Let us start off by talking about the liver.
Blue indicates link
What is your liver?
The liver is a large, meaty organ that sits on the right side of the belly. Weighing about 3 pounds, the liver is reddish-brown and feels rubbery to the touch. Normally you can’t feel the liver, because it’s protected by the rib cage. The liver has two large sections, called the right and the left lobes. The gallbladder sits under the liver, along with parts of the pancreas and intestines. The liver and these organs work together to digest, absorb, and process food.
The liver’s main job is to filter the blood coming from the digestive tract, before passing it to the rest of the body. The liver also detoxifies chemicals and metabolizes drugs. As it does so, the liver secretes bile that ends up back in the intestines. The liver also makes proteins important for blood clotting and other functions.
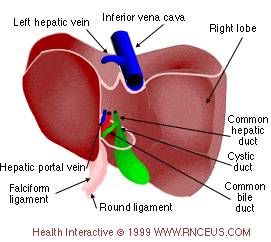
More on the liver:
The liver is an organ about the size of a football that sits just under your rib cage on the right side of your abdomen. The liver is essential for digesting food and ridding your body of toxic substances.
Liver disease can be inherited (genetic) or caused by a variety of factors that damage the liver, such as viruses and alcohol use. Obesity is also associated with liver damage.
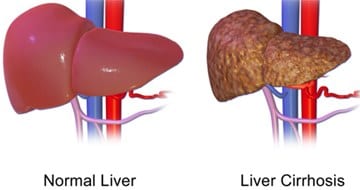
Over time, damage to the liver results in scarring (cirrhosis), which can lead to liver failure, a life-threatening condition.
What does the Liver do?
Known as the second-largest organ in the body after the skin, the liver has over 500 functions, including helping the blood clot and breaking down damaged cells. Weighing between two and three pounds, it holds about 13 percent of the body’s total blood volume. The liver has the distinction of being both a gland and an organ. As an organ, it can execute chemical actions, and as a gland, it secretes chemicals for other parts of the body to use.
The liver is a metabolically active organ responsible for many vital life functions. The primary functions of the liver are:
- Bile production and excretion
- Excretion of bilirubin, cholesterol,
hormones, and drugs - Metabolism of fats, proteins, and
carbohydrates - Enzyme activation
- Storage of glycogen, vitamins, and
minerals - Synthesis of plasma proteins, such as
albumin, and clotting factors - Blood detoxification and purification
What is Bile?
Bile is a fluid that is made and released by the liver and stored in the gallbladder. Bile helps with digestion. It breaks down fats into fatty acids, which can be taken into the body by the digestive tract.
Bile contains:
- Mostly cholesterol
- Bile acids (also called bile salts)
- Bilirubin (a breakdown product of red blood cells)
It also contains:
- Water
- Body salts (such as potassium and sodium)
- Copper and other metals
What does bile do?
Bile contains bile acids, which are critical for digestion and absorption of fats and fat-soluble vitamins in the small intestine. Many waste products, including bilirubin, are eliminated from the body by secretion into bile and elimination in feces. Bile is a complex fluid containing water, electrolytes, and a battery of organic molecules including bile acids, cholesterol, phospholipids, and bilirubin that flows through the biliary tract into the small intestine.
Bilirubin:
Bilirubin is a yellow compound that occurs in the normal catabolic pathway that breaks down heme in vertebrates. This catabolism is a necessary process in the body’s clearance of waste products that arise from the destruction of aged or abnormal red blood cells.
Phospholipids:
Phospholipids are a class of lipids that are a major component of all cell membranes. They can form lipid bilayers because of their amphiphilic characteristics. The structure of the phospholipid molecule generally consists of two hydrophobic fatty acid “tails” and a hydrophilic “head” consisting of a phosphate group.
Well, I think we have covered enough about the basic liver functions.
What is happening in our world today that is causing liver disease?
Most of us have grown to associate liver disease with overconsumption of alcohol, but there are many other factors.
We live in an increasingly toxic world. But did you know that over 80,000 chemicals contaminate the air, water, and food supply?
Here are the top 10 toxins that we’re exposed to on a daily basis…
Tobacco smoke
Prescription and OTC medications
Dental fillings (mercury is a toxic heavy metal!)
Bisphenol A (found in water bottles and food storage containers)
Artificial fragrance (3,000 chemicals in this category!)
Teflon (from anti-stain coatings on furniture and carpets)
Air pollution (indoor and outdoor)
Pesticides (RoundUp is the worst and it’s everywhere!!)
Your Liver is responsible for neutralizing all these toxins so that they don’t kill you.
This is why most people are walking around with a compromised liver that’s been beaten up by working overtime… for decades… without a break!
This is a big deal because the poor liver function can increase the risk of many diseases like:
Autoimmune disorders (Hashimoto’s, lupus, MS, etc.)
