What is Epilepsy?
Blue indicates link
Epilepsy is a central nervous system (neurological) disorder in which brain activity becomes abnormal, causing seizures or periods of unusual behavior, sensations, and sometimes loss of awareness.
Anyone can develop epilepsy. Epilepsy affects both males and females of all races, ethnic backgrounds, and ages.

Seizure symptoms can vary widely. Some people with epilepsy simply stare blankly for a few seconds during a seizure, while others repeatedly twitch their arms or legs. Having a single seizure doesn’t mean you have epilepsy. At least two unprovoked seizures are generally required for an epilepsy diagnosis.
Treatment with medications or sometimes surgery can control seizures for the majority of people with epilepsy. Some people require lifelong treatment to control seizures, but for others, the seizures eventually go away. Some children with epilepsy may outgrow the condition with age.
Epilepsy is a chronic disorder that causes unprovoked, recurrent seizures. A seizure is a sudden rush of electrical activity in the brain.
There are two main types of seizures. Generalized seizures affect the whole brain. Focal, or partial seizures, affect just one part of the brain.
A mild seizure may be difficult to recognize. It can last a few seconds during which you lack awareness.
Stronger seizures can cause spasms and uncontrollable muscle twitches and can last a few seconds to several minutes. During a stronger seizure, some people become confused or lose consciousness. Afterward, you may have no memory of it happening.
There are several reasons you might have a seizure.
These include:
- high fever
- head trauma
- Very low blood sugar
- alcohol withdrawal
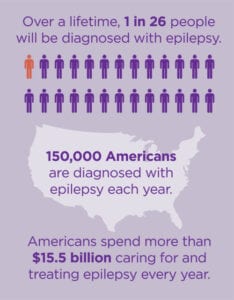
Epilepsy is a fairly common neurological disorder that affects 65 million people around the world. In the United States, it affects about 3 million people.
Anyone can develop epilepsy, but it’s more common in young children and older adults. It occurs slightly more in males than in females.
There’s no cure for epilepsy, but the disorder can be managed with medications and other strategies.
Types of Epilepsy Seizures
Seizures, abnormal movements, or behavior due to unusual electrical activity in the brain, are a symptom of epilepsy. However not all people who appear to have seizures have epilepsy, a group of related disorders characterized by a tendency for recurrent seizures.
Non-epileptic seizures (called pseudoseizures) are not accompanied by abnormal electrical activity in the brain and may be caused by psychological issues or stress. However, non-epileptic seizures look like true seizures, which makes diagnosis more difficult. Normal EEG readings and lack of response to epileptic drugs are two clues that are not true epileptic seizures. These types of seizures may be treated with psychotherapy and psychiatric medications.
Provoked seizures are single seizures that may occur as a result of trauma, low blood sugar (hypoglycemia), low blood sodium, high fever, or alcohol or drug abuse. Fever-related (or febrile) seizures may occur during infancy but are usually outgrown by age 6. After a careful evaluation to estimate the risk of recurrence, patients who suffer a single seizure may not need treatment.
Seizure disorder is a general term used to describe any condition in which seizures may be a symptom. Seizure disorder is a general term that is often used in place of the term ”epilepsy.”
Types of Epilepsy
Patients with epilepsy may experience more than one seizure type. This is because seizures are the only symptoms. Therefore, it is essential that your neurologist diagnose your type of epilepsy, not just the type(s) of seizure you are having.
All types of epilepsy have seizures as a symptom. These are surges of electricity in your brain. They’re like electrical storms that briefly stop your brain cells from working normally.
If you have a seizure caused by epilepsy, your doctor will follow three steps to give you the right diagnosis.
- Figure out the types of seizures you had
- Based on the type of seizure, figure out the type of epilepsy you have
- Decide whether you have a specific epilepsy syndrome as well
To come up with answers, your doctor will ask you questions and run tests, like an EEG (electroencephalogram) or MRI (magnetic resonance imaging) to check your brain waves. It is also helpful to bring someone who has witnessed the seizures or to have a video of the seizures in order to classify the seizure type.
