COPD. Causes, Treatments, Prevention.
Blue indicates link
We live in a world full of pollution, climate change seems to be obvious. Why do we continue to abuse our bodies by smoking to excess, and drinking too much alcohol in some cases? We are supposed to be the smartest form of life on this planet, yet there are some of us who continue to abuse our bodies and our world. One lifetime, one planet!!!
What is COPD?
COPD means Chronic Obstructive Pulmonary Disease. It is a term that covers two types of chronic (long-term) diseases where the airways (breathing tubes) in the lungs become swollen and partly
blocked. COPD gets worse over time. It cannot be cured, but it can be treated and managed.
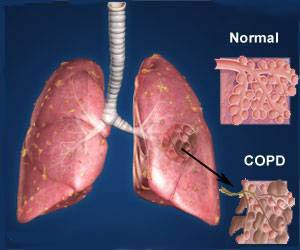
COPD consists of two major breathing diseases:
- emphysema
- chronic bronchitis
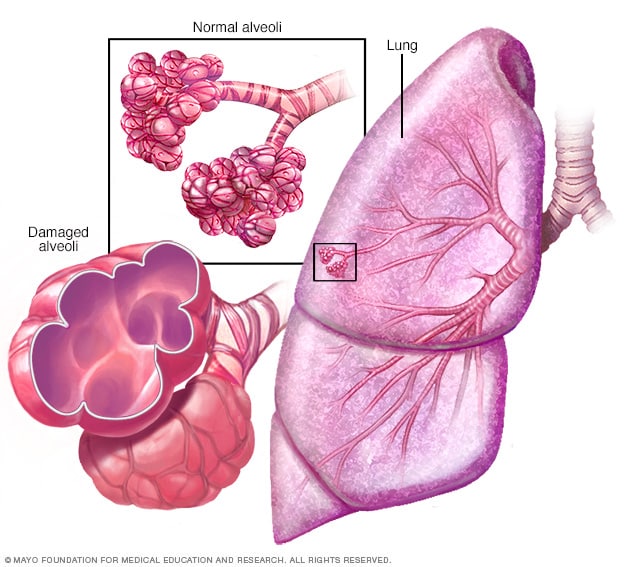
Emphysema damages the tiny alveoli (air sacs) at the tips of your lungs. Normally these air sacs stretch like balloons as you breathe in and out. Emphysema makes these air sacs stiff. Because they cannot stretch, the air gets trapped inside them. This makes it difficult for you to breathe in and makes you feel tired.
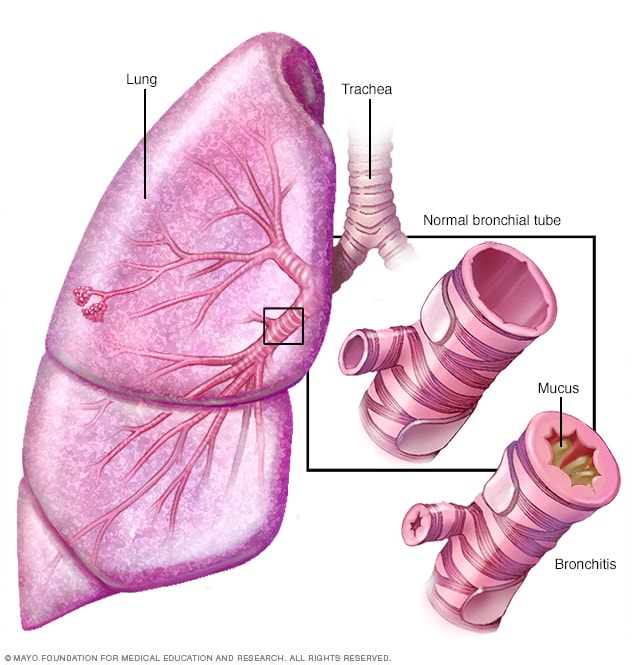
Chronic bronchitis makes your airways red, swollen, and irritated. Glands in your airways make extra mucus (phlegm), which blocks some air from passing through. This makes you cough, cough up mucus, and feel short of breath.
Many people with COPD have both of these diseases.
Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, mucus (sputum) production, and wheezing. It’s caused by long-term exposure to irritating gases or particulate matter, most often from cigarette smoke. People with COPD are at increased risk of developing heart disease, lung cancer, and a variety of other conditions.
Emphysema and chronic bronchitis are the two most common conditions that contribute to COPD. Chronic bronchitis is inflammation of the lining of the bronchial tubes, which carry air to and from the air sacs (alveoli) of the lungs. It’s characterized by daily cough and mucus (sputum) production.
Emphysema is a condition in which the alveoli at the end of the smallest air passages (bronchioles) of the lungs are destroyed as a result of damaging exposure to cigarette smoke and other irritating gases and particulate matter.
COPD is treatable. With proper management, most people with COPD can achieve good symptom control and quality of life, as well as reduced risk of other associated conditions.
Symptoms
COPD symptoms often don’t appear until significant lung damage has occurred, and they usually worsen over time, particularly if smoking exposure continues. For chronic bronchitis, the main symptom is a daily cough and mucus (sputum) production at least three months a year for two consecutive years.
