What is Bladder Incontinence?
Blue indicates link
Typically this is the loss of control of when you may have to go to the washroom to urinate. Urinary incontinence is the leaking of urine that you can not control. Many people find this hard to talk about and therefore it is hard to get accurate statistics. However, we know many men and women suffer from urinary incontinence. It is nothing to be ashamed of.

Urinary incontinence is not just a medical problem. It can be due to emotional and psychological factors. This may happen with both children and adults. Some of these people do not want to be too far away from a toilet, which may cause some social issues.
What are the symptoms of bladder control problems?
Signs and symptoms of urinary incontinence can include:
- leaking urine during everyday activities, such as lifting, bending, coughing, or exercising
- feeling a sudden, strong urge to urinate right away
- leaking urine without any warning or urge
- being unable to reach a toilet in time
- Wetting your bed during sleep
- Stress incontinence. Urine leaks when you exert pressure on your bladder by coughing, sneezing, laughing, exercising, or lifting something heavy.
- Urge incontinence. You have a sudden, intense urge to urinate followed by an involuntary loss of urine. You may need to urinate often, including throughout the night. Urge incontinence may be caused by a minor condition, such as infection, or a more severe condition such as a neurologic disorder or diabetes.
- Overflow incontinence. You experience frequent or constant dribbling of urine due to a bladder that doesn’t empty completely.
- Functional incontinence. A physical or mental impairment keeps you from making it to the toilet in time. For example, if you have severe arthritis, you may not be able to unbutton your pants quickly enough.
- Mixed incontinence. You experience more than one type of urinary incontinence
What causes bladder control problems in women?
Certain life events and health problems can lead to stress incontinence in women by weakening the pelvic floor muscles:
- pregnancy and childbirth
- trauma or injury, such as sexual assault
- cystocele and pelvic organ prolapse
- menopause
Weak pelvic floor muscles can make it hard for your bladder to keep urine in during stress incontinence. Stress incontinence occurs when some of your movements—coughing, sneezing, laughing, or physical activity—put pressure on your bladder and cause urine to leak. A weak pelvic floor can also cause fecal incontinence or bowel control problems.
What causes bladder control problems in men?
Men sometimes develop UI along with prostate problems.
Prostate problems:
Men have a prostate gland that surrounds the opening of the bladder. The prostate gets bigger as a man ages. When the prostate gets too big but isn’t cancerous, a man has a condition called prostate enlargement, or benign prostatic hyperplasia (BPH).
Men with an enlarged prostate may have:
- problems with starting to urinate
- a slow urine stream
- problems fully emptying the bladder
Men who have a history of prostate cancer may have short-term or long-term UI. Cancer can damage or block the urinary tract. Or, the surgery, radiation, or other prostate cancer treatments can lead to nerve damage, bladder spasms, or stress incontinence. Bladder control problems after prostate cancer can get better over time.
Causes of Bladder Incontinence
Health changes and problems
Certain health changes and problems can lead to urinary incontinence:
- aging
- bladder infection
- constipation
- birth defects
- blocked urinary tract—from a tumor or kidney stones
- chronic, or long-lasting, coughing
- diabetes
- overweight or obesity
Some health problems can be short-term, like coughing or constipation, and can cause temporary incontinence. When a disability or a problem speaking or thinking keeps you from reaching a toilet in time, you have functional incontinence.
Problems with your nervous system are common causes of UI. UI can occur when your brain doesn’t tell the right part of your urinary tract—usually the bladder, the sphincters, or both—to do its job.
Bladder nerves and muscles can be damaged or affected by:
- Alzheimer’s disease
- stroke
- Parkinson’s disease
- multiple sclerosis
- diabetes
- certain medicines
- spinal cord injury
- anxiety
Triggers of urinary incontinence can include drinking or touching the water, hearing running water, or being in a cold environment, such as reaching into the freezer at the grocery store.
