What is Bipolar Disorder?
Blue indicates link
Bipolar disorder, formerly called manic depression, is a mental health condition that causes extreme mood swings that include emotional highs (mania or hypomania) and lows (depression).

When you become depressed, you may feel sad or hopeless and lose interest or pleasure in most activities. When your mood shifts to mania or hypomania (less extreme than mania), you may feel euphoric, full of energy, or unusually irritable. These mood swings can affect sleep, energy, activity, judgment, behavior, and the ability to think clearly.
Episodes of mood swings may rarely occur or multiple times a year. While most people will experience some emotional symptoms between episodes, some may not experience any.
Although bipolar disorder is a lifelong condition, you can manage your mood swings and other symptoms by following a treatment plan. In most cases, bipolar disorder is treated with medications and psychological counseling (psychotherapy).
Symptoms:
There are several types of bipolar and related disorders. They may include mania hypomania and depression. Symptoms can cause unpredictable changes in mood and behavior, resulting in significant distress and difficulty in life.
- Bipolar I disorder. You’ve had at least one manic episode that may be preceded or followed by hypomanic or major depressive episodes. In some cases, mania may trigger a break from reality (psychosis).
- Bipolar II disorder. You’ve had at least one major depressive episode and at least one hypomanic episode, but you’ve never had a manic episode.
- Cyclothymic disorder. You’ve had at least two years — or one year in children and teenagers — of many periods of hypomania symptoms and periods of depressive symptoms (though less severe than major depression).
- Other types. These include, for example, bipolar and related disorders induced by certain drugs or alcohol or due to a medical condition, such as Cushing’s disease, multiple sclerosis, or stroke.
Bipolar II disorder is not a milder form of bipolar I disorder, but a separate diagnosis. While the manic episodes of bipolar I disorder can be severe and dangerous, individuals with bipolar II disorder can be depressed for longer periods, which can cause significant impairment.
Although bipolar disorder can occur at any age, typically it’s diagnosed in the teenage years or early 20s. Symptoms can vary from person to person, and symptoms may vary over time.
Mania and hypomania:
Mania and hypomania are two distinct types of episodes, but they have the same symptoms. Mania is more severe than hypomania and causes more noticeable problems at work, school, and social activities, as well as relationship difficulties. Mania may also trigger a break from reality (psychosis) and require hospitalization.
Both a manic and a hypomanic episode include three or more of these symptoms:
- Abnormally upbeat, jumpy, or wired
- Increased activity, energy, or agitation
- An exaggerated sense of well-being and self-confidence (euphoria)
- Decreased need for sleep
- Unusual talkativeness
- Racing thoughts
- Distractibility
- Poor decision-making — for example, going on buying sprees, taking sexual risks, or making foolish investments
Major depressive episode:
A major depressive episode includes symptoms that are severe enough to cause noticeable difficulty in day-to-day activities, such as work, school, social activities, or relationships. An episode includes five or more of these symptoms:
- Depressed mood, such as feeling sad, empty, hopeless, or tearful (in children and teens, depressed mood can appear as irritability)
- Marked loss of interest or feeling no pleasure in all — or almost all — activities
- Significant weight loss when not dieting, weight gain, or decrease or increase in appetite (in children, failure to gain weight, as expected, can be a sign of depression)
- Either insomnia or sleeping too much
- Either restlessness or slowed behavior
- Fatigue or loss of energy
- Feelings of worthlessness or excessive or inappropriate guilt
- Decreased ability to think or concentrate, or indecisiveness
- Thinking about, planning, or attempting suicide
Other features of bipolar disorder:
Signs and symptoms of bipolar I and bipolar II disorders may include other features, such as anxious distress, melancholy, psychosis, or others. The timing of symptoms may include diagnostic labels such as mixed or rapid cycling. In addition, bipolar symptoms may occur during pregnancy or change with the seasons.
Symptoms in children and teens:
Symptoms of bipolar disorder can be difficult to identify in children and teens. It’s often hard to tell whether these are normal ups and downs, the results of stress or trauma, or signs of a mental health problem other than bipolar disorder.