Experts now divide epilepsy into four basic types based on the seizures you’re having:
- Generalized epilepsy
- Focal epilepsy
- Generalized and focal epilepsy
- Unknown if generalized or focal epilepsy
Generalized Epilepsy
If you have this type of epilepsy, seizures start on both sides of the brain (or quickly affect networks of brain cells on both sides). This type of epilepsy has two basic kinds of seizures:
Generalized motor seizures. These used to be called “grand mal” seizures. They cause your body to move in ways you can’t control, sometimes dramatically. Tonic-clonic seizures are one example. When it hits, you lose consciousness and your muscles stiffen and jerk. Other types you may hear your doctor talk about include clonic, tonic, and myoclonic.
Generalized non-motor (or absence) seizures. They used to be called “petit mal” seizures. Some specific types you may hear your doctor mention are typical, atypical, and myoclonic.
During this type of seizure, you may stop what you’re doing and stare into space. You may also do the same movements over and over, like smacking your lips. These types of seizures are generally called “absence” seizures because it’s like the person isn’t really there.
Focal Epilepsy
In this type of epilepsy, seizures develop in a particular area (or network of brain cells) on one side of the brain. These used to be called “partial seizures.”
Focal epilepsy seizures come in four categories:
Focal-aware seizures. If you know what’s happening during the seizure, it’s an “aware” seizure. These used to be called “simple partial seizures.”
Focal impaired awareness seizures. If you’re confused or don’t know what’s happening during your seizure — or don’t remember if — it’s an impaired awareness seizure. These used to be called “complex partial seizures.”
Focal motor seizures. In this type of seizure, you’ll move to some extent — anything from twitching to spasms, to rubbing hands, to walking around. Some types that you may hear your doctor talk about are atonic, clonic, epileptic spasms, myoclonic, and tonic.
Focal non-motor seizures. This type of seizure doesn’t lead to twitches or other movements. Instead, it causes changes in how you feel or think. You might have intense emotions, strange feelings, or symptoms like a racing heart, goosebumps, or waves of heat or cold.
Generalized and Focal Epilepsy
Just as the name suggests, this is a type of epilepsy where people have both generalized and focal seizures.
Unknown if Generalized or Focal Epilepsy
Sometimes, doctors are sure that a person has epilepsy, but they don’t know whether the seizures are focal or generalized. This can happen if you were alone when you had seizures, so no one can describe what happened. Your doctor may also classify your epilepsy type as “unknown if generalized or focal epilepsy” if your test results aren’t clear.
Epilepsy Syndromes
In addition to a type of epilepsy, you could also have an epilepsy syndrome. These are more specific than the type. Doctors diagnose syndromes based on a bunch of symptoms or signs that tend to go together as well as the results of testing (MRI and EEG), which helps to classify the syndrome.
Some of these features include the age you started getting seizures, the type of seizures you have, your triggers, the time of day seizures happen, and more.
There are dozens of epilepsy seizure syndromes. Some include West syndrome, Doose syndrome, Rasmussen’s syndrome, and Lennox-Gastaut syndrome.
Symptoms
Because epilepsy is caused by abnormal activity in the brain, seizures can affect any process your brain coordinates. Seizure signs and symptoms may include:
- Temporary confusion
- A staring spell
- Uncontrollable jerking movements of the arms and legs
- Loss of consciousness or awareness
- Psychic symptoms such as fear, anxiety, or deja vu
Symptoms vary depending on the type of seizure. In most cases, a person with epilepsy will tend to have the same type of seizure each time, so the symptoms will be similar from episode to episode.
Doctors generally classify seizures as either focal or generalized, based on how the abnormal brain activity begins.
