What are Varicose Veins?
Blue indicates link
Varicose veins are superficial veins that have become enlarged and twisted. Typically, they occur just under the skin in the legs. Usually, they result in few symptoms but some may experience fullness or pain in the area. Complications may include bleeding or superficial thrombophlebitis. When varices occur in the scrotum it is known as a varicocele while those around the anus are known as hemorrhoids. Varicose veins may negatively affect the quality of life due to their physical, social, and psychological effects.
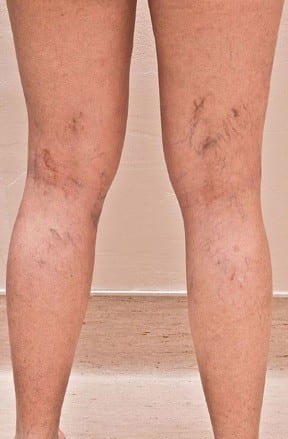
Varicose veins are twisted, enlarged veins. Any superficial vein may become varicose, but the veins most commonly affected are those in your legs. That’s because standing and walking upright increases the pressure in the veins of your lower body.
For many people, varicose veins and spider veins — a common, mild variation of varicose veins — are simply a cosmetic concern. For other people, varicose veins can cause aching pain and discomfort. Sometimes varicose veins lead to more serious problems.
Varicose veins may not cause any pain. Signs you may have varicose veins include:
- Veins that are dark purple or blue in color
- Veins that appear twisted and bulging; are often like cords on your legs
When painful signs and symptoms occur, they may include:
- An achy or heavy feeling in your legs
- Burning, throbbing, muscle cramping, and swelling in your lower legs
- Worsened pain after sitting or standing for a long time
- Itching around one or more of your veins
- Skin discoloration around a varicose vein
Spider veins are similar to varicose veins, but they’re smaller. Spider veins are found closer to the skin’s surface and are often red or blue.
Spider veins occur on the legs, but can also be found on the face. They vary in size and often look like a spider’s web.
When to see a doctor:
Self-care — such as exercise, elevating your legs, or wearing compression stockings — can help you ease the pain of varicose veins and may prevent them from getting worse. But if you’re concerned about how your veins look and feel and self-care measures haven’t stopped your condition from getting worse, see your doctor.
Causes:
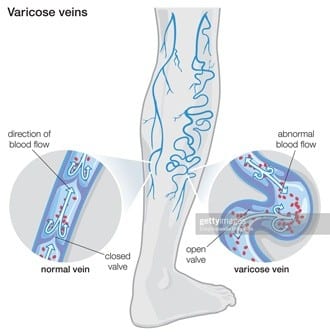
Weak or damaged valves can lead to varicose veins. Arteries carry blood from your heart to the rest of your tissues, and veins return blood from the rest of your body to your heart, so the blood can be recirculated. To return blood to your heart, the veins in your legs must work against gravity.
Muscle contractions in your lower legs act as pumps and elastic vein walls help blood return to your heart. Tiny valves in your veins open as blood flows toward your heart then close to stop blood from flowing backward. If these valves are weak or damaged, blood can flow backward and pool in the vein, causing the veins to stretch or twist.
Varicose veins occur when veins aren’t functioning properly. Veins have one-way valves that prevent blood from flowing backward. When these valves fail, blood begins to collect in the veins rather than continuing toward your heart. The veins then enlarge. Varicose veins often affect the legs. The veins there are the farthest from your heart, and gravity makes it harder for the blood to flow upward.
Some potential causes for varicose veins include:
- pregnancy
- menopause
- age over 50
- standing for long periods of time
- obesity
- family history of varicose veins
Symptoms of varicose veins:
The primary symptoms of varicose veins are highly visible, misshapen veins, usually on your legs. You may also have pain, swelling, heaviness, and achiness over or around the enlarged veins.
In some cases, you can develop swelling and discoloration. In severe cases, the veins can bleed significantly, and ulcers can form.
Diagnosing varicose veins:
Your doctor will likely examine your legs and visible veins while you’re sitting or standing to diagnose varicose veins. They may ask you about any pain or symptoms you’re having.
Your doctor may also want to do an ultrasound to check your blood flow. This is a noninvasive test that uses high-frequency sound waves. It allows your doctor to see how blood is flowing in your veins.
Depending on the location, a venogram may be done to further assess your veins. During this test, your doctor injects a special dye into your legs and takes X-rays of the area. The dye appears on the X-rays, giving your doctor a better view of how your blood is flowing.
Tests such as ultrasounds or venograms help ensure that another disorder like a blood clot or a blockage isn’t causing the pain and swelling in your legs.