Lifestyle factors
Lifestyle factors that make women and men more likely to develop UI include:
- eating habits, such as eating foods that cause constipation
- drinking habits, such as drinking alcohol or caffeinated or carbonated beverages
- certain medicines
- physical inactivity
- smoking
Temporary incontinence is usually a side effect of a medicine or short-term health condition. Temporary incontinence can also be a result of eating habits, including alcohol or caffeine use.
Urinary incontinence isn’t a disease, it’s a symptom. It can be caused by everyday habits, underlying medical conditions, or physical problems. A thorough evaluation by your doctor can help determine what’s behind your incontinence.
Temporary urinary incontinence:
Certain drinks, foods, and medications may act as diuretics — stimulating your bladder and increasing your volume of urine.
They include:
- Alcohol
- Caffeine
- Carbonated drinks and sparkling water
- Artificial sweeteners
- Chocolate
- Chili peppers
- Foods that are high in spice, sugar, or acid, especially citrus fruits
- Heart and blood pressure medications, sedatives, and muscle relaxants
- Large doses of vitamin C
Urinary incontinence may also be caused by an easily treatable medical condition, such as:
- Urinary tract infection. Infections can irritate your bladder, causing you to have strong urges to urinate, and sometimes incontinence.
- Constipation. The rectum is located near the bladder and shares many of the same nerves. Hard, compacted stool in your rectum causes these nerves to be overactive and increases urinary frequency.
Persistent urinary incontinence:
Urinary incontinence can also be a persistent condition caused by underlying physical problems or changes, including:
- Pregnancy. Hormonal changes and the increased weight of the fetus can lead to stress incontinence.
- Childbirth. Vaginal delivery can weaken muscles needed for bladder control and also damage bladder nerves and supportive tissue, leading to a dropped (prolapsed) pelvic floor. With prolapse, the bladder, uterus, rectum, or small intestine can get pushed down from the usual position and protrude into the vagina. Such protrusions can be associated with incontinence.
- Changes with age. Aging of the bladder muscle can decrease the bladder’s capacity to store urine. Also, involuntary bladder contractions become more frequent as you get older.
- Menopause. After menopause, women produce less estrogen, a hormone that helps keep the lining of the bladder and urethra healthy. Deterioration of these tissues can aggravate incontinence.
- Hysterectomy. In women, the bladder and uterus are supported by many of the same muscles and ligaments. Any surgery that involves a woman’s reproductive system, including the removal of the uterus, may damage the supporting pelvic floor muscles, which can lead to incontinence.
- Enlarged prostate. Especially in older men, incontinence often stems from enlargement of the prostate gland, a condition known as benign prostatic hyperplasia.
- Prostate cancer. In men, stress incontinence or urge incontinence can be associated with untreated prostate cancer. But more often, incontinence is a side effect of treatments for prostate cancer.
- Obstruction. A tumor anywhere along your urinary tract can block the normal flow of urine, leading to overflow incontinence. Urinary stones — hard, stone-like masses that form in the bladder — sometimes cause urine leakage.
- Neurological disorders. Multiple sclerosis, Parkinson’s disease, a stroke, a brain tumor, or a spinal injury can interfere with nerve signals involved in bladder control, causing urinary incontinence.
Risk factors
Factors that increase your risk of developing urinary incontinence include:
- Gender. Women are more likely to have stress incontinence. Pregnancy, childbirth, menopause, and normal female anatomy account for this difference. However, men with prostate gland problems are at increased risk of urge and overflow incontinence.
- Age. As you get older, the muscles in your bladder and urethra lose some of their strength. Changes with age reduce how much your bladder can hold and increase the chances of involuntary urine release.
- Being overweight. Extra weight increases pressure on your bladder and surrounding muscles, which weakens them and allows urine to leak out when you cough or sneeze.
- Smoking. Tobacco use may increase your risk of urinary incontinence.
- Family history. If a close family member has urinary incontinence, especially urge incontinence, your risk of developing the condition is higher.
