provide health benefits by supporting good bacteria that live in the gut.
In a 2015 study, people with psoriatic arthritis had less diversity of bacteria in their intestines compared to healthy participants.
Taking probiotics and prebiotics may help increase gut biodiversity. Prebiotics are substances that help good bacteria grow.
You can find probiotics in:
- yogurt
- fermented cheeses
- pickles
- sauerkraut
- kombucha
- tempeh
- Some types of milk
Probiotics are in foods like:
- dandelion greens
- garlic
- onions
You can also take probiotic or prebiotic supplements or both. Ask your doctor for advice.
5. Balneotherapy
The Dead Sea is located in Israel roughly 1,300 feet below sea level. It’s full of minerals and is very salty.
People have been soaking in the Dead Sea for centuries to improve the appearance of their skin and reduce inflammation.
Soothing a skin condition by bathing in mineral springs is known as balneotherapy. Only a few studies have looked at this remedy for psoriatic arthritis, but results have been promising.
If a trip to the Dead Sea isn’t feasible, you can purchase Dead Sea salts online. Another option is to try taking short, warm baths with Epsom salt to help reduce joint pain and inflammation.
6. Capsaicin
Capsaicin is a compound naturally found in chili peppers. It helps with arthritis pain by creating a numbing effect on pain receptors.
You can buy ointments, gels, and creams containing capsaicin in stores or online. Simply rub this product on the skin near your painful joints.
You can also find capsaicin patches that work for up to 8 hours at a time when applied directly to the skin. You might feel a burning sensation at first, but this should lessen over time.
7. Cold and heat
Heating pads loosen joints and relax aching muscles. Moist heat from a wet washcloth or warm bath can be especially soothing to sore joints.
Cold packs help reduce swelling and pain. Wrap the ice pack in a towel to avoid damaging your skin. You can alternate heat with cold as needed to help with arthritis symptoms.
8. Sleep
Fatigue is a common issue for people with psoriatic arthritis. Part of the reason for this pervasive tiredness is a lack of sleep.
A 2019 study published in the journal Dermatology and Therapy looked at sleep patterns in people with psoriasis and psoriatic arthritis.
Study results showed that nearly 60 percent of those involved in the study had trouble sleeping.
The research also found that almost 40 percent of them said they don’t sleep enough.
Getting enough sleep is important for preventing fatigue and improving your overall mood and quality of life.
Here are some tips on how to create proper sleep hygiene to help ensure a good night’s sleep:
- avoid caffeine and alcohol late in the day
- Exercise during the day
- Keep your room dark and cool
- Turn off all screens an hour before bedtime
- Avoid big meals before bed
- Take a relaxing bath or shower before bed
- go to bed and wake up at the same time each day
Getting the right treatment for psoriatic arthritis will also help you sleep better.
It may be that another treatable condition, like sleep apnea, is keeping you awake.
If you still aren’t getting enough rest, ask your doctor for recommendations such as a referral to a sleep specialist.
9. Stretching
Stretching is a vital part of psoriatic arthritis therapy. It prevents tightness and keeps you limber. Plus, it helps you avoid injuries when you exercise.
The National Psoriasis Foundation recommends 15 minutes of stretching as part of your daily exercise routine.
Work with a physical therapist or qualified personal trainer to create a daily stretching routine that works for you.
10. Exercise
Regular exercise has many benefits for people with psoriatic arthritis, including:
- preventing joint stiffness
- improving muscle strength, which can make daily tasks a little easier
- reducing stress and improving overall mood
- maintaining bone density
- reducing fatigue
- promoting weight loss, which takes the pressure off joints
- lowering the risk of cardiovascular disease and diabetes
Low-impact exercises are the easiest on painful joints. Swimming, yoga, Pilates, tai chi, walking, and cycling are good options.
Resistance training strengthens the muscles that support painful joints.
A 2018 study found that twice-weekly resistance training sessions improved functional ability, disease activity, and quality of life in people with psoriatic arthritis.
Warm up before exercising to prepare your body and prevent injury. Remember to stretch after each session, too.
A physical therapist can help you create an exercise plan that works well for you.
11. Massage
Massage is used to relieve muscle tension and reduce stress. A 2017 review of studies found massage helpful for relieving pain and improving strength and movement in people with arthritis.
However, it’s not clear whether it’s better than treatments like acupuncture or chiropractic care.
For best results, find a massage therapist who is trained to provide services for people with chronic conditions like psoriatic arthritis.
12. Acupuncture
Acupuncture is a form of traditional Chinese medicine in which practitioners place hair-thin needles into various pressure points around the body.
Inserting these needles promotes the release of natural pain relievers like serotonin and endorphins.
Research on using acupuncture for other forms of arthritis finds it helpful for relieving pain and improving movement and quality of life.
If you want to try this technique, see a licensed acupuncturist who has experience treating psoriatic arthritis. It’s important that they use clean needles and do not insert them into areas of skin with active flares.
13. Aloe vera
Aloe vera gel is possibly best known for soothing sunburns and helping wounds heal.
Research finds that a cream or gel containing aloe might also help relieve some of the redness, swelling, and scaling associated with psoriasis.
The National Psoriasis Foundation recommends creams containing 0.5 percent aloe. You can apply them up to 3 times daily.
14. Oregon grape
Mahonia aquifolium, also known as Oregon grape, is a medicinal herb with germ-killing properties.
In a 2018 review of studies, a cream or ointment containing 10 percent mahonia improved psoriasis symptoms with minimal side effects.
Unfortunately:
There’s no cure for psoriatic arthritis. However, a combination of the right medications and natural, at-home remedies can help you manage inflammation and joint pain.
Always speak with your doctor before using natural or alternative therapies, especially if you’re taking other medications.
Even if a natural remedy improves your symptoms, don’t stop taking your prescribed medication without consulting your doctor first.
Your diet is an essential part of relief from arthritis pain. That includes what you drink.
Thank you for reading
Michael
Comments are welcome
Amazing information! Arthritis is very serious and in this article you break down first what is Arthritis? Symptoms, like Swollen fingers and toes, Foot pain, and Lower back pain. What causes Arthritis? Risk factors like Psoriasis, Your family history, and your age. This is the information you need to be aware of your health!
Hi Darnell,
Thank you for your comments. This is an honor for me for you to comment on my article. Darnell Yeldon of the Lakers. Injuries also cause arthritis, I pray no one suffers from any form of arthritis. It is all about inflammation and this can all be controlled through diet.
All the best,
Michael