Treating and preventing varicose veins:
In general, doctors are conservative when treating varicose veins. You’ll probably be advised to make changes to your lifestyle, instead of trying more aggressive treatments.
Lifestyle changes:
The following changes may help prevent varicose veins from forming or becoming worse:
- Avoid standing for extended periods of time.
- Lose weight or maintain a healthy weight.
- Exercise to improve your circulation.
- Use compression socks or stockings.
Your online catalog links to compression socks or stockings.
If you already have varicose veins, you should take these steps to prevent new varicose veins. You should also elevate your legs whenever you’re resting or sleeping.
Compression:
Your doctor may advise you to wear special compression socks or stockings. These place enough pressure on your legs so that blood can flow more easily to your heart. They also decrease swelling.
The level of compression varies, but most types of compression stockings are available in drugstores or medical supply stores.
Surgery:
If lifestyle changes aren’t working, or if your varicose veins are causing a lot of pain or damaging your overall health, your doctor might try an invasive procedure.
Vein ligation and stripping is a surgical treatment that requires anesthesia. During the procedure, your surgeon makes cuts in your skin, cuts the varicose vein, and removes it through the incisions. Although updated variations of vein-stripping surgeries have been developed, they are less commonly performed because newer, less invasive options are available.
Other treatment options:
Currently, a wide variety of minimally invasive treatment options for varicose veins are available. These include:
- sclerotherapy, using a liquid or foam chemical injection to block off a larger vein
- micro sclerotherapy, using a liquid chemical injection to block off smaller veins
- laser surgery, using light energy to block off a vein
- Endovenous ablation therapy uses heat and radiofrequency waves to block off a vein
- endoscopic vein surgery, using a small lighted scope inserted through a small incision to block off a vein
You should always talk to your doctor about your treatment options and the risks before choosing a method. The method recommended can depend on your symptoms, size, and location of the varicose vein.
Outlook for people with varicose veins:
Varicose veins normally get worse over time. This is true even if you make the necessary lifestyle changes to control them and manage your pain. While they may be unsightly, they usually don’t cause any long-term medical problems.
In some cases, varicose veins can lead to ulcers or sores on your legs, blood clots, or chronic inflammation. If you have a severe case, your veins could rupture.
You should see your doctor if you develop any of these symptoms. They may then suggest taking a more aggressive approach, such as surgery or other interventions.
What Are the Treatments for Varicose Veins?
A mild case of varicose veins does not usually require a doctor’s care. You can find relief from the discomfort of varicose veins with basic at-home treatment and various alternative remedies.
Superficial varicose veins normally do not require medical attention, but they should not be ignored. To relieve the discomfort, your doctor may recommend the following:
Compression stockings, which you can buy in most pharmacies and medical supply stores. Over-the-counter stockings include the support pantyhose offering the least amount of pressure and the compression hose offering more pressure. Higher-pressure compression stockings provide the most pressure and require a prescription.
Compression stockings are designed to help your leg muscles push blood upward by providing graduated compression with the strongest support starting at the ankles and gradually decreasing upward. Put them on before you get out of bed in the morning. Raise your legs in the air and pull the stockings on evenly; they should not feel tight in the calf or groin. You should wear them all day and also elevate your legs for 10-15 minutes several times throughout the day.
An over-the-counter anti-inflammatory drug such as aspirin or ibuprofen to alleviate occasional swelling and pain.
If you notice the skin around a varicose vein becoming ulcerated or discolored, or if you have continuing pain with no obvious outward signs, contact a doctor at once about the possibility of deep vein involvement.
Medical Procedures:
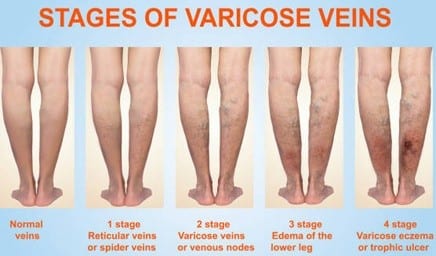
Most varicose veins do not need to be removed. If particularly bothersome, varicose veins can be eliminated by one of several methods:
- Laser treatment in which light energy from a laser is directed at the vein causing it to gradually fade or disappear; multiple treatments are required and the procedure is used to treat small varicose veins.
- Sclerotherapy, in which a chemical is injected into the vein to collapse its walls so it can no longer transport blood
- ablation with catheter-assisted methods that use heat with radiofrequency waves or lasers to destroy and ultimately close the vein
- Surgical removal, or stripping
Unfortunately, no treatment can prevent new veins from becoming varicose. Before pursuing a particular treatment, discuss all options with a dermatologist or vascular surgeon.