- Other diseases. Neurological disease or diabetes may increase your risk of incontinence.
Complications
Complications of chronic urinary incontinence include:
- Skin problems. Rashes, skin infections, and sores can develop from constantly wet skin.
- Urinary tract infections. Incontinence increases your risk of repeated urinary tract infections.
- Impacts on your personal life. Urinary incontinence can affect your social, work, and personal relationships.
Diagnosis
It’s important to determine the type of urinary incontinence that you have, and your symptoms often tell your doctor which type you have. That information will guide treatment decisions.
Your doctor is likely to start with a thorough history and physical exam. You may then be asked to do a simple maneuver that can demonstrate incontinence, such as coughing.
After that, your doctor will likely recommend:
- Urinalysis. A sample of your urine is checked for signs of infection, traces of blood, or other abnormalities.
- Bladder diary. For several days you record how much you drink when you urinate, the amount of urine you produce, whether you had an urge to urinate, and the number of incontinence episodes.
- Post-void residual measurement. You’re asked to urinate (void) into a container that measures urine output. Then your doctor checks the amount of leftover urine in your bladder using a catheter or ultrasound test. A large amount of leftover urine in your bladder may mean that you have an obstruction in your urinary tract or a problem with your bladder nerves or muscles.
If further information is needed, your doctor may recommend more involved tests, such as urodynamic testing and pelvic ultrasound. These tests are usually done if you’re considering surgery.
Treatment
Treatment for urinary incontinence depends on the type of incontinence, its severity, and the underlying cause. A combination of treatments may be needed. If an underlying condition is causing your symptoms, your doctor will first treat that condition.
Your doctor is likely to suggest the least invasive treatments first and move on to other options only if these techniques fail.
Behavioral techniques
Your doctor may recommend:
- Bladder training, to delay urination after you get the urge to go. You may start by trying to hold off for 10 minutes every time you feel an urge to urinate. The goal is to lengthen the time between trips to the toilet until you’re urinating only every 2.5 to 3.5 hours.
- Double voiding, helps you learn to empty your bladder more completely to avoid overflow incontinence. Double voiding means urinating, then waiting a few minutes and trying again.
- Scheduled toilet trips, to urinate every two to four hours rather than waiting for the need to go.
- Fluid and diet management, to regain control of your bladder. You may need to cut back on or avoid alcohol, caffeine, or acidic foods. Reducing liquid consumption, losing weight, or increasing physical activity also can ease the problem.
Pelvic floor muscle exercises
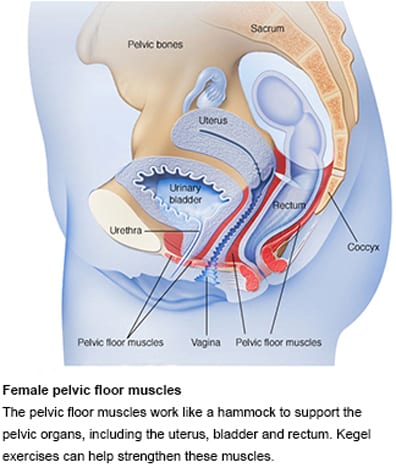
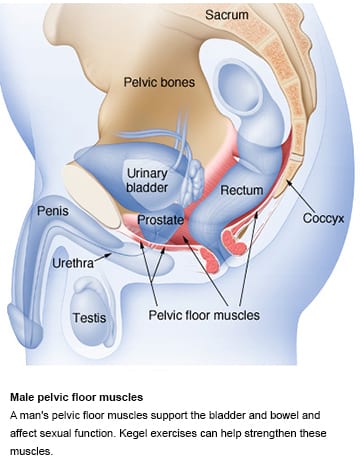
Your doctor may recommend that you do these exercises frequently to strengthen the muscles that help control urination. Also known as Kegel exercises, these exercises are especially effective for stress incontinence but may also help urge incontinence.
To do pelvic floor muscle exercises, imagine that you’re trying to stop your urine flow.