Causes
Epilepsy has no identifiable cause in about half the people with the condition. In the other half, the condition may be traced to various factors, including:
- Genetic influence. Some types of epilepsy, which are categorized by the type of seizure you experience or the part of the brain that is affected, run in families. In these cases, it’s likely that there’s a genetic influence. Researchers have linked some types of epilepsy to specific genes, but for most people, genes are only part of the cause of epilepsy. Certain genes may make a person more sensitive to environmental conditions that trigger seizures.
- Head trauma. Head trauma as a result of a car accident or other traumatic injury can cause epilepsy.
- Brain conditions. Brain conditions that cause damage to the brain, such as brain tumors or strokes, can cause epilepsy. Stroke is a leading cause of epilepsy in adults older than age 35.
- Infectious diseases. Infectious diseases, such as meningitis, AIDS, and viral encephalitis, can cause epilepsy.
- Prenatal injury. Before birth, babies are sensitive to brain damage that could be caused by several factors, such as an infection in the mother, poor nutrition, or oxygen deficiencies. This brain damage can result in epilepsy or cerebral palsy.
- Developmental disorders. Epilepsy can sometimes be associated with developmental disorders, such as autism and neurofibromatosis.
Risk factors
Certain factors may increase your risk of epilepsy:
- Age. The onset of epilepsy is most common in children and older adults, but the condition can occur at any age.
- Family history. If you have a family history of epilepsy, you may be at an increased risk of developing a seizure disorder.
- Head injuries. Head injuries are responsible for some cases of epilepsy. You can reduce your risk by wearing a seat belt while riding in a car and by wearing a helmet while bicycling, skiing, riding a motorcycle, or engaging in other activities with a high risk of head injury.
- Stroke and other vascular diseases. Stroke and other blood vessel (vascular) diseases can lead to brain damage that may trigger epilepsy. You can take a number of steps to reduce your risk of these diseases, including limiting your intake of alcohol and avoiding cigarettes, eating a healthy diet, and exercising regularly.
- Dementia. Dementia can increase the risk of epilepsy in older adults.
- Brain infections. Infections such as meningitis, which causes inflammation in your brain or spinal cord, can increase your risk.
- Seizures in childhood. High fevers in childhood can sometimes be associated with seizures. Children who have seizures due to high fevers generally won’t develop epilepsy. The risk of epilepsy increases if a child has a long seizure, another nervous system condition, or a family history of epilepsy.
Complications
Having a seizure at certain times can lead to circumstances that are dangerous to yourself or others.
- Falling. If you fall during a seizure, you can injure your head or break a bone.
- Drowning. If you have epilepsy, you’re 15 to 19 times more likely to drown while swimming or bathing than the rest of the population because of the possibility of having a seizure while in the water.
- Car accidents. A seizure that causes either loss of awareness or control can be dangerous if you’re driving a car or operating other equipment. Many states have driver’s license restrictions related to a driver’s ability to control seizures and impose a minimum amount of time that a driver is seizure-free, ranging from months to years, before being allowed to drive.
- Pregnancy complications. Seizures during pregnancy pose dangers to both mother and baby and certain anti-epileptic medications increase the risk of birth defects. If you have epilepsy and you’re considering becoming pregnant, talk to your doctor as you plan your pregnancy. Most women with epilepsy can become pregnant and have healthy babies. You’ll need to be carefully monitored throughout pregnancy, and medications may need to be adjusted. It’s very important that you work with your doctor to plan your pregnancy.
- Emotional health issues. People with epilepsy are more likely to have psychological problems, especially depression, anxiety, and suicidal thoughts and behaviors. Problems may be a result of difficulties dealing with the condition itself as well as medication side effects.
Other life-threatening complications of epilepsy are uncommon but may happen, such as:
- Status epilepticus. This condition occurs if you’re in a state of continuous seizure activity lasting more than five minutes or if you have frequent recurrent seizures without regaining full consciousness in between them. People with status epilepticus have an increased risk of permanent brain damage and death.