Cancer
Dementia
Diabetes
Heart problems
Hormone imbalances
Thyroid problems
Skin issues
It is vital to keep your liver healthy. From my understanding liver disease is nasty and if neglected fatal!
Liver disease is more commonly associated with men, but there is an increase in liver disease in women and that is one of the reasons I have chosen the topic. Liver Disease and Women.
We have touched on some of the reasons why liver damage occurs, and that is due to the increased amount of toxins we breathe every day. Yes, this includes children!
What are the Symptoms of Liver Disease:
- Skin and eyes that appear yellowish (jaundice)
- Abdominal pain and swelling
- Swelling in the legs and ankles
- Itchy skin
- Dark urine color
- Pale stool color, or bloody or tar-colored stool
- Chronic fatigue
- Nausea or vomiting
- Loss of appetite
- The tendency to bruise easily
The symptoms of liver damage in women are similar to those in men. These symptoms may include yellowing of the skin and eyes, a condition called jaundice, tea-colored urine, and generalized itching. In addition, the liver may look and feel enlarged, and the patient may have little or no appetite. In addition, a person may experience include weight loss, nausea and vomiting, and clay-colored stools. Sometimes a blocked bile duct can contribute to clay- or light-colored stools as well.
Typically, early symptoms of liver damage in women are vague. They may include bloating, excessive gas, and pain in the upper right quadrant of the abdomen. Although these symptoms can be mild and due to other, less serious conditions, they must be evaluated by the physician. As symptoms of liver damage in women become worse, the patient may even display confusion and lethargy. This happens because liver damage can cause high amounts of ammonia to be released into the bloodstream, causing confusion and sleepiness.
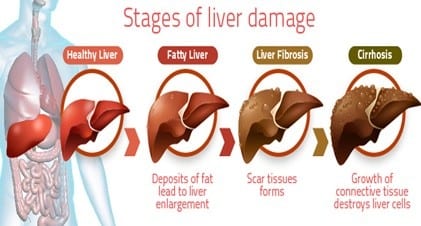
Primary liver damage can be caused by excessive intake of alcohol, leading to cirrhosis of the liver, diabetes, and hepatitis. In addition, gallbladder disease can cause liver damage in women. Although the liver can repair itself, extensive liver damage may be permanent. In addition, certain medications and illicit drugs can also contribute to liver damage in both men and women. For example, taking pain relievers while drinking alcohol may result in liver damage and many times, the condition is irreversible.
Treating liver damage depends upon the underlying cause. For example, if the liver damage is caused by cirrhosis, refraining from consuming alcoholic beverages may result in an improvement. Similarly, if liver damage is related to medications or drugs, stopping the drugs may result in a reversal of liver damage. Since diabetes can contribute to liver damage in women and men, diabetic patients must comply with the medication regimen and follow their physician’s recommendations for a healthy diet and exercise program.
Women are more commonly affected by toxin-mediated liver disease, such as alcohol- and drug-induced liver disease, and have an increased prevalence of acute liver failure. Women are more susceptible than men to the toxic effects of alcohol on the liver for any given dose of alcohol, even though men abuse or depend on alcohol more than women, at a ratio of 2:1 in persons over the age of 26 years. A 12-year prospective study of alcohol use in over 13,000 participants in Denmark showed that the risk of development of alcohol-related liver disease increased in women who consumed 7 to 13 beverages per week (84-156 g) compared with men who consumed 14 to 27 beverages per week.
Among persons who consumed 28 to 41 beverages per week (336-492 g), the relative risk of alcohol-induced cirrhosis was 7.0 (95% CI, 3.8-12.8) in men vs. 17.0 (95% CI, 6.8-40.8) in women. However, alcoholic cirrhosis is less frequently diagnosed in women, as shown in a population-based registry of 8482 Danish patients from 1993 to 2005 in which only 33% of patients were women.
Compared with their male counterparts, women with alcoholic liver disease have a more rapid progression to fibrosis that persists even after abstinence from alcohol. Dietary factors are known to influence the development of alcoholic liver disease. An analysis of 107,000 women from the United Kingdom suggests that the combination of high body mass index (BMI) and high alcohol intake increases the development of chronic liver disease.
Whether there is a survival difference between the sexes regarding alcoholic liver disease is less clear. In a prospective study of 490,000 men and women in the United States who were followed for 9 years, the relative risk of death from cirrhosis or alcoholism was equal in both sexes for those consuming 2 to 3 drinks per day but was increased in men who consumed 4 or more drinks per day.
Women are more likely to present with drug-induced hepatotoxicity and acute liver failure than men. Prospective data from the Acute Liver Failure Study Group, which included 23 sites from 1998 to 2007, showed that 67% of the 1147 patients were women. Among 133 cases of drug-induced liver injury assessed, 71% were in women, and women accounted for over 70% of all patients hospitalized with acute liver injury due to acetaminophen and idiosyncratic drug reactions. However, gender is not a predictor of survival in acute liver failure.