Then:

- Tighten (contract) the muscles you would use to stop urinating and hold for five seconds, and then relax for five seconds. (If this is too difficult, start by holding for two seconds and relaxing for three seconds.)
- Work up to holding the contractions for 10 seconds at a time.
- Aim for at least three sets of 10 repetitions each day.
To help you identify and contract the right muscles, your doctor may suggest you work with a physical therapist or try biofeedback techniques.
Electrical stimulation
Electrodes are temporarily inserted into your rectum or vagina to stimulate and strengthen pelvic floor muscles. Gentle electrical stimulation can be effective for stress incontinence and urge incontinence, but you may need multiple treatments over several months.
Medications
Medications commonly used to treat incontinence include:
- Anticholinergics. These medications can calm an overactive bladder and may be helpful for urge incontinence. Examples include oxybutynin (Ditropan XL), tolterodine (Detrol), darifenacin (Enablex), fesoterodine (Toviaz), solifenacin (Vesicare), and trospium (Sanctura).
- Mirabegron (Myrbetriq). Used to treat urge incontinence, this medication relaxes the bladder muscle and can increase the amount of urine your bladder can hold. It may also increase the amount you are able to urinate at one time, helping to empty your bladder more completely.
- Alpha-blockers. In men with urge or overflow incontinence, these medications relax bladder neck muscles and muscle fibers in the prostate and make it easier to empty the bladder. Examples include tamsulosin (Flomax), alfuzosin (Uroxatral), silodosin (Rapaflo), doxazosin (Cardura), and terazosin.
- Topical estrogen. For women, applying low-dose, topical estrogen in the form of a vaginal cream, ring, or patch may help tone and rejuvenate tissues in the urethra and vaginal areas. Systemic estrogen — taking the hormone as a pill — isn’t recommended for urinary incontinence and may even make it worse.
Types of pessaries.
Devices designed to treat women with incontinence include:
- Urethral insert, a small, tampon-like disposable device inserted into the urethra before a specific activity, such as tennis, can trigger incontinence. The insert acts as a plug to prevent leakage and is removed before urination.
- Pessary, a stiff ring that you insert into your vagina and wear all day. The device is typically used in someone who has a prolapse that is causing incontinence. The pessary helps hold up your bladder, which lies near the vagina, to prevent urine leakage.
Interventional therapies
Interventional therapies that may help with incontinence include:
- Bulking material injections. Synthetic material is injected into tissue surrounding the urethra. The bulking material helps keep the urethra closed and reduces urine leakage. This procedure is generally much less effective than more invasive treatments such as surgery for stress incontinence and usually needs to be repeated regularly.
- Botulinum toxin type A (Botox). Injections of Botox into the bladder muscle may benefit people who have an overactive bladder. Botox is generally prescribed to people only if other first-line medications haven’t been successful.
- Nerve stimulators. A device resembling a pacemaker is implanted under your skin to deliver painless electrical pulses to the nerves involved in bladder control (sacral nerves). Stimulating the sacral nerves can control urge incontinence if other therapies haven’t worked. The device may be implanted under the skin in your buttock and connected to wires on the lower back, above the pubic area, or with the use of a special device, inserted into the vagina.
Surgery
If other treatments aren’t working, several surgical procedures can treat the problems that cause urinary incontinence:
- Sling procedures. Strips of your body’s tissue, synthetic material, or mesh are used to create a pelvic sling around your urethra and the area of thickened muscle where the bladder connects to the urethra (bladder neck). The sling helps keep the urethra closed, especially when you cough or sneeze. This procedure is used to treat stress incontinence.
- Bladder neck suspension. This procedure is designed to provide support to your urethra and bladder neck — an area of thickened muscle where the bladder connects to the urethra. It involves an abdominal incision, so it’s done during general or spinal anesthesia.
- Prolapse surgery. In women with mixed incontinence and pelvic organ prolapse, surgery may include a combination of a sling procedure and prolapse surgery.
