What is Tuberculosis?
Blue indicates link
Yes, it is another airborne disease. Tuberculosis (TB) is caused by bacteria (Mycobacterium tuberculosis) that most often affect the lungs. Tuberculosis is curable and preventable.
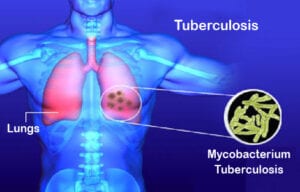
TB is spread from person to person through the air. When people with lung TB cough, sneeze, or spit, they propel the TB germs into the air. A person needs to inhale only a few of these germs to become infected.
About one-quarter of the world’s population has latent TB, which means people have been infected by TB bacteria but are not (yet) ill with the disease and cannot transmit the disease.
People infected with TB bacteria have a 5–15% lifetime risk of falling ill with TB. Persons with compromised immune systems, such as people living with HIV, malnutrition, or diabetes, or people who use tobacco, have a higher risk of falling ill.
When a person develops active TB disease, the symptoms (such as cough, fever, night sweats, or weight loss) may be mild for many months. This can lead to delays in seeking care and results in the transmission of the bacteria to others. People with active TB can infect 5–15 other people through close contact over the course of a year. Without proper treatment, 45% of HIV-negative people with TB on average, and nearly all HIV-positive people with TB will die.
Tuberculosis (TB) is a potentially serious infectious disease that mainly affects your lungs. The bacteria that cause tuberculosis are spread from one person to another through tiny droplets released into the air via coughs and sneezes.
Once rare in developed countries, tuberculosis infections began increasing in 1985, partly because of the emergence of HIV, the virus that causes AIDS. HIV weakens a person’s immune system so it can’t fight the TB germs. In the United States, because of stronger control programs, tuberculosis began to decrease again in 1993 but remains a concern.
Many strains of tuberculosis resist the drugs most used to treat the disease. People with active tuberculosis must take several types of medications for many months to eradicate the infection and prevent the development of antibiotic resistance.
Symptoms
Although your body may harbor the bacteria that cause tuberculosis (TB), your immune system usually can prevent you from becoming sick. For this reason, doctors make a distinction between:
- Latent TB. In this condition, you have a TB infection, but the bacteria remain in your body in an inactive state and cause no symptoms. Latent TB, also called inactive TB or TB infection, isn’t contagious. It can turn into active TB, so treatment is important for the person with latent TB and to help control the spread of TB. An estimated 2 billion people have latent TB.
- Active TB. This condition makes you sick and in most cases can spread to others. It can occur in the first few weeks after infection with the TB bacteria, or it might occur years later.
Signs and symptoms of active TB include:
- Coughing that lasts three or more weeks
- Coughing up blood
- Chest pain, or pain with breathing or coughing
- Unintentional weight loss
- Fatigue
- Fever
- Night sweats
- Chills
- Loss of appetite
Tuberculosis can also affect other parts of your body, including your kidneys, spine, or brain. When TB occurs outside your lungs, signs, and symptoms vary according to the organs involved. For example, tuberculosis of the spine may give you back pain, and tuberculosis in your kidneys might cause blood in your urine.
Causes
Tuberculosis is caused by bacteria that spread from person to person through microscopic droplets released into the air. This can happen when someone with the untreated, active form of tuberculosis coughs, speaks, sneezes, spits, laughs, or sings.
Although tuberculosis is contagious, it’s not easy to catch. You’re much more likely to get tuberculosis from someone you live with or work with than from a stranger. Most people with active TB who’ve had appropriate drug treatment for at least two weeks are no longer contagious.
HIV and TB
Since the 1980s, the number of cases of tuberculosis has increased dramatically because of the spread of HIV, the virus that causes AIDS. Infection with HIV suppresses the immune system, making it difficult for the body to control TB bacteria. As a result, people with HIV are many times more likely to get TB and to progress from latent to active disease than are people who aren’t HIV positive.