Children and teens may have distinct major depressive manic or hypomanic episodes, but the pattern can vary from that of adults with bipolar disorder. And moods can rapidly shift during episodes. Some children may have periods without mood symptoms between episodes.
The most prominent signs of bipolar disorder in children and teenagers may include severe mood swings that are different from their usual mood swings.
When to see a doctor:
Despite the mood extremes, people with bipolar disorder often don’t recognize how much their emotional instability disrupts their lives and the lives of their loved ones and don’t get the treatment they need.
And if you’re like some people with bipolar disorder, you may enjoy the feelings of euphoria and cycles of being more productive. However, this euphoria is always followed by an emotional crash that can leave you depressed, worn out — and perhaps in financial, legal, or relationship trouble.
If you have any symptoms of depression or mania, see your doctor or mental health professional. Bipolar disorder doesn’t get better on its own. Getting treatment from a mental health professional with experience in bipolar disorder can help you get your symptoms under control.
When to get emergency help:
Suicidal thoughts and behavior are common among people with bipolar disorder. If you have thoughts of hurting yourself, call 911 or your local emergency number immediately, go to an emergency room, or confide in a trusted relative or friend. Please keep these numbers handy. You could feel good at one moment and something could trigger a suicidal thought.
If you have a loved one who is in danger of suicide or has made a suicide attempt, make sure someone stays with that person. Call 911 or your local emergency number immediately. Or, if you think you can do so safely, take the person to the nearest hospital emergency room.
Causes:
The exact cause of bipolar disorder is unknown, but several factors may be involved, such as:
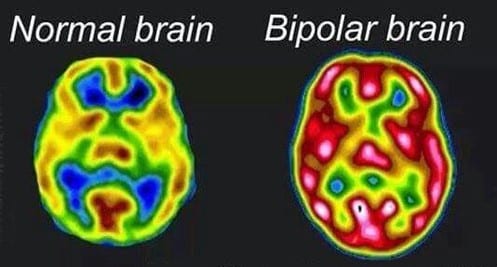
- Biological differences. People with bipolar disorder appear to have physical changes in their brains. The significance of these changes is still uncertain but may eventually help pinpoint causes.
- Genetics. Bipolar disorder is more common in people who have a first-degree relative, such as a sibling or parent, with the condition. Researchers are trying to find genes that may be involved in causing bipolar disorder.
Risk factors:
Factors that may increase the risk of developing bipolar disorder or act as a trigger for the first episode include:
- Having a first-degree relative, such as a parent or sibling, with bipolar disorder
- Periods of high stress, such as the death of a loved one or other traumatic event
- Drug or alcohol abuse
Complications:
Left untreated, bipolar disorder can result in serious problems that affect every area of your life, such as:
- Problems related to drug and alcohol use
- Suicide or suicide attempts
- Legal or financial problems
- Damaged relationships
- Poor work or school performance
Co-occurring conditions:
If you have bipolar disorder, you may also have another health condition that needs to be treated along with the bipolar disorder. Some conditions can worsen bipolar disorder symptoms or make treatment less successful. Examples include:
- Anxiety disorders
- Eating disorders
- Attention-deficit/hyperactivity disorder (ADHD)
- Alcohol or drug problems
- Physical health problems, such as heart disease, thyroid problems, headaches, or obesity
Prevention:
There’s no sure way to prevent bipolar disorder. However, getting treatment at the earliest signs of a mental health disorder can help prevent bipolar disorder or other mental health conditions from worsening.
If you’ve been diagnosed with bipolar disorder, some strategies can help prevent minor symptoms from becoming full-blown episodes of mania or depression:
- Pay attention to warning signs. Addressing symptoms early on can prevent episodes from getting worse. You may have identified a pattern to your bipolar episodes and what triggers them. Call your doctor if you feel you’re falling into an episode of depression or mania. Involve family members or friends in watching for warning signs.
- Avoid drugs and alcohol. Using alcohol or recreational drugs can worsen your symptoms and make them more likely to come back.
- Take your medications exactly as directed. You may be tempted to stop treatment — but don’t. Stopping your medication or reducing your dose on your own may cause withdrawal effects or your symptoms may worsen or return.
