Global Health Threats Facing Us
Blue indicates link

GLOBAL HEALTH 2019. Climate Change
The world is facing multiple health challenges. These range from outbreaks of vaccine-preventable diseases like measles and diphtheria, increasing reports of drug-resistant pathogens, growing rates of obesity, and physical inactivity to the health impacts of environmental pollution and climate change and multiple humanitarian crises.
To address these and other threats, 2019 sees the start of the World Health Organization’s new 5-year strategic plan – the 13th General Programme of Work. This plan focuses on a triple billion target: ensuring 1 billion more people benefit from access to universal health coverage, 1 billion more people are protected from health emergencies and 1 billion more people enjoy better health and well-being. Reaching this goal will require addressing the threats to health from a variety of angles.
Here are 10 of the many issues that will demand attention from WHO and health partners in 2019.
Nine out of ten people breathe polluted air every day. In 2019, air pollution is considered by the WHO as the greatest environmental risk to health. Microscopic pollutants in the air can penetrate respiratory and circulatory systems, damaging the lungs, heart, and brain, killing 7 million people prematurely every year from diseases such as cancer, stroke, heart and lung disease. Around 90% of these deaths are in low- and middle-income countries, with high volumes of emissions from industry, transport, and agriculture, as well as dirty cookstoves and fuels in homes.
The primary cause of air pollution (burning fossil fuels) is also a major contributor to climate change, which impacts people’s health in different ways. Between 2030 and 2050, climate change is expected to cause 250,000 additional deaths per year, from malnutrition, malaria, diarrhea, and heat stress.
In October 2018, WHO held its first-ever Global Conference on Air Pollution and Health in Geneva. Countries and organizations made more than 70 commitments to improve air quality. This year, the United Nations Climate Summit in September will aim to strengthen climate action and ambition worldwide. Even if all the commitments made by countries for the Paris Agreement are achieved, the world is still on a course to warm by more than 3°C this century.
Noncommunicable diseases:
Noncommunicable diseases, such as diabetes, cancer, and heart disease, are collectively responsible for over 70% of all deaths worldwide, or 41 million people. This includes 15 million people dying prematurely, aged between 30 and 69.
Over 85% of these premature deaths are in low- and middle-income countries. The rise of these diseases has been driven by five major risk factors: tobacco use, physical inactivity, the harmful use of alcohol, unhealthy diets, and air pollution. These risk factors also exacerbate mental health issues, that may originate from an early age: half of all mental illness begins by the age of 14, but most cases go undetected and untreated – suicide is the second leading cause of death among 15-19 year-olds.
Among many things, this year WHO will work with governments to help them meet the global target of reducing physical inactivity by 15% by 2030 – through such actions as implementing the ACTIVE policy toolkit to help get more people active every day.
Global influenza pandemic:
The world will face another influenza pandemic – the only thing we don’t know is when it will hit and how severe it will be. Global defenses are only as effective as the weakest link in any country’s health emergency preparedness and response system.
WHO is constantly monitoring the circulation of influenza viruses to detect potential pandemic strains: 153 institutions in 114 countries are involved in global surveillance and response.
Every year, the WHO recommends which strains should be included in the flu vaccine to protect people from seasonal flu. In the event that a new flu strain develops pandemic potential, WHO has set up a unique partnership with all the major players to ensure effective and equitable access to diagnostics, vaccines, and antivirals (treatments), especially in developing countries.
Fragile and vulnerable settings:
More than 1.6 billion people (22% of the global population) live in places where protracted crises (through a combination of challenges such as drought, famine, conflict, and population displacement) and weak health services leave them without access to basic care.
Fragile settings exist in almost all regions of the world, and these are where half of the key targets in the sustainable development goals, including on child and maternal health, remain unmet.
WHO will continue to work in these countries to strengthen health systems so that they are better prepared to detect and respond to outbreaks, as well as able to deliver high-quality health services, including immunization.
Antimicrobial resistance:
The development of antibiotics, antivirals, and antimalarials are some of modern medicine’s greatest successes. Now, time with these drugs is running out. Antimicrobial resistance – the ability of bacteria, parasites, viruses, and fungi to resist these medicines – threatens to send us back to a time when we were unable to easily treat infections such as pneumonia, tuberculosis, gonorrhea, and salmonellosis. The inability to prevent infections could seriously compromise surgery and procedures such as chemotherapy.
Resistance to tuberculosis drugs is a formidable obstacle to fighting a disease that causes around 10 million people to fall ill and 1.6 million to die every year. In 2017, around 600,000 cases of tuberculosis were resistant to rifampicin – the most effective first-line drug – and 82% of these people had multidrug-resistant tuberculosis.