Herbal Remedies for Varicose Veins
Butcher’s broom, St. John’s wort, and witch hazel are particularly helpful in relieving the ache and discomfort of varicose veins and hemorrhoids.
Butcher’s broom, contains compounds called ruscogenins. These substances decrease inflammation while constricting the vein. Taken internally, 100 mg ruscogenins — usually a whole herb extract — taken three times per day is beneficial. German researchers verify that this herb helps to tighten, strengthen, and decrease inflammation in veins, helping blood flow up the legs. A compress of butcher’s broom may be applied externally.
St. John’s wort also reduces inflammation and is used externally and internally for both ailments. Use it externally in salves, oils, or tinctures, rubbing them into the affected area. Drink infusions of St. John’s wort to provide nutrients and compounds that will nourish the stressed veins. This herb should be used fresh or freeze-dried, as it loses its medicinal properties if air-dried.
Witch hazel, the famous astringent herb, is full of tannins, gallic acids, and essential oils. While you can take it internally as a tea, it is best to make a strong decoction for use as a compress. When applied to hemorrhoids, witch hazel reduces pain and swelling. It also tightens and soothes aching varicose veins and reduces inflammation.
When applied externally, lavender, too, will reduce inflammation and help heal these enlarged vessels. Yarrow, horse chestnut, calendula tincture, and chamomile are also helpful when used topically.
Flavonoid-rich foods, help reduce the risk of developing varicose veins and hemorrhoids because of their strengthening action on the veins. These compounds reduce fragility and tone the muscles that line the walls of the vessels. Blue, red, and purple foods, such as berries, cherries, and plums, are rich in flavonoids, as are some herbs such as St. John’s wort, hawthorn, linden flowers, and bilberry.
Rosemary, not only strengthens and protects vessels with its antioxidants but also improves circulation, thus helping to alleviate both varicose veins and hemorrhoids. Use liberally in foods, and make a liniment to apply topically.
Keeping circulation and weight control in mind can help prevent swollen veins. And, whether seeking to prevent or treat varicose veins with a compress, herbal remedies involving herbs such as rosemary and witch hazel may offer help and, hopefully, relief.
Many complementary or alternative treatments have been used for varicose veins. These include vitamin supplements, homeopathy, and acupuncture.
However, the most established of these alternative varicose vein treatments is in the use of herbal medicines, especially those containing extracts of horse chestnut seed.
Many will recognize the horse chestnut seed as the conker. These have, at various times, been used as cattle feed, as well as furnishing children with ammunition for conker battles.
Herbalists have a long tradition of using horse chestnut seeds to treat varicose veins. The herb is now prescribed by doctors in countries such as Switzerland and Germany where it is routinely considered as a treatment of choice, filling the gap between the use of compression stockings and more invasive methods such as injections or surgery.
Horse chestnut seeds contain active substances, particularly one known as β-aescin. A large amount of research information is available in the public domain on how horse chestnut seed extracts work.
Although pregnant women are susceptible to varicose veins, horse chestnut should not be taken internally. Instead, use Horse Chestnut seed gel applied externally.
Risk factors
These factors increase your risk of developing varicose veins:
- Age. The risk of varicose veins increases with age. Aging causes wear and tear on the valves in your veins that help regulate blood flow. Eventually, that wear causes the valves to allow some blood to flow back into your veins where it collects instead of flowing up to your heart.
- Sex. Women are more likely to develop the condition. Hormonal changes during pregnancy, pre-menstruation, or menopause may be a factor because female hormones tend to relax vein walls. Hormone treatments, such as birth control pills, may increase your risk of varicose veins.
- Pregnancy. During pregnancy, the volume of blood in your body increases. This change supports the growing fetus but also can produce an unfortunate side effect — enlarged veins in your legs. Hormonal changes during pregnancy may also play a role.
- Family history. If other family members had varicose veins, there’s a greater chance you will too.
- Obesity. Being overweight puts added pressure on your veins.
- Standing or sitting for long periods of time. Your blood doesn’t flow as well if you’re in the same position for long periods.
Complications
Complications of varicose veins, although rare, can include:
- Ulcers. Painful ulcers may form on the skin near varicose veins, particularly near the ankles. A discolored spot on the skin usually begins before an ulcer forms. See your doctor immediately if you suspect you’ve developed an ulcer.
- Blood clots. Occasionally, veins deep within the legs become enlarged. In such cases, the affected leg may become painful and swell. Any persistent leg pain or swelling warrants medical attention because it may indicate a blood clot — a condition known medically as thrombophlebitis.