Other signs and symptoms of COPD may include:
- Shortness of breath, especially during physical activities
- Wheezing
- Chest tightness
- Having to clear your throat first thing in the morning, due to excess mucus in your lungs
- A chronic cough that may produce mucus (sputum) that may be clear, white, yellow or greenish
- The blueness of the lips or fingernail beds (cyanosis)
- Frequent respiratory infections
- Lack of energy
- Unintended weight loss (in later stages)
- Swelling in ankles, feet, or legs
People with COPD are also likely to experience episodes called exacerbations, during which their symptoms become worse than usual day-to-day variation and persist for at least several days.
Causes
The main cause of COPD in developed countries is tobacco smoking. In the developing world, COPD often occurs in people exposed to fumes from burning fuel for cooking and heating in poorly ventilated homes. Only about 20 to 30 percent of chronic smokers may develop clinically apparent COPD, although many smokers with long smoking histories may develop reduced lung function. Some smokers develop less common lung conditions. They may be misdiagnosed as having COPD until a more thorough evaluation is performed.
How your lungs are affected
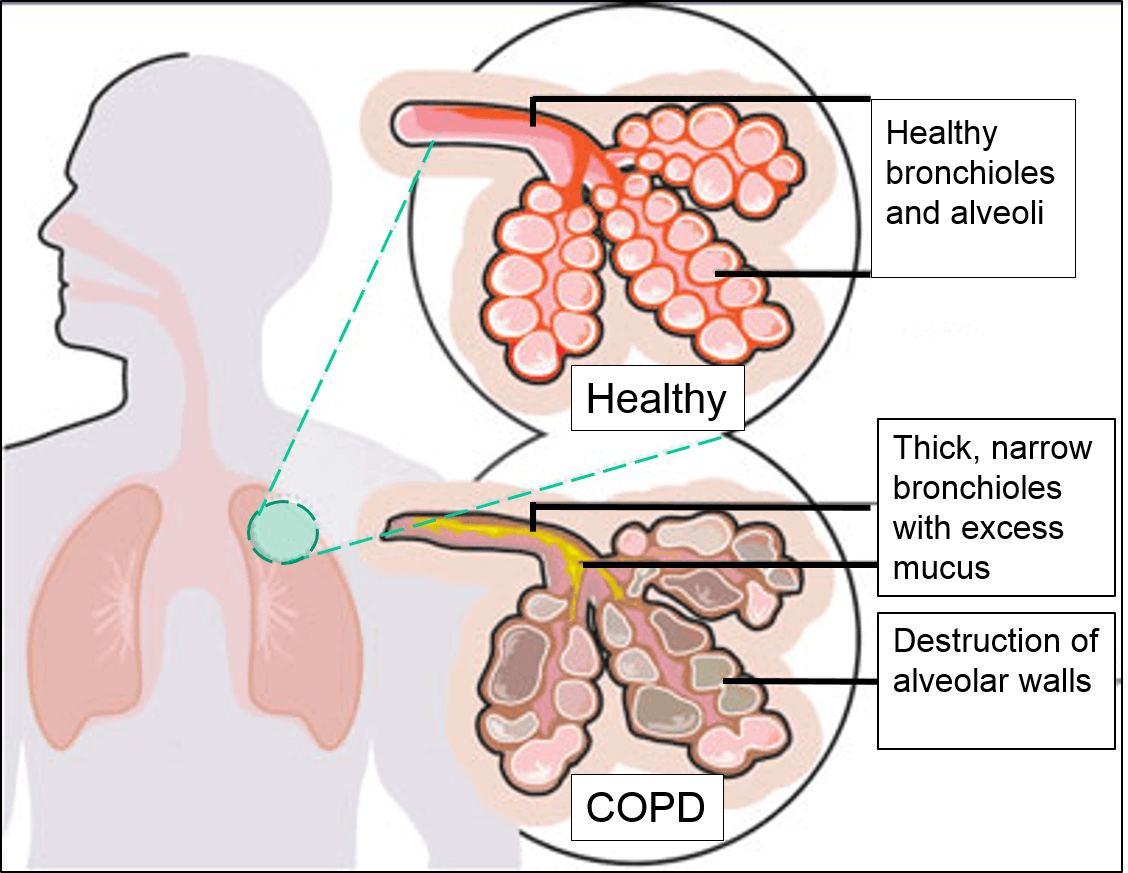
Air travels down your windpipe (trachea) and into your lungs through two large tubes (bronchi). Inside your lungs, these tubes divide many times — like the branches of a tree — into many smaller tubes (bronchioles) that end in clusters of tiny air sacs (alveoli).
The air sacs have very thin walls full of tiny blood vessels (capillaries). The oxygen in the air you inhale passes into these blood vessels and enters your bloodstream. At the same time, carbon dioxide — a gas that is a waste product of metabolism — is exhaled.
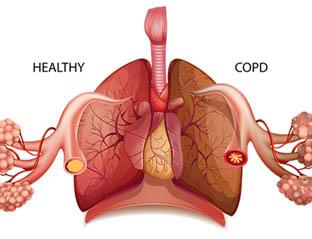
Your lungs rely on the natural elasticity of the bronchial tubes and air sacs to force air out of your body. COPD causes them to lose their elasticity and over-expand, which leaves some air trapped in your lungs when you exhale.


Emphysema Bronchitis
Causes of airway obstruction include:
- Emphysema. This lung disease causes the destruction of the fragile walls and elastic fibers of the alveoli. Small airways collapse when you exhale, impairing airflow out of your lungs.
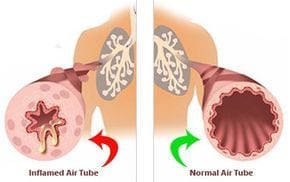
- Chronic bronchitis. In this condition, your bronchial tubes become inflamed and narrowed and your lungs produce more mucus, which can further block the narrowed tubes. You develop a chronic cough trying to clear your airways.