Diagnosis:
To determine if you have bipolar disorder, your evaluation may include:
- Physical exam. Your doctor may do a physical exam and lab tests to identify any medical problems that could be causing your symptoms.
- Psychiatric assessment. Your doctor may refer you to a psychiatrist, who will talk to you about your thoughts, feelings, and behavior patterns. You may also fill out a psychological self-assessment or questionnaire. With your permission, family members or close friends may be asked to provide information about your symptoms.
- Mood charting. You may be asked to keep a daily record of your moods, sleep patterns, or other factors that could help with diagnosis and finding the right treatment.
- Criteria for bipolar disorder. Your psychiatrist may compare your symptoms with the criteria for bipolar and related disorders in the Diagnostic and Statistical Manual of Mental Disorders (DSM-5), published by the American Psychiatric Association.
Diagnosis in children:
Although the diagnosis of children and teenagers with bipolar disorder includes the same criteria that are used for adults, symptoms in children and teens often have different patterns and may not fit neatly into the diagnostic categories.
Also, children who have bipolar disorder are frequently diagnosed with other mental health conditions such as attention-deficit/hyperactivity disorder (ADHD) or behavior problems, which can make diagnosis more complicated. Referral to a child psychiatrist with experience in bipolar disorder is recommended.
Bipolar Disorder Video Things We Might Not Tell You
Treatment:
Treatment is best guided by a medical doctor who specializes in diagnosing and treating mental health conditions (psychiatrist) who is skilled in treating bipolar and related disorders. You may have a treatment team that also includes a psychologist, a social worker, and a psychiatric nurse.
Bipolar disorder is a lifelong condition. Treatment is directed at managing symptoms. Depending on your needs, treatment may include:
- Medications. Often, you’ll need to start taking medications to balance your moods right away.
- Continued treatment. Bipolar disorder requires lifelong treatment with medications, even during periods when you feel better. People who skip maintenance treatment are at high risk of a relapse of symptoms or having minor mood changes turn into full-blown mania or depression.
- Day treatment programs. Your doctor may recommend a day treatment program. These programs provide the support and counseling you need while you get symptoms under control.
- Substance abuse treatment. If you have problems with alcohol or drugs, you’ll also need substance abuse treatment. Otherwise, it can be very difficult to manage bipolar disorder.
- Hospitalization. Your doctor may recommend hospitalization if you’re behaving dangerously, you feel suicidal or you become detached from reality (psychotic). Getting psychiatric treatment at a hospital can help keep you calm and safe and stabilize your mood, whether you’re having a manic or major depressive episode.
The primary treatments for bipolar disorder include medications and psychological counseling (psychotherapy) to control symptoms and also may include education and support groups.
Medications:
A number of medications are used to treat bipolar disorder. The types and doses of medications prescribed are based on your particular symptoms.
Medications may include:
- Mood stabilizers. You’ll typically need mood-stabilizing medication to control manic or hypomanic episodes. Examples of mood stabilizers include lithium (Lithobid), valproic acid (Depakene), divalproex sodium (Depakote), carbamazepine (Tegretol, Equetro, others), and lamotrigine (Lamictal).
- Antipsychotics. If symptoms of depression or mania persist in spite of treatment with other medications, adding an antipsychotic drug such as olanzapine (Zyprexa), risperidone (Risperdal), quetiapine (Seroquel), aripiprazole (Abilify), ziprasidone (Geodon), lurasidone (Latuda) or asenapine (Saphris) may help. Your doctor may prescribe some of these medications alone or along with a mood stabilizer.
- Antidepressants. Your doctor may add an antidepressant to help manage depression. Because an antidepressant can sometimes trigger a manic episode, it’s usually prescribed along with a mood stabilizer or antipsychotic.
- Antidepressant-antipsychotic. The medication Symbyax combines the antidepressant fluoxetine and the antipsychotic olanzapine. It works as a depression treatment and a mood stabilizer.
- Anti-anxiety medications. Benzodiazepines may help with anxiety and improve sleep but are usually used on a short-term basis.
Finding the right medication:
Finding the right medication or medications for you will likely take some trial and error. If one doesn’t work well for you, there are several others to try.