Drug resistance is driven by the overuse of antimicrobials in people, but also in animals, especially those used for food production, as well as in the environment. WHO is working with these sectors to implement a global action plan to tackle antimicrobial resistance by increasing awareness and knowledge, reducing infection, and encouraging prudent use of antimicrobials.
Ebola and other high-threat pathogens:
In 2018, the Democratic Republic of the Congo saw two separate Ebola outbreaks, both of which spread to cities of more than 1 million people. One of the affected provinces is also in an active conflict zone.
This shows that the context in which an epidemic of a high-threat pathogen like Ebola erupts is critical – what happened in rural outbreaks in the past doesn’t always apply to densely populated urban areas or conflict-affected areas.
At a conference on Preparedness for Public Health Emergencies held last December, participants from the public health, animal health, transport, and tourism sectors focussed on the growing challenges of tackling outbreaks and health emergencies in urban areas. They called for WHO and partners to designate 2019 as a “Year of action on preparedness for health emergencies”.
WHO’s R&D Blueprint identifies diseases and pathogens that have the potential to cause a public health emergency but lack effective treatments and vaccines. This watchlist for priority research and development includes Ebola, several other hemorrhagic fevers, Zika, Nipah, Middle East respiratory syndrome coronavirus (MERS-CoV) and Severe Acute Respiratory Syndrome (SARS), and disease X, which represents the need to prepare for an unknown pathogen that could cause a serious epidemic.
Weak primary health care:
Primary health care is usually the first point of contact people have with their health care system, and ideally should provide comprehensive, affordable, community-based care throughout life.
Primary health care can meet the majority of a person’s health needs for the course of their life. Health systems with strong primary health care are needed to achieve universal health coverage.
Yet many countries do not have adequate primary health care facilities. This neglect may be a lack of resources in low- or middle-income countries, but possibly also a focus in the past few decades on single disease programs. In October 2018, WHO co-hosted a major global conference in Astana, Kazakhstan at which all countries committed to renew the commitment to primary health care made in the Alma-Ata declaration in 1978.
In 2019, WHO will work with partners to revitalize and strengthen primary health care in countries, and follow up on specific commitments made by in the Astana Declaration.
Vaccine hesitancy:
Vaccine hesitancy – the reluctance or refusal to vaccinate despite the availability of vaccines – threatens to reverse progress made in tackling vaccine-preventable diseases. Vaccination is one of the most cost-effective ways of avoiding disease – it currently prevents 2-3 million deaths a year, and a further 1.5 million could be avoided if global coverage of vaccinations improved.
Measles, for example, has seen a 30% increase in cases globally. The reasons for this rise are complex, and not all of these cases are due to vaccine hesitancy. However, some countries that were close to eliminating the disease have seen a resurgence.
The reasons why people choose not to vaccinate are complex; a vaccine advisory group to WHO identified complacency, inconvenience in accessing vaccines, and lack of confidence are key reasons underlying hesitancy. Health workers, especially those in communities, remain the most trusted advisors and influencers of vaccination decisions, and they must be supported to provide trusted, credible information on vaccines.
In 2019, WHO will ramp up work to eliminate cervical cancer worldwide by increasing coverage of the HPV vaccine, among other interventions. 2019 may also be the year when transmission of wild poliovirus is stopped in Afghanistan and Pakistan. Last year, less than 30 cases were reported in both countries. WHO and its partners are committed to supporting these countries to vaccinate every last child to eradicate this crippling disease for good.
Dengue:
Dengue, a mosquito-borne disease that causes flu-like symptoms and can be lethal and kill up to 20% of those with severe dengue, has been a growing threat for decades.
A high number of cases occur in the rainy seasons of countries such as Bangladesh and India. Now, its season in these countries is lengthening significantly (in 2018, Bangladesh saw the highest number of deaths in almost two decades), and the disease is spreading to less tropical and more temperate countries such as Nepal, which have not traditionally seen the disease.
An estimated 40% of the world is at risk of dengue fever, and there are around 390 million infections a year. WHO’s Dengue control strategy aims to reduce deaths by 50% by 2020.
HIV:
The progress made against HIV has been enormous in terms of getting people tested, providing them with antiretrovirals (22 million are on treatment), and providing access to preventive measures such as pre-exposure prophylaxis (PrEP, which is when people at risk of HIV take antiretrovirals to prevent infection).