Cigarette smoke and other irritants
In the vast majority of cases, the lung damage that leads to COPD is caused by long-term cigarette smoking. But there are likely other factors at play in the development of COPD, such as a genetic susceptibility to the disease, because only about 20 to 30 percent of smokers may develop COPD.
Other irritants can cause COPD, including cigar smoke, secondhand smoke, pipe smoke, air pollution, and workplace exposure to dust, smoke, or fumes.
Alpha-1-antitrypsin deficiency
In about 1 percent of people with COPD, the disease results from a genetic disorder that causes low levels of a protein called alpha-1-antitrypsin. Alpha-1-antitrypsin (AAt) is made in the liver and secreted into the bloodstream to help protect the lungs. Alpha-1-antitrypsin deficiency can affect the liver as well as the lungs. Damage to the lungs can occur in infants and children, not only in adults with long smoking histories.
For adults with COPD related to AAt deficiency, treatment options include those used for people with more common types of COPD. In addition, some people can be treated by replacing the missing AAt protein, which may prevent further damage to the lungs.
In developed countries like the United States, the single biggest cause of COPD is cigarette smoking. About 90 percent of people who have COPD are smokers or former smokers.
Among long-time smokers, 20 to 30 percent develop COPD. Many others develop lung conditions or have reduced lung function.
Most people with COPD are at least 40 years old and have at least some history of smoking. The longer and more tobacco products you smoke, the greater your risk of COPD is. In addition to cigarette smoke, cigar smoke, pipe smoke, and secondhand smoke can cause COPD.
Your risk of COPD is even greater if you have asthma and smoke.
You can also develop COPD if you’re exposed to chemicals and fumes in the workplace. Long-term exposure to air pollution and inhaling dust can also cause COPD.
In developing countries, along with tobacco smoke, homes are often poorly ventilated, forcing families to breathe fumes from burning fuel used for cooking and heating.
There may be a genetic predisposition to developing COPD. Up to an estimated 5 percent of people with COPD have a deficiency in a protein called alpha-1-antitrypsin. This deficiency causes the lungs to deteriorate and also can affect the liver. There may be other associated genetic factors at play as well.
COPD isn’t contagious.
Diagnosing COPD
There’s no single test for COPD. Diagnosis is based on symptoms, a physical exam, and diagnostic test results.
When you visit the doctor, be sure to mention all of your symptoms. Tell your doctor if:
- you’re a smoker or have smoked in the past
- You’re exposed to lung irritants on the job
- You’re exposed to a lot of secondhand smoke
- You have a family history of COPD
- you have asthma or other respiratory conditions
- You take over-the-counter or prescription medications
During the physical exam, your doctor will use a stethoscope to listen to your lungs as you breathe. Based on all this information, your doctor may order some of these tests to get a more complete picture:
- Spirometry is a noninvasive test to assess lung function. During the test, you’ll take a deep breath and then blow into a tube connected to the spirometer.
- Imaging tests include a chest X-ray or CT scan. These images can provide a detailed look at your lungs, blood vessels, and heart.
- An arterial blood gas test involves taking a blood sample from an artery to measure your blood oxygen, carbon dioxide, and other important levels.
These tests can help determine if you have COPD or a different condition, such as asthma, restrictive lung disease, or heart failure.
Treatment for COPD
Treatment can ease symptoms, prevent complications, and generally slow disease progression. Your healthcare team may include a lung specialist (pulmonologist) and physical and respiratory therapists.
Medication
Bronchodilators are medications that help relax the muscles of the airways, widening the airways so you can breathe easier. They’re usually taken through an inhaler or a nebulizer. Glucocorticosteroids can be added to reduce inflammation in the airways.
To lower the risk of other respiratory infections, ask your doctor if you should get a yearly flu shot, pneumococcal vaccine, and a tetanus booster that includes protection from pertussis (whooping cough).
Oxygen therapy
If your blood oxygen level is too low, you can receive supplemental oxygen through a mask or nasal cannula to help you breathe better. A portable unit can make it easier to get around.
Surgery
Surgery is reserved for severe COPD or when other treatments have failed, which is more likely when you have a form of severe emphysema.
One type of surgery is called bullectomy. During this procedure, surgeons remove large, abnormal air spaces (bullae) from the lungs.
Another is lung volume reduction surgery, which removes damaged upper lung tissue.
Lung transplantation is an option in some cases.
Lifestyle changes
Certain lifestyle changes may also help alleviate your symptoms or provide relief.
- If you smoke, quit. Your doctor can recommend appropriate products or support services.
- Whenever possible, avoid secondhand smoke and chemical fumes.
- Get the nutrition your body needs. Work with your doctor or dietician to create a healthy eating plan.
- Talk to your doctor about how much exercise is safe for you.
Medications for COPD
Medications can reduce symptoms and cut down on flare-ups. It may take some trial and error to find the medication and dosage that works best for you. These are some of your options:
Inhaled bronchodilators
Medicines called bronchodilators help loosen the tight muscles of your airways. They’re typically taken through an inhaler or nebulizer.
Short-acting bronchodilators last from four to six hours. You only use them when you need them. For ongoing symptoms, there are long-acting versions you can use every day. They last about 12 hours.