This process requires patience, as some medications need weeks to months to take full effect. Generally, only one medication is changed at a time so that your doctor can identify which medications work to relieve your symptoms with the least bothersome side effects. Medications also may need to be adjusted as your symptoms change.
Side effects:
Mild side effects often improve as you find the right medications and doses that work for you, and your body adjusts to the medications. Talk to your doctor or mental health professional if you have bothersome side effects.
Don’t make changes or stop taking your medications. If you stop your medication, you may experience withdrawal effects, or your symptoms may worsen or return. You may become very depressed, feel suicidal, or go into a manic or hypomanic episode. If you think you need to make a change, call your doctor.
Medications and pregnancy:
A number of medications for bipolar disorder can be associated with birth defects and can pass through breast milk to your baby. Certain medications, such as valproic acid and divalproex sodium, should not be used during pregnancy. Also, birth control medications may lose effectiveness when taken along with certain bipolar disorder medications.
Discuss treatment options with your doctor before you become pregnant, if possible. If you’re taking medication to treat your bipolar disorder and think you may be pregnant, talk to your doctor right away.
Psychotherapy:
Psychotherapy is a vital part of bipolar disorder treatment and can be provided in individual, family, or group settings. Several types of therapy may be helpful. These include:
- Interpersonal and social rhythm therapy (IPSRT). IPSRT focuses on the stabilization of daily rhythms, such as sleeping, waking, and mealtimes. A consistent routine allows for better mood management. People with bipolar disorder may benefit from establishing a daily routine for sleep, diet, and exercise.
- Cognitive-behavioral therapy (CBT). The focus is on identifying unhealthy, negative beliefs and behaviors and replacing them with healthy, positive ones. CBT can help identify what triggers your bipolar episodes. You also learn effective strategies to manage stress and to cope with upsetting situations.
- Psychoeducation. Learning about bipolar disorder (psychoeducation) can help you and your loved ones understand the condition. Knowing what’s going on can help you get the best support, identify issues, make a plan to prevent relapse, and stick with treatment.
- Family-focused therapy. Family support and communication can help you stick with your treatment plan and help you and your loved ones recognize and manage warning signs of mood swings.
Bipolar Disorder Video
Other treatment options:
Depending on your needs, other treatments may be added to your depression therapy.
During electroconvulsive therapy (ECT), electrical currents are passed through the brain, intentionally triggering a brief seizure. ECT seems to cause changes in brain chemistry that can reverse symptoms of certain mental illnesses. ECT may be an option for bipolar treatment if you don’t get better with medications, can’t take antidepressants for health reasons such as pregnancy, or are at high risk of suicide.
Transcranial magnetic stimulation (TMS) is being investigated as an option for those who haven’t responded to antidepressants.
Treatment in children and teenagers:
Treatments for children and teenagers are generally decided on a case-by-case basis, depending on symptoms, medication side effects, and other factors. Generally, treatment includes:
- Medications. Children and teens with bipolar disorder are often prescribed the same types of medications as those used in adults. There’s less research on the safety and effectiveness of bipolar medications in children than in adults, so treatment decisions are often based on adult research.
- Psychotherapy. Initial and long-term therapy can help keep symptoms from returning. Psychotherapy can help children and teens manage their routines, develop coping skills, address learning difficulties, resolve social problems, and help strengthen family bonds and communication. And, if needed, it can help treat substance abuse problems common in older children and teens with bipolar disorder.
- Psychoeducation. Psychoeducation can include learning the symptoms of bipolar disorder and how they differ from behavior related to your child’s developmental age, the situation, and appropriate cultural behavior. Understanding bipolar disorder can also help you support your child.
- Support. Working with teachers and school counselors and encouraging support from family and friends can help identify services and encourage success.
Lifestyle and home remedies:
You’ll probably need to make lifestyle changes to stop cycles of behavior that worsen your bipolar disorder. Here are some steps to take:
- Quit drinking or using recreational drugs. One of the biggest concerns with bipolar disorder is the negative consequences of risk-taking behavior and drug or alcohol abuse. Get help if you have trouble quitting on your own.