However, the epidemic continues to rage with nearly a million people every year dying of HIV/AIDS. Since the beginning of the epidemic, more than 70 million people have acquired the infection, and about 35 million people have died. Today, around 37 million worldwide live with HIV. Reaching people like sex workers, people in prison, men who have sex with men, or transgender people is hugely challenging. Often these groups are excluded from health services. A group increasingly affected by HIV are young girls and women (aged 15–24), who are particularly at high risk and account for 1 in 4 HIV infections in sub-Saharan Africa despite being only 10% of the population.
This year, WHO will work with countries to support the introduction of self-testing so that more people living with HIV know their status and can receive treatment (or preventive measures in the case of a negative test result). One activity will be to act on new guidance announced In December 2018, by WHO and the International Labour Organization to support companies and organizations to offer HIV self-tests in the workplace.
The most prevalent health issues in the world today along with their symptoms, causes, and preventive measures.
Cancer:
Cancer remains one of the major health concerns of the 21st century. Its occurrence has been increasing with modernization and advancement perhaps due to environmental deterioration and increased exposure to chemicals and radiation.
While there’s no particular cause of cancer, various risk factors contribute to the genesis of particular kinds of cancer. Tobacco and smoking, obesity, alcoholism, too much sun exposure, and radiation are among the common risk factors, while genetics also plays a pivotal role in increased risk among siblings and relatives.
Various infections like the Hepatitis B virus and Human Papillomavirus are also among the progenitors of cancer. Prostate cancer and breast cancer are the most common cancers in males and females respectively.
While a number of anticancer drugs, chemotherapy, radiation therapy, and surgery are used in treating cancer, complete treatment is still far off for many neoplasms. Hence, early detection of cancer is crucial.
Regular screening for cancer, and lifestyle modifications like regular exercise, healthy diet, and quitting smoking, and tobacco are preventive measures.
Diabetes:
Diabetes is a chronic condition associated with abnormally high blood glucose levels: fasting blood sugar level greater than 110 mg/dl, random blood glucose level greater than 200 mg/dl.
Blood glucose level is maintained in the normal range of 70-110 mg/dl by insulin, a hormone secreted by β cells of the pancreas. Any abnormality that causes the damage of β cells, and thus little or no insulin, contributes to the pathogenesis of Type 1 diabetes commonly seen in children and youth. Type 2 diabetes, however, results when body cells become resistant to the action of insulin and it commonly affects older people.
Diabetes leads to many acute and chronic complications affecting almost all parts of the body-brain (stroke, cognitive impairment), eye (retinopathy, glaucoma), heart (heart attack, congestive heart failure), nerves (peripheral neuropathy), ear (hearing impairment), skin (increased risk of infections). It thus remains one of the most debilitating diseases.
Preventive measures include lifestyle modifications like regular exercise, the inclusion of fiber-rich whole grains, nuts, vegetables, and fruits in the diet, maintaining a normal weight, and regular checkups.
The treatment regimen for type 1 and type 2 diabetes differ in that type 1 diabetes treatment includes insulin while type 2 diabetes is cured by sulfonylureas (glibenclamide, glipizide), meglitinides (repaglinide), biguanides (metformin), thiazolidinediones (pioglitazone).
Heart diseases:
Heart diseases like myocardial infarction, angina, and heart failure have been associated with a high fatality rate, killing more people than all forms of cancer combined in the United States.
Smoking, a high-fat diet, lack of exercise, and a sedentary lifestyle are common causes, while other body conditions add fuel to the fire aggravating the disease. Atherosclerosis, diabetes, hypertension, and infections are common culprits.
Hence, preventive measures like putting an end to smoking, minimizing salt intake, regular physical exercise, consuming a diet low in fat, and having regular health checkups will do a lot in reducing your risk for heart disease.
Kidney disease:
Renal failure remains one of the main global medical concerns. Kidney disease is assessed by measurement of GFR, which is the ability of kidneys to filter blood. The normal value of GFR is 125ml/min and by definition decrease in GFR is kidney failure.
Causes of acute kidney injury include pre-renal causes like dehydration, blood loss, and shock; renal causes include infections of the kidney; obstruction to urine flow falls under post-renal causes.
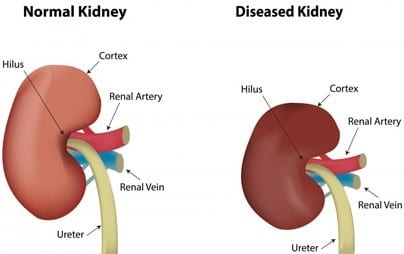
When kidneys don’t function for more than 3 months, it’s called chronic kidney disease, unlike acute kidney injury which is acute in onset. Symptoms include reduced urine volume, nausea, loss of appetite, muscle cramps, etc.