Some bronchodilators are selective beta-2-agonists, and others are anticholinergics. These bronchodilators work by relaxing tightened muscles of the airways, which widens your airways for better air passage. They also help your body clear mucus from the lungs. These two types of bronchodilators can be taken separately or in combination by inhaler or with a nebulizer.
Corticosteroids
Long-acting bronchodilators are commonly combined with inhaled glucocorticosteroids. A glucocorticosteroid can reduce inflammation in the airways and lower mucus production. The long-acting bronchodilator can relax the airway muscle to help the airways stay wider. Corticosteroids are also available in pill form.
Phosphodiesterase-4 inhibitors
This type of medication can be taken in pill form to help reduce inflammation and relax the airways. It’s generally prescribed for severe COPD with chronic bronchitis.
Theophylline
This medication eases chest tightness and shortness of breath. It may also help prevent flare-ups. It’s available in pill form. Theophylline is an older medication that relaxes the muscles of the airways, and it may cause side effects. It’s generally not a first-line treatment for COPD therapy.
Antibiotics and antivirals
Antibiotics or antivirals may be prescribed when you develop certain respiratory infections.
Vaccines
COPD increases your risk of other respiratory problems. For that reason, your doctor might recommend that you get a yearly flu shot, the pneumococcal vaccine, or the whooping cough vaccine.
Diet recommendations for people with COPD
There’s no specific diet for COPD, but a healthy diet is important for maintaining overall health. The stronger you are, the more able you’ll be to prevent complications and other health problems.
Choose a variety of nutritious foods from these groups:
- vegetables
- fruits
- grains
- protein
- dairy
Drink plenty of fluids. Drinking at least six to eight, 8-ounce glasses of non-caffeinated liquids a day can help keep mucus thinner. This may make the mucus easier to cough out.
Limit caffeinated beverages because they can interfere with medications. If you have heart problems, you may need to drink less, so talk to your doctor.
Go easy on the salt. It causes the body to retain water, which can strain your breathing.
Maintaining a healthy weight is important. It takes more energy to breathe when you have COPD, so you might need to take in more calories. But if you’re overweight, your lungs and heart may have to work harder.
If you’re underweight or frail, even basic body maintenance can become difficult. Overall, having COPD weakens your immune system and decreases your ability to fight off infection.
A full stomach makes it harder for your lungs to expand, leaving you short of breath. If that happens, try these remedies:
- Clear your airways about an hour before a meal.
- Take smaller bites of food that you chew slowly before swallowing.
- Swap three meals a day for five or six smaller meals.
- Save fluids until the end so you feel less full during the meal.
Living with COPD
COPD requires lifelong disease management. That means following the advice of your healthcare team and maintaining healthy lifestyle habits.
Since your lungs are weakened, you’ll want to avoid anything that might overtax them or cause a flare-up.
Number one on the list of things to avoid is smoking. If you’re having trouble quitting, talk to your doctor about smoking cessation programs. Try to avoid secondhand smoke, chemical fumes, air pollution, and dust.
A little exercise each day can help you stay strong. Talk to your doctor about how much exercise is good for you.
Eat a diet of nutritious foods. Avoid highly processed foods that are loaded with calories and salt but lack nutrients.
If you have other chronic diseases along with COPD, it’s important to manage those as well, particularly diabetes mellitus and heart disease.
Clear the clutter and streamline your home so that it takes less energy to clean and do other household tasks. If you have advanced COPD, get help with daily chores.
Be prepared for flare-ups. Carry your emergency contact information with you and post it on your refrigerator. Include information about what medications you take, as well as the doses. Program emergency numbers into your phone.
It can be a relief to talk to others who understand. Consider joining a support group. The COPD Foundation provides a comprehensive list of organizations and resources for people living with COPD.
What are the stages of COPD?
One measure of COPD is achieved by spirometry grading. There are different grading systems, and one grading system is part of the GOLD classification. The GOLD classification is used for determining COPD severity and helping to form a prognosis and treatment plan.
There are four GOLD grades based on spirometry testing:
- Grade 1: mild
- Grade 2: moderate
- Grade 3: severe
- Grade 4: Very severe
This is based on the spirometry test result of your FEV1. This is the amount of air you can breathe out of the lungs in the first second of forced expiration. The severity increases as your FEV1 decreases.
The GOLD classification also takes into account your individual symptoms and a history of acute exacerbations. Based on this information, your doctor can assign a letter group to you to help define your COPD grade.
As the disease progresses, you’re more susceptible to complications, such as:
- respiratory infections, including common colds, flu, and pneumonia
- heart problems
- High blood pressure in lung arteries (pulmonary hypertension)
- lung cancer
- depression and anxiety
Is there a connection between COPD and lung cancer?
COPD and lung cancer are major health problems worldwide. These two diseases are linked in a number of ways.
COPD and lung cancer have several common risk factors. Smoking is the number one risk factor for both diseases. Both are more likely if you breathe secondhand smoke, or are exposed to chemicals or other fumes in the workplace.
There may be a genetic predisposition to developing both diseases. Also, the risk of developing either COPD or lung cancer increases with age.
It was estimated in 2009 that between 40 and 70 percent of people with lung cancer also have COPD. This same 2009 study concluded that COPD is a risk factor for lung cancer.
A 2015 study suggests they may actually be different aspects of the same disease, and that COPD could be a driving factor in lung cancer.
In some cases, people don’t learn they have COPD until they’re diagnosed with lung cancer.
However, having COPD doesn’t necessarily mean you’ll get lung cancer. It does mean that you have a higher risk. That’s another reason why, if you smoke, quitting is a good idea.