Drug-resistant TB
Another reason tuberculosis remains a major killer is the increase in drug-resistant strains of the bacterium. Since the first antibiotics were used to fight tuberculosis more than 60 years ago, some TB germs have developed the ability to survive despite medications, and that ability gets passed on to their descendants.
Drug-resistant strains of tuberculosis emerge when an antibiotic fails to kill all the bacteria it targets. The surviving bacteria become resistant to that particular drug and frequently other antibiotics as well. Some TB bacteria have developed resistance to the most commonly used treatments, such as isoniazid and rifampin.
Some strains of TB have also developed resistance to drugs less commonly used in TB treatment, such as the antibiotics known as fluoroquinolones, and injectable medications including amikacin and capreomycin (Capastat). These medications are often used to treat infections that are resistant to the more commonly used drugs.
Risk factors
Anyone can get tuberculosis, but certain factors can increase your risk of the disease. These factors include:
Weakened immune system
A healthy immune system often successfully fights TB bacteria, but your body can’t mount an effective defense if your resistance is low. A number of diseases, conditions, and medications can weaken your immune system, including:
- HIV/AIDS
- Diabetes
- Severe kidney disease
- Certain cancers
- Cancer treatment, such as chemotherapy
- Drugs to prevent rejection of transplanted organs
- Some drugs used to treat rheumatoid arthritis, Crohn’s disease, and psoriasis
- Malnutrition
- Very young or advanced age
Traveling or living in certain areas
The risk of contracting tuberculosis is higher for people who live in or travel to areas that have high rates of tuberculosis and drug-resistant tuberculosis, including:
- Africa
- Eastern Europe
- Asia
- Russia
- Latin America
- Caribbean Islands
Poverty and substance use
- Lack of medical care. If you receive a low or fixed income, live in a remote area, have recently immigrated to the United States, or are homeless, you may lack access to the medical care needed to diagnose and treat TB.
- Substance use. The use of IV drugs or excessive alcohol weakens your immune system and makes you more vulnerable to tuberculosis.
- Tobacco use. Using tobacco greatly increases the risk of getting TB and dying of it.
Where you work or live
- Health care work. Regular contact with people who are ill increases your chances of exposure to TB bacteria. Wearing a mask and frequent hand-washing greatly reduce your risk.
- Living or working in a residential care facility. People who live or work in prisons, homeless shelters, psychiatric hospitals, or nursing homes are all at a higher risk of tuberculosis. That’s because the risk of the disease is higher anywhere there is overcrowding and poor ventilation.
- Living in or emigrating from a country where TB is common. People from a country where TB is common may be at high risk of tuberculosis infection.
- Living with someone infected with TB. Living with someone who has TB increases your risk.
Complications
Without treatment, tuberculosis can be fatal. The untreated active disease typically affects your lungs, but it can spread to other parts of your body through your bloodstream. Examples of tuberculosis complications include:
- Spinal pain. Back pain and stiffness are common complications of tuberculosis.
- Joint damage. Tuberculous arthritis usually affects the hips and knees.
- Swelling of the membranes that cover your brain (meningitis). This can cause a lasting or intermittent headache that occurs for weeks. Mental changes also are possible.
- Liver or kidney problems. Your liver and kidneys help filter waste and impurities from your bloodstream. These functions become impaired if the liver or kidneys are affected by tuberculosis.
- Heart disorders. Rarely, tuberculosis can infect the tissues that surround your heart, causing inflammation and fluid collection that may interfere with your heart’s ability to pump effectively. This condition, called cardiac tamponade, can be fatal.
Prevention
If you test positive for latent TB infection, your doctor may advise you to take medications to reduce your risk of developing active tuberculosis. The only type of tuberculosis that is contagious is the active variety when it affects the lungs. So if you can prevent your latent tuberculosis from becoming active, you won’t transmit tuberculosis to anyone else.
Protect your family and friends
If you have active TB, keep your germs to yourself. It generally takes a few weeks of treatment with TB medications before you’re not contagious anymore. Follow these tips to help keep your friends and family from getting sick:
- Stay home. Don’t go to work or school or sleep in a room with other people during the first few weeks of treatment for active tuberculosis.