- Sudden unexpected death in epilepsy (SUDEP). People with epilepsy also have a small risk of sudden unexpected death. The cause is unknown, but some research shows it may occur due to heart or respiratory conditions. People with frequent tonic-clonic seizures or people whose seizures aren’t controlled by medications may be at higher risk of SUDEP. Overall, about 1 percent of people with epilepsy die of SUDEP.
Diagnosis
To diagnose your condition, your doctor will review your symptoms and medical history. Your doctor may order several tests to diagnose epilepsy and determine the cause of seizures. Your evaluation may include:
- A neurological exam. Your doctor may test your behavior, motor abilities, mental function, and other areas to diagnose your condition and determine the type of epilepsy you may have.
- Blood tests. Your doctor may take a blood sample to check for signs of infections, genetic conditions, or other conditions that may be associated with seizures.
Your doctor may also suggest tests to detect brain abnormalities, such as:
- Electroencephalogram (EEG). This is the most common test used to diagnose epilepsy. In this test, electrodes are attached to your scalp with a paste-like substance or cap. The electrodes record the electrical activity of your brain. If you have epilepsy, it’s common to have changes in your normal pattern of brain waves, even when you’re not having a seizure. Your doctor may monitor you on video when conducting an EEG while you’re awake or asleep, to record any seizures you experience. Recording the seizures may help the doctor determine what kind of seizures you’re having or rule out other conditions. The test may be done in a doctor’s office or the hospital. If appropriate, you also may have an ambulatory EEG, which you wear at home while the EEG records seizure activity over the course of a few days. Your doctor may give you instructions to do something that will cause seizures, such as getting little sleep prior to the test.
- High-density EEG. In a variation of an EEG test, your doctor may recommend high-density EEG, which spaces electrodes more closely than conventional EEG — about half a centimeter apart. High-density EEG may help your doctor more precisely determine which areas of your brain are affected by seizures.
- Computerized tomography (CT) scan. A CT scan uses X-rays to obtain cross-sectional images of your brain. CT scans can reveal abnormalities in your brain that might be causing your seizures, such as tumors, bleeding, and cysts.
- Magnetic resonance imaging (MRI). An MRI uses powerful magnets and radio waves to create a detailed view of your brain. Your doctor may be able to detect lesions or abnormalities in your brain that could be causing your seizures.
- Functional MRI (fMRI). A functional MRI measures the changes in blood flow that occur when specific parts of your brain are working. Doctors may use an fMRI before surgery to identify the exact locations of critical functions, such as speech and movement so that surgeons can avoid injuring those places while operating.
- Positron emission tomography (PET). PET scans use a small amount of low-dose radioactive material that’s injected into a vein to help visualize active areas of the brain and detect abnormalities.
- Single-photon emission computerized tomography (SPECT). This type of test is used primarily if you’ve had an MRI and EEG that didn’t pinpoint the location in your brain where the seizures are originating. A SPECT test uses a small amount of low-dose radioactive material that’s injected into a vein to create a detailed, 3-D map of the blood flow activity in your brain during seizures. Doctors also may conduct a form of a SPECT test called subtraction ictal SPECT compared to MRI (SISCOM), which may provide even more detailed results.
- Neuropsychological tests. In these tests, doctors assess your thinking, memory, and speech skills. The test results help doctors determine which areas of your brain are affected.
Along with your test results, your doctor may use a combination of analysis techniques to help pinpoint where in the brain seizures start:
- Statistical parametric mapping (SPM). SPM is a method of comparing areas of the brain that have increased metabolism during seizures to normal brains, which can give doctors an idea of where seizures begin.
- Curry analysis. Curry analysis is a technique that takes EEG data and projects it onto an MRI of the brain to show doctors where seizures are occurring.
- Magnetoencephalography (MEG). MEG measures the magnetic fields produced by brain activity to identify potential areas of seizure onset.
An accurate diagnosis of your seizure type and where seizures begin gives you the best chance of finding an effective treatment.
Treatment
Doctors generally begin by treating epilepsy with medication. If medications don’t treat the condition, doctors may propose surgery or another type of treatment.