COPD statistics
Worldwide, it’s estimated that about 65 million people have moderate to severe COPD. About 12 million adults in the United States have a diagnosis of COPD. It’s estimated that 12 million more have the disease, but don’t know it yet.
Most people with COPD are 40 years of age or older.
The majority of people with COPD are smokers or former smokers. Smoking is the most important risk factor that can be changed. Between 20 and 30 percent of chronic smokers develop COPD which shows symptoms and signs.
Between 10 and 20 percent of people with COPD have never smoked. In up to 5 percent of people with COPD, the cause is a genetic disorder involving a deficiency of a protein called alpha-1-antitrypsin.
COPD is a leading cause of hospitalizations in industrialized countries. In the United States, COPD is responsible for a large number of emergency department visits and hospital admissions. In the year 2000, it was noted that there were over 700,000 hospital admissions and approximately 1.5 million emergency department visits. Among people with lung cancer, between 40 and 70 percent also have COPD.
About 120,000 people die from COPD each year in the United States. It’s the third leading cause of death in the United States. More women than men die from COPD each year.
It’s projected that the number of patients diagnosed with COPD will increase by more than 150 percent from 2010 to 2030. Much of that can be attributed to an aging population.
What’s the outlook for people with COPD?
COPD tends to progress slowly. You may not even know you have it during the early stages.
Once you have a diagnosis, you’ll need to start seeing your doctor on a regular basis. You’ll also have to take steps to manage your condition and make the appropriate changes to your daily life.
Early symptoms can usually be managed, and certain lifestyle choices can help you maintain a good quality of life for some time.
As the disease progresses, symptoms can become increasingly limiting.
People with severe stages of COPD may not be able to care for themselves without assistance. They are at increased risk of developing respiratory infections, heart problems, and lung cancer. They may also be at risk of depression and anxiety.
COPD generally reduces life expectancy, though the outlook varies considerably from person to person. People with COPD who never smoked may have a modest reduction in life expectancy, while former and current smokers are likely to have a larger reduction.
Besides smoking, your outlook depends on how well you respond to treatment and whether you can avoid serious complications. Your doctor is in the best position to evaluate your overall health and give you an idea about what to expect.
Breathing Exercises to Increase Lung Capacity
Overview
Your lung capacity is the total amount of air that your lungs can hold. Over time, our lung capacity and lung function typically decrease slowly as we age after our mid-20s.
Some conditions like chronic obstructive pulmonary disease (COPD) can significantly speed up these reductions in lung capacity and functioning. This leads to difficulty in breathing and shortness of breath.
Fortunately, there are exercises that can help maintain and increase lung capacity, making it easier to keep your lungs healthy and get your body the oxygen it needs.
1. Diaphragmatic breathing
Diaphragmatic breathing, or “belly breathing,” engages the diaphragm, which is supposed to do most of the heavy lifting when it comes to breathing.
This technique is particularly helpful in people with COPD, as the diaphragm isn’t as effective in these individuals and could be strengthened. The technique is best used when feeling rested.
If you have COPD, ask your doctor or respiratory therapist to show you how to use this exercise for the best results.
According to the COPD Foundation, you should do the following to practice diaphragmatic breathing:
- Relax your shoulders and sit back or lie down.
- Place one hand on your belly and one on your chest.
- Inhale through your nose for two seconds, feeling the air move into your abdomen and feeling your stomach move out. Your stomach should move more than your chest does.
- Breathe out for two seconds through pursed lips while pressing on your abdomen.
- Repeat.
 The Best Places to Live with COPD
The Best Places to Live with COPD COPD: Facts, Statistics, and You
COPD: Facts, Statistics, and You COPD: Symptoms and Patient Groups
COPD: Symptoms and Patient Groups
A diet higher in fat, and lower in carbs may be best
A reduced carbohydrate diet results in lower carbon dioxide production. This may help people with COPD better manage their health.
According to a study in the Lung Journal in 2015, healthy subjects following a ketogenic diet had a lower carbon dioxide output and carbon dioxide end-tidal partial pressure (PETCO2) compared to those following a Mediterranean diet.
In addition, research from 2003 shows improvement in people with COPD who took a high-fat, low-carb supplement instead of eating a high-carb diet.
Even when reducing carbohydrates, a healthy diet includes a variety of foods. Try to include these in your daily diet.
Protein-rich foods
Eat high-protein, high-quality foods, such as grass-fed meat, pastured poultry and eggs, and fish — particularly oily fish such as salmon, mackerel, and sardines.
Complex carbohydrates
If you include carbohydrates in your diet, opt for complex carbohydrates. These foods are high in fiber, which helps improve the function of the digestive system and blood sugar management.
Foods to incorporate into your diet include:
Fresh produce
Fresh fruits and vegetables contain essential vitamins, minerals, and fiber. These nutrients will help to keep your body healthy. Non-starchy vegetables (all except peas, potatoes, and corn) are low in carbohydrates, so they can be included in all diets.
Some fruits and vegetables are more suitable than others — check out the list of foods to avoid in the next section to find out more.
Potassium-rich foods
Potassium is vital to lung function, so a potassium deficiency can cause breathing issues. Try to eat foods containing high levels of potassium, such as:
Potassium-rich foods can be especially useful if your dietitian or doctor has prescribed you a diuretic medication.