- Artificial urinary sphincter. In men, a small, fluid-filled ring is implanted around the bladder neck to keep the urinary sphincter shut until you’re ready to urinate. To urinate, you press a valve implanted under your skin that causes the ring to deflate and allows urine from your bladder to flow.
Absorbent pads and catheters
If medical treatments can’t completely eliminate your incontinence, you can try products that help ease the discomfort and inconvenience of leaking urine:
- Pads and protective garments. Most products are no more bulky than normal underwear and can be easily worn under everyday clothing. Men who have problems with dribbles of urine can use a drip collector — a small pocket of absorbent padding that’s worn over the penis and held in place by close-fitting underwear.
- Catheter. If you’re incontinent because your bladder doesn’t empty properly, your doctor may recommend that you learn to insert a soft tube (catheter) into your urethra several times a day to drain your bladder. You’ll be instructed on how to clean these catheters for safe reuse.
Lifestyle and home remedies
Problems with urine leakage may require you to take extra care to prevent skin irritation:
- Use a washcloth to clean yourself
- Allow your skin to air-dry
- Avoid frequent washing and douching because these can overwhelm your body’s natural defenses against bladder infections
- Consider using a barrier cream, such as petroleum jelly or cocoa butter, to protect your skin from urine
- Ask your doctor about special cleansers made to remove urine that may be less drying than other products.
If you have urge incontinence or nighttime incontinence, make the toilet more convenient:
- Move any rugs or furniture you might trip over or collide with on the way to the toilet
- Use a night light to illuminate your path and reduce your risk of falling
If you have functional incontinence, you might:
- Keep a bedside commode in your bedroom
- Install an elevated toilet seat
Alternative Treatments Remedies
Increase fiber intake:
This dietary ingredient resolves constipation, which is one of the triggers of urinary incontinence. Fiber is found in:
- Whole-grain products
- Vegetables, such as avocado
- Peas, lentils, and other beans
- Nuts and seeds
According to the Institute of Medicine, general intake recommendations are 25 grams for women up to the age of 50 years and 21 grams for those over 50 years. For men, the recommendations are 38 grams up to the age of 50 years and 30 grams for those over 50 years. This is a very easy target to achieve, just think of a salad topped with flax seeds or pumpkin seeds.
Most importantly, fiber works best when it absorbs water so make sure you drink plenty of water for your stool to be soft and formed.
Avoid Irritants
Caffeine, alcohol, and carbonated drinks have been shown to irritate the bladder and make bladder leakage symptoms worse as they make you want to urinate more. The same goes for energy drinks as they also interfere with brain signals and consequently when you need to urinate.
Another dietary change is to avoid acidic, spicy foods, and sweets. Acidic fruits such as lemons are found by some to worsen the condition so you should also avoid citrus teas. Ketchup and tomato sauces are a no-no, but surprisingly, even pineapple belongs to this group, and regrettably, chocolate has both caffeine and acid.
The choices you make greatly depend on your tolerance, so it may take a little trial and error to see what irritates your symptoms. For example, if you think caffeine is a problem, try switching to decaffeinated coffee for a while and see if your symptoms improve.
After a trial period, try restoring regular coffee in small amounts and see if the symptoms worsen. You can do this will all possible irritants to see what foods and drinks worsen your symptoms.
Maintain Healthy Vitamin D and Magnesium Levels
Many people are deficient in the sunshine vitamin, and studies show that women with sufficient vitamin D are less likely to suffer from pelvic floor disorders. The recommended daily amount is 600 IU.
On the other hand, magnesium has been shown to ease muscle spasms and therefore help the bladder empty completely, resolving sleepless nights due to incontinence.
Some magnesium-rich foods are:
- Sesame
- Bananas
- Potatoes and starch
If you opt for supplements, your doctor should be consulted first.