Medication
Most people with epilepsy can become seizure-free by taking one anti-seizure medication, which is also called anti-epileptic medication. Others may be able to decrease the frequency and intensity of their seizures by taking a combination of medications.
Many children with epilepsy who aren’t experiencing epilepsy symptoms can eventually discontinue medications and live a seizure-free life. Many adults can discontinue medications after two or more years without seizures. Your doctor will advise you about the appropriate time to stop taking medications.
Finding the right medication and dosage can be complex. Your doctor will consider your condition, frequency of seizures, age, and other factors when choosing which medication to prescribe. Your doctor will also review any other medications you may be taking, to ensure the anti-epileptic medications won’t interact with them.
Your doctor likely will first prescribe a single medication at a relatively low dosage and may increase the dosage gradually until your seizures are well-controlled.
Anti-seizure medications may have some side effects. Mild side effects include:
- Fatigue
- Dizziness
- Weight gain
- Loss of bone density
- Skin rashes
- Loss of coordination
- Speech problems
- Memory and thinking problems
More severe but rare side effects include:
- Depression
- Suicidal thoughts and behaviors
- Severe rash
- Inflammation of certain organs, such as your liver
To achieve the best seizure control possible with medication, follow these steps:
- Take medications exactly as prescribed.
- Always call your doctor before switching to a generic version of your medication or taking other prescription medications, over-the-counter drugs, or herbal remedies.
- Never stop taking your medication without talking to your doctor.
- Notify your doctor immediately if you notice new or increased feelings of depression, suicidal thoughts, or unusual changes in your mood or behaviors.
- Tell your doctor if you have migraines. Doctors may prescribe one of the anti-epileptic medications that can prevent migraines and treat epilepsy.
At least half the people newly diagnosed with epilepsy will become seizure-free with their first medication. If anti-epileptic medications don’t provide satisfactory results, your doctor may suggest surgery or other therapies. You’ll have regular follow-up appointments with your doctor to evaluate your condition and medications.
Surgery
Epilepsy surgery
When medications fail to provide adequate control over seizures, surgery may be an option. With epilepsy surgery, a surgeon removes the area of your brain that’s causing seizures.
Doctors usually perform surgery when tests show that:
- Your seizures originate in a small, well-defined area of your brain
- The area in your brain to be operated on doesn’t interfere with vital functions such as speech, language, motor function, vision, or hearing
Although many people continue to need some medication to help prevent seizures after successful surgery, you may be able to take fewer drugs and reduce your dosages.
In a small number of cases, surgery for epilepsy can cause complications such as permanently altering your thinking (cognitive) abilities. Talk to your surgeon about his or her experience, success rates, and complication rates with the procedure you’re considering.
Therapies
Apart from medications and surgery, these potential therapies offer an alternative for treating epilepsy:
- Vagus nerve stimulation. In vagus nerve stimulation, doctors implant a device called a vagus nerve stimulator underneath the skin of your chest, similar to a heart pacemaker. Wires from the stimulator are connected to the vagus nerve in your neck. The battery-powered device sends bursts of electrical energy through the vagus nerve and to your brain. It’s not clear how this inhibits seizures, but the device can usually reduce seizures by 20 to 40 percent. Most people still need to take anti-epileptic medication, although some people may be able to lower their medication dose. You may experience side effects from vagus nerve stimulation, such as throat pain, hoarse voice, shortness of breath, or coughing.
- Ketogenic diet. Some children with epilepsy have been able to reduce their seizures by following a strict diet that’s high in fats and low in carbohydrates. In this diet, called a ketogenic diet, the body breaks down fats instead of carbohydrates for energy. After a few years, some children may be able to stop the ketogenic diet — under the close supervision of their doctors — and remain seizure-free. Consult a doctor if you or your child is considering a ketogenic diet. It’s important to make sure that your child doesn’t become malnourished when following the diet. Side effects of a ketogenic diet may include dehydration, constipation, slowed growth because of nutritional deficiencies, and a buildup of uric acid in the blood, which can cause kidney stones. These side effects are uncommon if the diet is properly and medically supervised. Following a ketogenic diet can be a challenge. Low-glycemic index and modified Atkins diets offer less restrictive alternatives that may still provide some benefit for seizure control.