Women are 10 times more likely to have primary biliary cirrhosis (PBC) than men and 4 times as likely to have autoimmune hepatitis. The exact mechanism of gender differences in autoimmune liver disease and autoimmunity, in general, is not known; however, both immunogenetics and sex hormones play a complex and, perhaps, interactive role. Sex steroids alter the immune system on many levels: they can regulate gene expression through steroid-responsive elements, alter antigen
presentation through effects on human leukocyte antigen genes, and alter the cytokine environment. Additionally, X chromosome monosomy and fetal microchimerism (the presence of fetal cells in maternal circulation) may play a role in the pathogenesis of PBC. In the case of PBC, epidemiologic studies also have shown different environmental risk factors between sexes, including hair dye use, recurrent urinary tract infections, smoking, and estrogen deficiency, all of which may contribute to increased disease in women.
In patients with PBC, overall survival is similar between both sexes. Women with PBC present at a younger age with increased rates of pruritus and appear to have slower rates of fibrosis than men. In patients with autoimmune hepatitis, the rates of progression to cirrhosis, treatment failure, and death from liver failure were equivalent in men and women.
Estrogen levels are thought to be associated with benign liver tumors, although the potential mechanisms are unclear. The data are inconsistent in determining whether there are increased hormone receptors on benign tumors and whether exogenous estrogens, such as oral contraceptive pills (OCPs), stimulate benign tumor growth. The evidence regarding OCP’s influence on benign liver lesions is most compelling for adenomas, with 80% of women reporting OCP use. Therefore, discontinuation of OCPs is recommended for such patients.
For other liver lesions, there is less convincing evidence for the role of OCPs in tumor progression. A small case-control study suggested that patients taking OCPs were at increased risk of FNH. However, a study of 136 women followed for 9 years did not show an association in size or number of FNH lesions in OCP users. The overall survey of the literature suggests no increased risk of FNH or change in the character of FNH on OCPs, and discontinuation is not recommended in these patients.
Likewise, there is debate over whether estrogen use increases rates of cavernous hemangiomas. In a study of 94 women followed from 1986 to 2003 (mean follow-up of 7 years), there was a trend toward an increased incidence of cavernous hemangiomas and hormone therapy, but this trend was not statistically significant.
Personal Note:
There are certain things that are beyond our control. We try to control the number of toxins in the air we breathe, yet there are certain polluters out that have a lack of respect. I listen to stories about climate change, I watch people in certain countries having to wear a mask just to go outside of their homes. My gosh, we are entering 2020 and I consider ourselves an advanced society.
Please look after yourself. Exercise, if you feel like a drink, by all means, enjoy it in moderation. I know smoking is a hard habit to quit, but give your life a chance. My site is dedicated to you empower yourself in a healthy fashion. The alternatives are there. I am a recovering alcoholic, I choose not to have that one drink. For me, one drink is one too many and a thousand is not enough.
Liver and Kidney Foods. Please click on the link below.
https://www.pinterest.ca/sherardm/liver-and-kidney-foods/
Thank you for reading,
Michael.
Comments are welcome
I have studied the liver many times in the past due to my love for biology, and you give a detailed account of the liver, its position (although not scientifically labelled), and the many functions it has. I like how you are emphasising the need of the liver as I hope it raises an awareness about treating your liver with care, thus not drinking as much.
Additionally, the fact that there are gender differences in susceptibility to diseases is quite amazing. Don’t you think?
Hi Conor,
Thank you for your comments. You obviously have a great knowledge about the liver. I merely scratched the surface in my post. I apologize for not labeling the liver in more detail, something I will change. Awareness is necessary for us to take the proper steps to live a healthy life. For the longest time alcohol was thought to be the only toxin that caused damage to the liver.
Best wishes,
Michael
Thank you for your post. It is informative and helpful to anyone who is interested in the liver and its associated conditions. I particularly like your description on the top 10 toxins that our liver is responsible to neutralize.
I know that our liver is critical to degrade alcohol, but am not aware of many other toxins that liver is also critical to detox, such as smoking and air pollution. These toxins are from lungs and I don’t know how they could reach liver, may be through the circulation system? If this is true, then these toxins could be in all parts of human body. it is so dangerous and we need to try our best to prevent them reaching our lung in the first place.
It is kind of you sharing the life-saving information with us.
Hi Anthony,
Thank you for your comments. Seems like the liver works as the central filtering organism in the human body. For the longest time it was thought that alcohol was the main reason for liver damage. It certainly is the greatest contributor, but scientists are becoming more aware of other significant toxins that can cause severe liver damage.
Best wishes,
Michael