Healthy fats
When choosing to eat a higher-fat diet, instead of choosing fried foods, opt for snacks and meals containing fats like avocados, nuts, seeds, coconut and coconut oil, olives, olive oil, fatty fish, and cheese. These foods will provide more overall nutrition, especially in the long term.
Know what to avoid
Certain foods can cause problems such as gas and bloating or may have little to no nutritional value. Foods to avoid or minimize include:
Salt
Too much sodium or salt in your diet causes water retention, which may affect your ability to breathe. Remove the salt shaker from the table and don’t add salt to your cooking. Use unsalted herbs and spices to flavor food instead.
Check with your dietitian or healthcare provider about low-sodium salt substitutes. They may contain ingredients that could affect your health negatively.
Despite what many people believe, most sodium intake doesn’t come from the salt shaker, but rather from what’s already in the food.
Be sure to check the labels of the foods you buy. Your snacks should contain no more than 300 milligrams (mg) of sodium per serving. Whole meals should have no more than 600 mg.
Some fruits
Apples, stone fruits such as apricots peaches, and melons may cause bloating and gas in some people due to their fermentable carbohydrates. This may lead to breathing problems in people with COPD.
Instead, you can focus on low fermentable or low FODMAP fruits like berries, pineapple, and grapes. However, if these foods aren’t a problem for you and your carbohydrate goal allows for fruit, you can include them in your diet.
Some vegetables and legumes
There’s a long list of vegetables and legumes known to cause bloating and gas. What matters is how your body works.
You may want to monitor your intake of the foods below. However, you can continue to enjoy them if they don’t cause a problem for you:
- beans
- Brussels sprouts
- cabbage
- cauliflower
- corn
- leeks
- some lentils
- onions
- peas
Soybeans may also cause gas.
Dairy products
Some people find that dairy products, such as milk and cheese, make phlegm thicker. However, if dairy products don’t seem to make your phlegm worse, you can continue to eat them.
Chocolate
Chocolate contains caffeine, which may interfere with your medication. Check with your doctor to find out if you should avoid or limit your intake.
Fried foods
Foods that are fried, deep-fried, or greasy can cause gas and indigestion. Heavily spiced foods may also cause discomfort and may affect your breathing. Avoid these foods when possible.
Don’t forget to watch what you drink
People with COPD should try to drink plenty of fluids throughout the day. Around six to eight 8-ounce glasses of non-caffeinated beverages are recommended per day. Adequate hydration keeps mucus thin and makes it easier to cough up.
Limit or avoid caffeine altogether, as it could interfere with your medication. Caffeinated drinks include coffee, tea, soda, and energy drinks, such as Red Bull.
Ask your doctor about alcohol. You may be advised to avoid or limit alcoholic beverages, as they can interact with medications. Alcohol may also slow down your breathing rate and make it more difficult to cough up mucus.
Likewise, talk to your doctor if you have been diagnosed with heart problems as well as COPD. Sometimes it’s necessary for people with heart problems to limit their fluid intake.
Watch your weight — in both directions
People with chronic bronchitis have a tendency to be obese, while those with emphysema have a tendency to be underweight. This makes diet and nutrition assessment a vital part of COPD treatment.
If you’re overweight
When you’re overweight, your heart and lungs have to work harder, making breathing more difficult. Excess body weight may also increase the demand for oxygen.
Your doctor or dietitian can advise you on how to achieve a healthier body weight by following a customized eating plan and an achievable exercise program.
If you’re underweight
Some symptoms of COPD, such as lack of appetite, depression, or feeling unwell in general, can cause you to become underweight. If you’re underweight, you may feel weak and tired or be more prone to infections.
COPD requires you to use more energy when breathing. According to the Cleveland Clinic, a person with COPD may burn up to 10 times as many calories when breathing as a person without COPD.
If you’re underweight, you need to include healthy, high-calorie snacks in your diet. Items to add to your grocery list include:
Be prepared for mealtime
COPD can be a challenging condition to live with, so it’s important to make food preparation a straightforward and stress-free process. Make mealtime easier, encourage your appetite if you’re underweight, and stick to a healthy eating program by following these general guidelines:
Eat small meals
Try eating five to six small meals per day rather than three large ones. Eating smaller meals may help you avoid filling up your stomach too much and give your lungs enough room to expand, making breathing easier.
Eat your main meal early
Try to eat your main meal early in the day. This will boost your energy levels for the whole day.
Choose quick and easy foods
Choose foods that are quick and easy to prepare. This will help you to avoid wasting energy. Sit down when preparing meals so that you aren’t too tired to eat and ask family and friends to assist you with meal preparation if necessary.
You may also be eligible for a meal home delivery service.
Get comfortable
Sit up comfortably in a high-backed chair when eating to avoid putting too much pressure on your lungs.
Make enough for leftovers
When making a meal, make a bigger portion so that you can refrigerate or freeze some for later and have nutritious meals available when you feel too tired to cook.
The takeaway
It’s important to stay mindful of your overall health when you have COPD, and nutrition is a big part of that. Planning healthy meals and snacks while emphasizing higher fat intake can help you manage symptoms and minimize complications.
ALWAYS CONSULT YOUR DOCTOR FIRST IF YOU HAVE ANY TYPE OF BREATHING PROBLEMS
Natural Treatment For COPD
Omega-3 fatty acids are a kind of polyunsaturated fatty acids. They are beneficial for COPD patients as they are good anti-inflammatory agents. They also improve breathing difficulties. They are also good antioxidants, which destroy the free radicals that are associated with COPD.