- Ventilate the room. Tuberculosis germs spread more easily in small closed spaces where air doesn’t move. If it’s not too cold outdoors, open the windows and use a fan to blow indoor air outside.
- Cover your mouth. Use a tissue to cover your mouth anytime you laugh, sneeze, or cough. Put the dirty tissue in a bag, seal it, and throw it away.
- Wear a mask. Wearing a surgical mask when you’re around other people during the first three weeks of treatment may help lessen the risk of transmission.
Finish your entire course of medication
This is the most important step you can take to protect yourself and others from tuberculosis. When you stop treatment early or skip doses, TB bacteria have a chance to develop mutations that allow them to survive the most potent TB drugs. The resulting drug-resistant strains are much more deadly and difficult to treat.
Vaccinations
In countries where tuberculosis is more common, infants often are vaccinated with the bacillus Calmette-Guerin (BCG) vaccine because it can prevent severe tuberculosis in children. The BCG vaccine isn’t recommended for general use in the United States because it isn’t very effective in adults. Dozens of new TB vaccines are in various stages of development and testing.
Diagnosis
During the physical exam, your doctor will check your lymph nodes for swelling and use a stethoscope to listen carefully to the sounds your lungs make while you breathe.
The most commonly used diagnostic tool for tuberculosis is a simple skin test, though blood tests are becoming more commonplace. A small amount of a substance called PPD tuberculin is injected just below the skin of your inside forearm. You should feel only a slight needle prick.
Within 48 to 72 hours, a healthcare professional will check your arm for swelling at the injection site. A hard, raised red bump means you’re likely to have a TB infection. The size of the bump determines whether the test results are significant.
Results can be wrong
The TB skin test isn’t perfect. Sometimes, it suggests that people have TB when they really don’t. It can also indicate that people don’t have TB when they really do.
A false-positive test may happen if you’ve been vaccinated recently with the bacillus Calmette-Guerin (BCG) vaccine. This tuberculosis vaccine is seldom used in the United States but is widely used in countries with high TB infection rates.
False-negative results may occur in certain populations — including children, older people, and people with AIDS — who sometimes don’t respond to the TB skin test. A false-negative result can also occur in people who’ve recently been infected with TB, but whose immune systems haven’t yet reacted to the bacteria.
Blood tests
Blood tests may be used to confirm or rule out latent or active tuberculosis. These tests use sophisticated technology to measure your immune system’s reaction to TB bacteria.
These tests require only one office visit. A blood test may be useful if you’re at high risk of TB infection but have a negative response to the skin test, or if you’ve recently received the BCG vaccine.
Imaging tests
If you’ve had a positive skin test, your doctor is likely to order a chest X-ray or a CT scan. This may show white spots in your lungs where your immune system has walled off TB bacteria, or it may reveal changes in your lungs caused by active tuberculosis. CT scans provide more detailed images than do X-rays.
Sputum tests
If your chest X-ray shows signs of tuberculosis, your doctor may take samples of your sputum — the mucus that comes up when you cough. The samples are tested for TB bacteria.
Sputum samples can also be used to test for drug-resistant strains of TB. This helps your doctor choose the medications that are most likely to work. These tests can take four to eight weeks to be completed.
Treatment
Medications are the cornerstone of tuberculosis treatment. However, treating TB takes much longer than treating other types of bacterial infections.
For active tuberculosis, you must take antibiotics for at least six to nine months. The exact drugs and length of treatment depend on your age, overall health, possible drug resistance, and the infection’s location in the body.
Most common TB drugs
If you have latent tuberculosis, you may need to take only one or two types of TB drugs. Active tuberculosis, particularly if it’s a drug-resistant strain, will require several drugs at once. The most common medications used to treat tuberculosis include:
- Isoniazid
- Rifampin (Rifadin, Rimactane)
- Ethambutol (Myambutol)
- Pyrazinamide
If you have drug-resistant TB, a combination of antibiotics called fluoroquinolones and injectable medications, such as amikacin or capreomycin (Capastat), are generally used for 20 to 30 months. Some types of TB are developing resistance to these medications as well.