- Bleeding. Occasionally, veins very close to the skin may burst. This usually causes only minor bleeding. But any bleeding requires medical attention.
Prevention:
There’s no way to completely prevent varicose veins. However, improving your circulation and muscle tone may reduce your risk of developing varicose veins or getting additional ones. The same measures you can take to treat the discomfort from varicose veins at home can help prevent varicose veins, including:
- Exercising
- Watching your weight
- Eating a high-fiber, low-salt diet
- Avoiding high heels and tight hosiery
- Elevating your legs
- Changing your sitting or standing position regularly
Herbal Remedies. Please click for prices and catalog
Images, Treatments, Varicose Veins. Please highlight and go to the link below.
https://www.pinterest.ca/sherardm/varicose-veins/
Personal Note:
For some people, this can be embarrassing. I know this beautiful young lady who stays away from going swimming and always wears pants. If we were to look at beauty through the outward appearance of someone, then we need to make some major adjustments to our way of thinking.
Thank you for reading,
Michael
Comments are welcome.



Personally, I think exercising and wearing compression socks are the two best ways to battle varicose veins. I know those won’t help everyone, but I think if most people exercised regularly and got into the habit of wearing compression socks, then they would see improvement within a few months. I actually didn’t know laser therapy was an option, though.
Hi Nate,
Thank you for your comments. I do think compression socks and exercise goes together. I was not aware of the different stages of varicose veins though. Sometimes it the little things we should pay detail to that can make a difference.
Best wishes,
Michael
My girlfriend is feeling ashamed of her varicose veins in her legs which were acquired through her prolonged standing working as a teacher. Reading the suggestions here, I realized that if someone can’t avoid standing for a very long time as it is part of their work, at least they should reduce their bodyweight so as to lessen the pressure that’s leading to the development of varicose veins in the legs. She’s still young, at her 20s, so maybe we can still do something to correct those problems.
Hi Gomer,
Thank you for your comments. I too have a very precious friend that is so conscious about her varicose veins which are only on her legs that she sometimes forgets how really beautiful she is. Your girlfriend is young, please look through those images and information about essential oils, even Bragg apple cider and work with her. Yes the two of you can correct varicose veins.
Best wishes to you and your girlfriend,
Michael
Good information on varicose veins! It seems like a terrible part of getting these is seeing it on your leg and not knowing what is going on/what it is yet. Seeing veins like that might make me scared at first. Luckily, the concerns of them occurring aren’t terrible and there are ways to treat them. I feel like I have heard the most about laser therapy to treat them. Varicocele would be terrible to have. I actually know somebody that did and that is why him and his wife could not get pregnant. Luckily they were able to before he had a painful treatment to correct them. Thanks for the information!
Hi Andrew,
Thank you for your comments. I was a bit shocked at how bad varicose veins could get. Thank you for sharing your friends story.
Best wishes,
Michael
Hello, While reading I know that Varicose veins normally get worse over time. The primary symptoms of varicose veins are highly visible, misshapen veins, usually on our legs. We may also have pain, swelling, heaviness, and achiness over or around the enlarged veins. We will probably be advised to make changes to our lifestyle, instead of trying more aggressive treatments. Your guide is very helpful for everyone.
Hi Bai Asha,
Thank you for your comments. Varicose veins do not have to get worse over time. I was hoping I may have mentioned something in my article to prove this. I did not know how bad they could get until I did the research for this article. All I want to do through my posts is to inform my readers there is always hope.
Best wishes,
Michael
Now I know after reading your article that Varicose veins are twisted, enlarged veins. Any superficial vein may become varicosed, but the veins most commonly affected are those in your legs. Spider veins are similar to varicose veins, but they’re smaller. Spider veins are found closer to the skin’s surface and are often red or blue. We should see our doctor if develop any of these symptoms. Thanks for giving your light on such a useful topic.
Hi Parveen,
Thank you for the comments. Until I researched varicose veins, I never realized how severe and painful this condition could cause the person who is afflicted by this condition. Also the progression, I saw some nasty cases but did not want to share the pictures.
Best wishes,
Michael
Very informative! You are sharing such a great info about varicose veins and some effective treatments to reduce their appearance. I like this article so much. Thanks and keep sharing.
Hi Harvey,
Thank you for your comments. Much appreciated.
Best wishes,
Michael
Excellent blog on the varicose veins. Thank you so much for sharing this blog post.
Thank you, appreciate you commenting.
Best wishes,
Michael