Fish varieties like sardines, herring, mackerel, trout, salmon, and tuna are rich sources of omega-3 fatty acids. The vegetarian alternatives are flaxseeds and walnuts. They are also found in fish oil supplements.
Vitamin C also helps in the healthy functioning of the lungs. Citrus fruits, papaya, broccoli, and many vegetables are rich sources of this nutrient. Vitamin C is also available as a supplement.
Magnesium levels are generally low in people suffering from COPD. Magnesium is an important mineral that aids in lung functioning. Magnesium supplements have proven to be beneficial for COPD.
Herbs
Herbs have been used to treat various lung diseases and lung infections since ancient times. Herbs ease the symptoms and have no side effects. Many herbs are used to treat COPD. The most common herbs used are:
Ginseng roots are good for patients suffering from COPD. It increases oxygen intake and improves ventilation. Patients with advanced COPD showed positive results with Ginseng intake.
Ginkgo is a very good antioxidant. It is used to treat various diseases. Ginkgo helps in clearing the airways of the lungs and improves its functioning. It is generally taken thrice a day.
Olive leaf has anti-inflammatory properties. It is also a natural antibiotic. These leaves reduce lung inflammation and relieve the infection caused by COPD.
Comfrey leaves are widely used for their active healing properties. It relieves the inflammation in the membranes of the bronchia. It also discharges the mucous from the tubes and membranes of the lungs.
Relaxation Techniques
Yoga
The specific breathing exercises of yoga can provide the lungs with more oxygen. It can also calm the mind and help you relax. These exercises improve the air circulation to the lungs and ease the blocked airways. Yoga moves have proved beneficial even for patients with severe COPD.
Massage
Massage helps your body relax thereby reducing stress and hormones related to stress such as cortisol. For patients with COPD, massage elevates pulmonary functions, strengthens the muscles that aid respiration, and reduces shortness of breath.
Home Remedies
Certain home remedies have proven to be beneficial in relieving the symptoms of COPD. To overcome severe cough, inhaling a few drops of frankincense oil on a piece of cloth, several times a day can help.
Black tea can ease breathing by opening up the air passages in the lungs. The active chemical in black tea, theophylline is responsible for this. Three to four cups of black tea per day can help.
Acupressure For COPD
This age-old Chinese pressure-based massage technique helps people with COPD breathe easier. The pressure applied to certain points in the body distributes energy within and revives comfort. As a result, it aids easy breathing.
Natural treatment methods have shown promising results in many patients. However, one should make sure that natural remedies do not interact with the prescribed drugs.
Thank you for reading.
Comments are welcome.
Michael



Hi there
Wow is all I can say it must of taken years to add all of that content I had a good read and really enjoyed your articles I have bookmarked you website for reference in future to read when I have more more all the links I have tried on your site work great and it all comes together great I signed up to email and subscribe as well so look for forward to the next article
Thanks
Hi J Little,
Thank you for your comments and support. Much appreciated.
Best wishes,
Michael
Hello Michael, thank you for sharing this helpful and educating post on the beginning stages of COPD. We have been told several times to stay clear of pollutants such as smoke, dust and others. Now I see the reason behind this warning. Thank you for sharing your advice and recommendations regarding this ailment.
Peace out!
Hi MrBiizy,
Thank you for your comments.
Best wishes,
Michael
I have to say Michael, this article addresses a major in this time and age. This Chronic obstructive pulmonary disease is indeed life-threatening and should never be taken lightly. I smoke occasionally but reading this sends a chill sensation down my spine. The worst of this issue is that there is no cure yet. However, I believe that people who are diagnosed at the early stage stands a fair chance of taking necessary actions to control it. This is really informative and helpful. Thanks for sharing
Hi Rhain,
Thank you for your comments. I hope the article makes people more aware.
Best wishes,
Michael
Hello there thanks for this awesome article it would be of help to the public as I has been of help to me..I used to work as a a sectary in a healthy consultancy firm…that was where I heard about this disease Chronic obstructive pulmonary disease (COPD) is a lung disease characterized by chronic obstruction of lung airflow that interferes with normal breathing and is not fully reversible. The more familiar terms ‘chronic bronchitis’ and ’emphysema’ are no longer used, but are now included within the COPD diagnosis.but I never not until now I never took out time to study about that is know the symptoms and the final stage of this illness…but thank to your article I have a better idea
Hi Feji,
Thank you for your comments.
Best wishes,
Michael
Hi Michael, thank you for the comprehensive and very informative post. I have never heard of COPD until now and reading through the symptoms, I wonder why I haven’t come across this condition before. Given it is the #1 cause of hospitalisation amongst industrialised nations, it’s surprising COPD has not received more publicity.
You mention in the article that the causes of COPD are often smoking-related. With many nations having introduced smokefree legislation to reduce tobacco advertising and marketing and funds to run ‘quit smoking’ programmes, is there any research to indicate that this is having an effect on the incidence of COPD? Your statistic of a 150% increase in cases over the next decade would indicate little impact on COPD rates.
Hi,
Thank you for your comments. Unfortunately COPD cases are on the rise. This is mainly due to the many toxins in the air and pollution.
Best wishes,
Michael
Four years ago I experienced a severe breathing problems. A year later, it worsened and I was diagnosed of COPD. I came across Herbal HealthPoint (w w w. herbalhealthpoint. c o m) December, 2018 and learnt about their successful herbal therapy for COPD. I immediately started on the COPD treatment; i began to notice a reduction in symptoms till it all vanished. I feel better and breath better. I Just wanted to share for people suffering from this horrible lungs disease.