Some drugs may be used as add-on therapy to the current drug-resistant combination treatment, including:
- Bedaquiline (Sirturo)
- Linezolid (Zyvox)
Medication side effects
Serious side effects of TB drugs aren’t common but can be dangerous when they do occur. All tuberculosis medications can be highly toxic to your liver. When taking these medications, call your doctor immediately if you experience any of the following:
- Nausea or vomiting
- Loss of appetite
- Yellow color to your skin (jaundice)
- Dark urine
- A fever that lasts three or more days and has no obvious cause
Completing treatment is essential
After a few weeks, you won’t be contagious and you may start to feel better. It might be tempting to stop taking your TB drugs. However, it is crucial that you finish the full course of therapy and take the medications exactly as prescribed by your doctor. Stopping treatment too soon or skipping doses can allow the bacteria that are still alive to become resistant to those drugs, leading to TB which is much more dangerous and difficult to treat.
To help people stick with their treatment, a program called directly observed therapy (DOT) is recommended. In this approach, a healthcare worker administers your medication so that you don’t have to remember to take it on your own.
When you are taking antibiotics it is essential to complete the prescribed dosage.
Herbal, Home Remedies For Tuberculosis.
It is essential you consult with your doctor before taking herbal remedies.
1. Garlic
Garlic is rich in sulfuric acid that destroys the germs causing TB. It also contains allicin and ajoene, which have been found to inhibit bacterial growth. Plus, its antibacterial properties and immune-boosting effect are highly beneficial for a TB patient. Garlic can be eaten raw or cooked.
- Mix together one-half teaspoon of chopped garlic, one cup of milk, and four cups of water. Boil it until it is reduced to one–fourth of the volume. Drink the mixture three times daily.
- Add 10 drops of garlic juice to a glass of hot milk and drink it before going to bed. Do not drink water afterward, as it may diminish the beneficial effects.
- Dice 10 cloves of garlic and boil them in one cup of milk. Eat the boiled pieces of garlic and then drink the milk. Do this daily for a few months.
2. Bananas
Bananas are an excellent source of nutrients and calcium that can help boost a TB patient’s immune system. They also can help alleviate cough and fever.
- Take a ripe banana, mash it, and mix in one cup of coconut water, one-half cup of yogurt, and one teaspoon of honey. Consume it twice daily.
- Make raw banana juice and drink one glass of it daily.
- You can also drink the juice of the banana plant stem to relieve symptoms like chronic cough, excess phlegm, excessive perspiration at night with a high fever, and so on. Slowly sip one to two cups of banana stem juice every two hours until symptoms subside.
3. Drumstick
Drumstick has anti-inflammatory and antibacterial properties that can help eliminate the TB-causing bacteria from the lungs and reduce inflammation resulting from the infection and constant coughing. Plus, drumstick pods and leaves are a good source of carotene, calcium, phosphorus, and vitamin C.
- Boil a handful of drumstick leaves in one cup of water for five minutes.
- Allow it to cool and add salt, pepper, and lime juice.
- Drink this daily in the morning on an empty stomach.
Also, boiled drumsticks can be consumed daily to get relief from the infection.
4. Indian Gooseberry
Indian gooseberry, also known as amla, has anti-inflammatory and antibacterial properties. The various nutrients in Indian gooseberry provide energy and enhance the body’s capacity to function properly.
- De-seed three or four Indian gooseberries. Extract the juice with the help of a juicer.
- Add one tablespoon of honey and mix it well.
- Drink this every morning on an empty stomach.
Raw Indian gooseberry or its powder can also be consumed.
5. Oranges
Oranges have many essential minerals and compounds. Orange juice has a saline action in the lungs, which eases expectorations and protects the body from secondary infections. It can boost the immune system as well.
- Add a pinch of salt and one tablespoon of honey to a glass of freshly squeezed orange juice. Mix it thoroughly.
- Drink this twice daily, one glass in the morning and another in the evening.
6. Custard Apple
The rejuvenating properties of custard apples can also help in the treatment of tuberculosis. Usually, the pulp of custard apple is used.