- Deep brain stimulation. In deep brain stimulation, surgeons implant electrodes into a specific part of your brain, typically your thalamus. The electrodes are connected to a generator implanted in your chest or your skull that sends electrical pulses to your brain and may reduce your seizures.
Lifestyle and home remedies
Understanding your condition can help you take better control of it:
- Take your medication correctly. Don’t adjust your dosage before talking to your doctor. If you feel your medication should be changed, discuss it with your doctor.
- Get enough sleep. Lack of sleep can trigger seizures. Be sure to get adequate rest every night.
- Wear a medical alert bracelet. This will help emergency personnel know how to treat you correctly.
- Exercise. Exercising may help keep you physically healthy and reduce depression. Make sure to drink enough water, and rest if you get tired during exercise.
In addition, make healthy life choices, such as managing stress, limiting alcoholic beverages, and avoiding cigarettes.
Herbal Natural Treatments
1. Epsom Salt
Studies show that Epsom salt is effective in reducing seizures in people with epilepsy. The magnesium sulfate in Epsom salt changes physiochemical cell relationships in the brain, which in turn lessens the frequency of seizures and convulsions.
- Crush pure-grade Epsom salt into a very fine powder. Add ½ teaspoon of the powder to a glass of orange juice or water and drink it each morning.
- You can also enjoy relaxing and soothing Epsom salt baths 2 or 3 times a week.
2. Limes
A popular Ayurvedic remedy for epilepsy is limes. Limes help improve blood circulation to the brain. Moreover, they help normalize excessive calcium that may hamper brain functionality.
- Mix 2 tablespoons of fresh lime juice and ½ teaspoon of baking soda in a glass of water. Drink it daily before going to bed.
- You can also apply fresh lime juice to your head and massage thoroughly for a few minutes. Do this daily before taking a shower.
3. Garlic
Garlic is also useful in treating epilepsy. Its antioxidant, antispasmodic, and anti-inflammatory properties help destroy harmful free radicals in the body and promote proper functioning of the nervous system. This in turn prevents seizures and other epilepsy-related symptoms.
- Mix together ½ cup each of milk and water. Heat it to a boil. Add 4 to 5 crushed garlic cloves and boil until the mixture is reduced by half. Strain and drink it once daily.
- Alternatively, take garlic supplements daily. Consult your doctor for the correct dosage.
4. Passionflower
The herb passionflower also helps reduce seizures. It contains a chemical known as chrysin, which helps increase the amount of gamma-aminobutyric acid (GABA) in the brain. This, in turn, reduces the frequency of seizures as well as anxiety.
- Drink 1 to 2 cups of herbal tea prepared with passionflower. Steep 1 teaspoon of dried passionflower in a cup of boiling water for 10 minutes, then strain it.
- Passionflower is also available in capsule, tablet, liquid extract, and tincture forms. Always take this herb under the guidance of a doctor.
Note: Avoid passionflower if you are pregnant or breastfeeding. Also, consult your doctor before taking this herb as it may increase the effects of anti-seizure medications.
5. Winter Melon
According to Ayurveda, winter melon, also known as ash gourd, is an effective home remedy for epilepsy due to its nutritional and medicinal properties. This vegetable helps keep the nervous system healthy and ensures the smooth functioning of the brain cells.
- Drink ½ glass of winter melon juice daily in the morning on an empty stomach. To enhance the taste, you can add a little sugar.
- Another option is to extract the juice of a bowl of crushed winter melon. Add 1 to 2 teaspoons of licorice powder to it and mix well. Drink this solution once daily.
6. Exercise
Regular physical exercise improves fitness, energy, and mood, which in turn helps reduce seizures and the impact of epilepsy on one’s life. Moreover, exercise releases feel-good hormones into the brain and increases oxygen flow to the brain.