- Form healthy relationships. Surround yourself with people who are a positive influence. Friends and family members can provide support and help you watch for warning signs of mood shifts.
- Create a healthy routine. Having a regular routine for sleeping, eating, and physical activity can help balance your moods. Check with your doctor before starting any exercise program. Eat a healthy diet. If you take lithium, talk with your doctor about appropriate fluid and salt intake. If you have trouble sleeping, talk to your doctor or mental health professional about what you can do.
- Check first before taking other medications. Call the doctor who’s treating you for bipolar disorder before you take medications prescribed by another doctor or any over-the-counter supplements or medications. Sometimes other medications trigger episodes of depression or mania or may interfere with medications you’re taking for bipolar disorder.
- Consider keeping a mood chart. Keeping a record of your daily moods, treatments, sleep, activities, and feelings may help identify triggers, effective treatment options, and when treatment needs to be adjusted.
Alternative medicine:
There isn’t much research on alternative or complementary medicine — sometimes called integrative medicine — and bipolar disorder. Most of the studies are on major depression, so it isn’t clear how these nontraditional approaches work for bipolar disorder.
If you choose to use alternative or complementary medicine in addition to your physician-recommended treatment, take some precautions first:
- Don’t stop taking your prescribed medications or skip therapy sessions. Alternative or complementary medicine is not a substitute for regular medical care when it comes to treating bipolar disorder.
- Be honest with your doctors and mental health professionals. Tell them exactly which alternative or complementary treatments you use or would like to try.
- Be aware of potential dangers. Alternative and complementary products aren’t regulated the way prescription drugs are. Just because it’s natural doesn’t mean it’s safe. Before using alternative or complementary medicine, talk to your doctor about the risks, including possible serious interactions with medications.
Coping and support:
Coping with bipolar disorder can be challenging. Here are some strategies that can help:
- Learn about bipolar disorder. Education about your condition can empower you and motivate you to stick to your treatment plan and recognize mood changes. Help educate your family and friends about what you’re going through.
- Stay focused on your goals. Learning to manage bipolar disorder can take time. Stay motivated by keeping your goals in mind and reminding yourself that you can work to repair damaged relationships and other problems caused by your mood swings.
- Join a support group. Support groups for people with bipolar disorder can help you connect to others facing similar challenges and share experiences.
- Find healthy outlets. Explore healthy ways to channel your energy, such as hobbies, exercise, and recreational activities.
- Learn ways to relax and manage stress. Yoga, tai chi, massage, meditation, or other relaxation techniques can be helpful.
Herbal Remedies for Bipolar Disorder:
Many herbs have been used to treat different conditions through the ages. Herbalists call these substances nervines, and some may prove useful for treating specific symptoms of bipolar disorder.
Of all the herbs, the nervines group of plant extracts is among the strongest and so are the most likely to cause serious side effects. Because of this possibility, you should always consult with your physician first before trying any of these herbs — especially if you are already taking medication for bipolar disorder.
The common types of nervines that have been tried by people with bipolar disorder include:
- Black cohosh (Cimicifuga racemosa). A nervous system depressant and sedative, sometimes used by people with autoimmune conditions for its anti-inflammatory effects. Its active ingredient appears to bind to estrogen receptor sites, so it may cause hormonal activity.
- Damiana (Turnera aphrodisiaca). A traditional remedy for depression. As its Latin name indicates, it is also believed to have aphrodisiac properties. Whatever the case may be there, it does seem to act on the hormonal system. Its energizing quality might be dangerous for bipolar patients.
- Gingko Biloba. An extract of the ginkgo tree is advertised as an herb that can improve your memory. There is some clinical evidence for this claim. It is an antioxidant and is prescribed in Germany for the treatment of dementia. It is believed to increase blood flow to the brain.
- Ginseng (Panax quinquefolium). It has an energizing effect that may be helpful to people whose depression is accompanied by extreme fatigue and lethargy.
- Grapeseed oil and pycnogenol. Both are extra-powerful antioxidants. (Pycnogenol is derived from marine pine trees.)
- Gotu kola (Centella asiatica, Hydrocotyl asiatica). An Ayurvedic herbal stimulant is sometimes recommended for depression and anxiety.