- Boil the pulp of two custard apples and 25 seedless raisins in one and a half cups of water until one-third of the water is left.
- Strain the mixture and add two teaspoons of powdered sugar and a one-quarter teaspoon each of cardamom and cinnamon. Allow it to cool.
- Drink this twice daily.
7. Black Pepper
Black pepper helps cleanse the lungs, which in turn helps alleviate chest pains associated with tuberculosis. Also, due to its anti-inflammatory properties, it can reduce the inflammation caused by bacteria and constant coughing.
- Fry eight to 10 black peppercorns in clarified butter.
- Add a pinch of asafetida powder and allow the mixture to cool.
- Divide the mixture into three equal parts and have one dose every few hours.
8. Walnuts
Walnuts act as a source of strength and boost the immune system of those suffering from tuberculosis. The various nutrients in walnuts can speed up the healing process.
- Combine two teaspoons of crushed walnut powder and one teaspoon of garlic paste. Add one teaspoon of clarified butter and mix the ingredients thoroughly. Eat this once daily.
- Walnuts can also be added to meals to keep the immune system strong.
9. Mint
Mint is very advantageous for treating tuberculosis due to its healing and antibacterial properties. This remedy will help dissolve mucus, revitalize body organs, and nourish the lungs as well as help to prevent dangerous side effects of medicines taken for tuberculosis.
- Mix one teaspoon of mint juice, two teaspoons of honey, two teaspoons of pure malt vinegar, and half a cup of carrot juice.
- Divide the mixture into three equal parts, and drink one dose every few hours.
10. Green Tea
Green tea can help in the treatment of tuberculosis because of its high antioxidant content and immune-strengthening properties. It also contains polyphenol compounds that can inhibit the proliferation of the bacteria that cause the disease.
Green tea leaves can be brewed with warm water to make a tea. If green tea leaves are not available, you can take them in capsule form easily found in the market. Explore more health benefits of green tea in this post.
Tuberculosis should not be taken lightly. Proper medical treatment combined with home remedies can help to overcome this health problem.
Tuberculosis Statistics
- A total of 1.5 million people died from TB in 2018 (including 251,000 people with HIV). Worldwide, TB is one of the top 10 causes of death and the leading cause of a single infectious agent (above HIV/AIDS).
- In 2018, an estimated 10 million people fell ill with tuberculosis(TB) worldwide. 5.7 million men, 3.2 million women, and 1.1 million children. There were cases in all countries and age groups. But TB is curable and preventable.
- In 2018, 1.1 million children fell ill with TB globally, and there were 205,000 child deaths due to TB (including among children with HIV). Child and adolescent TB is often overlooked by health providers and can be difficult to diagnose and treat.
- In 2018, the 30 high TB burden countries accounted for 87% of new TB cases. Eight countries account for two-thirds of the total, with India leading the count, followed by, China, Indonesia, the Philippines, Pakistan, Nigeria, Bangladesh, and South Africa.
- Multidrug-resistant TB (MDR-TB) remains a public health crisis and a health security threat. WHO estimates that there were 484,000 new cases with resistance to rifampicin – the most effective first-line drug, of which 78% had MDR-TB.
- Globally, TB incidence is falling at about 2% per year. This needs to accelerate to a 4–5% annual decline to reach the 2020 milestones of the End TB Strategy.
- An estimated 58 million lives were saved through TB diagnosis and treatment between 2000 and 2018.
- Ending the TB epidemic by 2030 is among the health targets of the Sustainable Development Goals.
Always consult with your doctor if you are experiencing any signs of tuberculosis.
Thank you for reading
Michael
Comments are welcome
There is so much great information in this article. I had no idea that many people carried TB and that it was that common. I travel a lot and I have been to many of the countries listed, the details about protecting myself and how to avoid high risk areas was so important. It really reminded me to stay safe and research the areas I’m traveling to better.
Hi Dash,
Thank you for your comments. It is essential if you travel a lot to take the necessary precautions to avoid catching any diseases. Be safe and stay healthy.
Best wishes,
Michael