- Do a warm-up and stretching exercises daily to feel more relaxed.
- Walking is one of the easiest and safest exercises that people with epilepsy should do. Walk for 45 minutes, at least 4 times a week.
- Swimming and other water sports can be great exercise.
- Gardening and other relaxing activities like tai chi are also great exercises.
Note: Drink water before and after exercise to prevent dehydration. In addition, stop and rest if you are feeling tired.
7. Yoga
Yoga is an age-old practice that alleviates stress, induces relaxation, and provides multiple health benefits for people with epilepsy. The combination of controlled deep breathing, physical postures, and meditation helps control seizures and reduce other epilepsy symptoms. The top yoga poses for epilepsy are:
- Balasana (Child’s Pose)
- Nadi Shodhana (Alternate Nostril Breathing)
- Kapotasana (Pigeon Pose)
- Sirsasana (Headstand)
- Camatkarasana (Wild Thing)
As it is very important to do yoga poses in the correct manner to reap the benefits, learn them from an expert only.
8. Take Necessary Vitamins
A healthy diet is essential in the treatment of epilepsy. There are different vitamins that can help a lot. For instance, vitamin E helps control neurons that cause seizures and anxiety disorders.
As epilepsy can occur due to vitamin B1 deficiency, eat foods high in vitamin B1, or take a supplement after consulting a doctor.
Other vitamins that can help treat epilepsy are vitamins B12, B6, and D.
Always consult a doctor before taking a supplement.
9. Acupuncture
In traditional Chinese medicine, acupuncture is a well-known treatment for seizures due to epilepsy. In acupuncture, the pressure is applied to specific points on the body using fine needles.
Although its mechanism is not known, acupuncture can help alter brain activity to reduce seizures by restoring the flow of qi (energy) throughout the body.
To enjoy the benefits of acupuncture, get it done by an expert only.
Additional Tips
- Get enough sleep as sleep deprivation can trigger seizures.
- If you have seizures regularly, wear a medical alert bracelet. This will help people know about your condition.
- Manage stress and avoid stressful situations.
- Drink ½ glass of grape juice daily.
- Limit your intake of alcohol and avoid smoking.
- As low calcium and magnesium can trigger seizures, eat foods high in these nutrients.
- Keep a written record of any seizures you have and keep your doctor updated.
- Avoid all “white” products, including white sugar, white flour, table salt, and white rice.
- Do not consume artificial sweeteners or additives.
- Do not skip meals, especially breakfast.
- Follow the ketogenic diet, even though the restrictions can be challenging.
Lastly, take the medicines prescribed by your doctor in incorrect dosages in a timely manner. Do not stop taking your medicines without your doctor’s approval.
Always consult with your doctor before taking any herbal remedies.
Thank you for reading
Michael
Comments are welcome
Thank you very much for this extremely informative article about Epilepsy and the different types of seizures that are associated with it. The additional tip sram so helpful to people that may never have considered them to be a problem.
Areas that may be triggers such as artificial sweeteners, white flour, table salt and white rice are thing that we normally wouldn’t consider to trigger a seizure
are extremely important for those at risk to understand.
Very well presented Thank you again
Richard
Hi Richard,
Thank you for your comments. Knowing what the trigger mechanisms are, I do believe can help a person suffering from epilepsy
from suffering a seizure.
Best wishes,
Michael
hello there! Thank you very much for this well detailed and informative article on epilepsy. I’ve seen someone have seizure before but I used to think epilepsy was contagious, i had no idea. Now I feel bad for avoiding the person like a plague. Thanks for enlightening me on this and also for explaining the different kinds of seizure. I am well informed now and I appreciate you for opening my eyes
Hi Sophie,
Thank you for commenting. I am glad you found my article informative. It is hard to know what to do if someone goes into an epileptic seizure. In fact, it is kind of scary.
Best wishes,
Michael