Guidelines for kidney disease prevention include reduced protein intake, salt restriction, adequate fluid intake, cessation of smoking, and maintaining normal body weight. Supplements like Forskolin really help in weight loss. Since kidney failure is mostly caused by diabetes and hypertension, treatment strategies include control of blood glucose level and blood pressure by necessary hypoglycemic and anti-hypertensive drugs. A kidney transplant is reserved for serious cases.
Alzheimer’s disease:
Alzheimer’s disease affects the cognitive function of the brain and is more common in females than in males. In males, another brain disease—Parkinson’s disease—is more common.
While the exact cause of Alzheimer’s disease remains unknown, it is widely known that advancing age and family history are common risk factors along with obesity, hypertension, and Down syndrome among others.
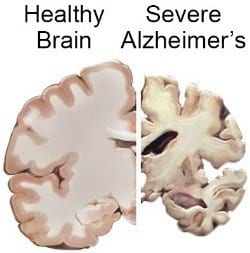
The pathophysiology involves the accumulation of senile plaques or beta-amyloid plaques and the formation of neurofibrillary tangles (NFTs) ultimately leading to loss of neurons and synapses necessary for cognitive functions of the body.
Treatment therapy includes only symptomatic therapies–cholinesterase inhibitors. Drugs are used according to symptoms, like antidepressants for depression and for agitation, sleep disorders, etc. Routine physical exercise will have an effect on disease progression as increased cardiorespiratory fitness has been shown to slow disease progression.
Influenza:
While a healthy person can fight influenza on his/her own, immunocompromised people, especially children, old, pregnant women, and people with conditions like diabetes and hypertension are at increased risk of developing potentially fatal pneumonia.
Increased incidence and death toll due to swine flu (H1N1 virus) led the WHO to declare the first flu pandemic in 41 years on June 11, 2009. It affected all continents except Antarctica in the 2009-2010 season and has been a regular problem since then, though luckily mortality rate has been similar to the usual flu.
With complications like pneumonia, influenza poses a serious threat, especially to the above-mentioned risk groups. Preemptive vaccination is the most effective way to prevent disease while regular washing of hands, preventing unnecessary touching of nose and mouth, and wearing masks are also to be followed.
Two antiviral agents, Zanamavir and Oseltamavir, are effective drugs to reduce the effects of swine flu, with newer drugs under study. There is evidence, however, of drug resistance due to excessive and indiscriminate use. Hence, necessary precautions and prevention are the most efficient way to save oneself from falling victim to the influenza virus.
Stroke:
A stroke or cerebrovascular accident is a condition potentially caused when blood supply to the brain is interrupted thus leading to the death of brain cells. It may be caused by ischemia– due to the blocked artery—or it can be hemorrhagic—due to the bursting of blood vessels.
Risk factors include obesity, physical inactivity, hypertension, and diabetes, while genetics also plays a role. Since it can lead to a number of complications like paralysis of the contralateral sides of the body, loss of cognitive function, emotional problems, and abnormal behaviors, and also due to the fact that treatment for any disease of the brain is complicated, one ought to have adequate knowledge about stroke, about its risk factors in general and everyone should develop a healthy lifestyle.
AIDS:
AIDS, having originated from chimpanzees, is already a global pandemic. About 37 million people are living with HIV AIDS with 17 million unaware of the fact they have the virus in their bodies. Sub-Saharan Africa is the most affected region with 25.8 million victims there, with a significant number of them being children due to mother-to-child transmission either during pregnancy, childbirth, or breastfeeding.
Transmitted through body fluids–blood, semen, breast milk, vaginal fluid, rectal fluids—it can be prevented if transmission of fluids can be avoided. Hence, safe blood transfusion, safe sex, limiting the number of sexual partners, and getting tested and treated for other STDs are effective preventive measures.
Antiretroviral therapy (ART) helps HIV-infected people to minimize virus load and stop the progression of disease thus, reducing the risk of transmission to other people as well. Antiretroviral therapy is provided to pregnant mothers to minimize the risk of transmission to the child while the newborn child should also receive the treatment for 6 weeks. As post-exposure prophylaxis (PEP), it is also used in cases possibly exposed to HIV as in breakage of the barrier during sex, exposure to the virus in health workers, etc.
Thank you for reading,
Michael
Comments are welcome.

Thank you so much for this post! It is really informative and it’s information that needs to get out there to the public. I worry about the effects of climate change mostly for my kids. This is something we can help prevent too and I hope we come together to work on a solution.
Hi Jessie,
Thank you for your comments.
Like you say we all need to come together and work on a solution. I think our planet is suffering because of the greed of big companies, and we have lost respect for mother nature.
Best wishes,
Michael
Great article, nice content, good read and informative.