- Licorice (Glycyrrhiza glabra, Liquiritia officinalis). Boosts hormone production, including hormones active in the digestive tract and brain.
- Sarsaparilla (Hemidesmus indicus). Like licorice, it seems to affect hormone production as well as settling the stomach and calming the nerves.
- St. John’s Wort (Hypericum perforatum). Has gained popularity as an herbal antidepressant. It has the backing of a decent amount of research. Those choosing to use this remedy should follow the same precautions as with SSRIs and MAOIs, two families of pharmaceutical antidepressants. It can also cause increased sensitivity to light. It is available by prescription in Germany, where it is the most widely used antidepressant. It is potentially dangerous to use St. John’s Wort with prescription antidepressants or any other medication that could affect serotonin.
Although most herbal remedies are relatively safe, you should consult with your doctor before trying one of these. Some herbs interact badly with certain medications and can lead to serious and possibly harmful side effects.
It is important that you see your doctor if you suffer from mood changes, sometimes not knowing why.
Thank you for reading
Michael
Comments are welcome
Bipolar is a serious condition needing help in all the levels of life. As the symptoms vary in different people, the overall result is very similar. We have 2 in our extended family who have been diagnosed and treated for many years. They both are wonderful people but have dealt with the serious highs and lows that go with the Bipolar condition.
When the symptoms began in the older member of our family many years ago, the diagnosis was not as complete, and treatment not as successful. As time went by the family and the ill one learned to cope, and seem to have been able to live a life, help support the family and be a member of the community. The younger one has not been able to stay in her chosen employment, even though well educated. This seems to be a measurement of the self-worth of this person.
The lives of Bipolst individuals is not always a smooth one and requires a lot of time to work through. Thank you for your informative article about this condition.
Hi Sami,
Thank you for your comments. Suffering from bipolar disorder is very hard. Support from friends and family is very essential. This is a recognized disease and about just feeling bad or depressed.
I hope the support will always be there.
All the best,
Michael
Relatives or friend can help someone with bipolar disorder during a manic episode by doing the following. Spending time with the person, depending on his or her level of energy and how well you can keep up. People who are manic often feel isolated from other people. Spending even short periods of time with them helps them feel less isolated and have the feelings not being loved
Hi edahnewton,
Thank you for your comments. You are absolutely right. A trusted non-judgemental relative or friend is crucial to the person suffering through any type of depressive episode. Unfortunately, many people who suffer from depression do not realize they are suffering from a medical condition caused by a chemical imbalance in the brain. These people feel guilty and this is sad.
All the best,
Michael
Nice article on bipolar disorder. This is one of the most detailed write up i have come across in a while. I learn a lot of new things reading through and i now know how to handle bipolar cases just incase i am faced with one. I want to ask is there a cure to bipolar disaorder like can someone get totally off it?
Hi Iheanacho,
Thank you for your comments. Being an understanding friend, without judgement is very important to the person who may be suffering from any type of depressive disorder. This is a medical condition caused by a chemical imbalance in the brain. Unfortunately, there are no real cures. There are treatments, which may be found through prescription drugs, herbal remedies and certain exercises such as yoga and practising meditation. I suffer from bipolar disorder and for many years I was on prescription drugs. Unfortunately, the side effects were nasty:
https://empoweryourlifestyles…. I have been able to get off the prescription medications and practice the alternate methods to relieve my episodes. Please always follow the doctor’s recommendations.
All the best,
Michael
Hello there, This is an amazing article that you have got here. Indeed ghe bipolar disorder can result in huge catastrophy and may linger for too long in na individual. With all this description, I wander the danger that the individual would have caused to his or her own self. is there a particular place where a psychotherapist can be sought.
Hi Steviejohn,
Thank you for your comments. If someone feels depressed it is important they share their feelings with someone they can confide in and trust. The next step is to see their doctor. In most cases, if not in all the doctor will refer this individual to a psychiatrist, psychologist, or psychotherapist. Recently the statics for suicide have risen, and that is sad. Anyone who feels depressed should know it is a medical condition, and not feel guilty about it. They are not alone. I suffer from this disease.
All the best,
Michael