Hi Susan,
I am so glad that your breathing problems have been cleared. Seems like Herbal HealthPoint provides a great service.
I am always in favor of the herbal treatments.
Thank you
All the best,
Michael
I was diagnosed of Chronic Obstructive Pulmonary Disease (COPD) in 2012 at the age of 63. I had been a heavy smoker, my symptoms started out with dry cough and shortness of breath, i ended up in the hospital, on a ventilator. I should have known it was coming, but like most smokers, thought it would never happen to me. My COPD got significantly worse and unbearable because of my difficulty catching breath. Last year, i started on a natural COPD Herbal therapy from Rich Herbal Gardens, i read a lot of positive reviews from patients who used the treatment and i immediately started on it. I had great relief with this herbal treatment. I breath very much better now, no case of shortness of breath or chest tightness since treatment. Visit Rich Herbal Gardens website ww w. richherbalgardens. com. This COPD treatment is a miracle, I feel better and breath better!!
Hi Willinie,
I am glad you found the herbal way of addressing your COPD and are feeling better today
Thank you for sharing your story.
Best wishes,
Michael
I’m 59 years old and female. I was diagnosed a couple of years ago with COPD and I was beyond scared! My lung function test indicated 49% capacity. After having had flu a year ago, the shortness of breath, coughing and chest pains continued even after being treated with antibiotics. I’ve been smoking two packs a day for 36 years. Being born without a sternum caused my ribs to be curled in just one inch away from my spine, resulting to underdeveloped lungs. At age 34 I had surgery and it was fixed. Unfortunately my smoking just caused more damage to my already under developed lungs. The problem was having is that I enjoy smoking and don’t want to give up! Have tried twice before and nearly went crazy and don’t want to go through that again. I saw the fear in my husband and children’s eyes when I told them about my condition then they start to find solution on their own to help my condition.I am an 59 now who was diagnose COPD emphysema which I know was from my years of smoking. I started smoking in school when smoking was socially acceptable. I remember when smoking was permitted in hospitals. It was not known then how dangerous cigarettes were for us, and it seemed everybody smoked but i was able to get rid of my COPD lung condition through the help of total cure herbal foundation my husband bought, totalcureherbsfoundation .c om has the right herbal formula to help you get rid and repair any lung conditions and cure you totally with their natural organic herbs,it class products at affordable prices. Purchase these medicines and get the generic medicines delivered in USA, UK & Australia,I wish anybody who starts smoking at a young age would realize what will eventually happen to their bodies if they continue that vile habit throughout their life.
Hi Ivanna,
Thank you for sharing your story. I hope other people read this also and realize how smoking can be so harmful to your health.
I am glad you are going the herbal way. I hope you have stopped smoking. Smoking wrecked havoc on my dad’s health. Perhaps seeing
him suffer has saved me from the addiction. To stop smoking after all those years I am sure is tough as you will go through a period
of withdrawals.
I personally am a recovering alcoholic and have been hospitalized on several occasions due to it. I can relate to the difficulty in
quitting any substance you have grown up with.
Ivanna you are only 59 you have many more years ahead of you. Follow through with your herbal remedies and if ever you feel you need
to talk to someone, I will be hear to listen. In fact I would like to know how you are doing.
I like to see my website offering help and healthy options to as many people as possible.
I wish you all the best,
Michael
I’m back to normal life….Of course you must quit smoking. Start using herbs instead of drugs….do your research. Also read up COPD HERBAL REMEDY from ww w besthealthherbalcentre co m, Couple drops on tongue replaces an inhalers. Asthma too. Read up on this! All lung problems and sleep apnea also. Educate yourself and take your own life back.
Hi Promise, thank you for your comments. Glad you are back to a normal life. I am a true believer in the herbal. Thank you for the link to besthealthherbalcentre.
All the best,
Michael
I was diagnosed of Parkinson disease two years ago, I started out with only Azilect, then Mirapex and sinemet as the disease progressed, but didn’t help much. Last year, I started on PARKINSON DISEASE TREATMENT PROTOCOL from Herbal Health Point (w ww . herbalhealthpoint. com). One month into the treatment, I made a significant recovery. I had great improvement with my movement and balance. Its been a year, life has been amazing
Hi Susan,
Thank you for your comments and the link to herbalhealthpoint.com. I do have an article
on Parkinsons with the mention of alternative herbal remedies. I am using a different herbal company
but will be checking out your link. I am glad to hear about the improvement. Perhaps you could share
the herbal remedies you used.
Best wishes,
Michael
HERBAL FORMULA
Start using herbs instead of drugs….Do your research. Also read up COPD HERBAL REMEDY from BEST HEALTH HERBAL CENTRE, Couple drops on tongue replaces an inhalers. Asthma too. Read up on this! All lung problems. Educate yourself and take your own life back.
Hi Promise,
Thank you for your comments. I have covered COPD and mentioned the benefits of herbal remedies.
Best wishes,
Michael
Few years ago, I began to do a lot of research and came across HERBAL HEALTHPOINT (w w w. herbalhealthpoint. c o m) and their COPD HERBAL TREATMENT. After seeing positive reviews from other patients, I quickly started on the treatment, i experienced significant recovery from symptoms, including the shortness of breath. Its been over 2 years since treatment, i live symptom free
I used the herbal treatment for almost 4 months, it reversed my COPD. My severe shortness of breath, dry cough, chest tightness gradually disappeared.