Stop Smoking
A chronic cough is common in smokers and is a risk factor for cancer as it aggravates the bladder and can worsen bladder leakage. Urge incontinence is three times more common in women who smoke than in those who do not, supporting studies that heavy smokers are at greater risk of incontinence.
Hydrate Properly
Too much water can worsen the condition; yet too little can also make it worse, as it could lead to UTIs. The recommendation is to drink smaller glasses of water at intervals throughout the day rather than sipping all day and to avoid drinking water at least 2 hours before bedtime.
Learning relaxation techniques can also help in learning how to control the pelvic floor muscles and is therefore advisable.
Learning how to breathe properly, meditate, or simply practice mindfulness may be a good start as stress and an already troubled bladder are a bad combination.
Train Your Bladder
Try following a strict bathroom schedule, such as going every few hours to prevent your bladder from overflowing. If you feel the urge to urinate before the scheduled time, try to hold it for a few minutes more by tightening your muscles so you can achieve longer periods between bathroom visits.
Take Care of Your Body
Be active and maintain a healthy weight. When overweight, the pressure on the abdomen is greatly increased, as is the pressure on the bladder. Multiple studies have shown that walking or swimming for just 30 minutes a day may greatly improve bladder control.
Yoga helps tighten the muscles that control the urethral sphincter and provides benefits similar to that of Kegel exercises. Moreover, yoga is good for relaxation and helps relieve anxiety and depression related to urinary incontinence.
A 2014 study published in the journal Female Pelvic Medicine & Reconstructive Surgery found that a 6-week yoga therapy program helped control urinary incontinence in women with stress incontinence. The women who took part in the yoga program experienced an overall 70 percent reduction in the frequency of urine leakage.
To help control incontinence, you can try yoga poses like Root Lock (Mula Bandha), Chair Pose (Utkatasana), Triangle Pose (Trikonasana), and Squat Pose (Malasana). Seek the help of a yoga trainer with knowledge of pelvic floor health, or join a yoga class to practice yoga properly.
Meditation and guided imagery can help you regain control over your body and reduce incontinence.
In a 2009 study, Loyola University Health System researchers found that cognitive therapy involving deep breathing and guided imagery exercises training the brain to control the bladder helped reduce the average number of urge incontinence episodes per week from 38 to 12.
Try relaxation and visualization exercises for a few weeks to notice an improvement in your condition.
Acupuncture
According to Chinese medicine, acupuncture can help reduce urinary incontinence by strengthening the urinary system and correcting the imbalance of the kidneys.
It can help increase your ability to hold urine and reduce urinary urgency. Studies have also shown this therapy to be beneficial in treating incontinence, but further well-designed studies are still needed.
Herbal Remedies
Gosha-jinki-gan: This blend of 10 herbs is one of the most studied products. Japanese researchers found that people who took it daily for 8 weeks went to the bathroom less. Other studies confirm that it lowers the urge and helps with incontinence. Chughtai says it may work by stopping nerve signals to the bladder.
Hachi-mi-jio-gan: This Chinese remedy is a blend of eight natural ingredients. A Japanese study done on animal tissue showed it eased bladder muscle contractions.
Buchu (Barosma betulina): Found in the mountains of South Africa, this flowering plant has been used as medicine since the 1650s. It has treated everything from coughs and kidney infections to stomachaches — and OAB.
Cleavers: Because of the small, sticky hooks on the leaves, this herb is usually brewed into tea to treat urinary tract infections. There’s no research on OAB, but Chughtai says many people believe it can soothe the bladder.
Horsetail: Named for its long, tail-like appearance, this member of the fern family grows in swamps, marshes, and rivers. It’s high in antioxidants, which are thought to protect against the natural stress that comes with aging. “Over time, bladder tissue can become unhealthy and fibrous,” Chughtai says. Horsetail may slow or reverse this process, although there’s little research to back that idea up or show that it helps OAB.
Corn silk: These fine threads are a pain when you’re shucking corn, but they’re packed with vitamins and antioxidants. They’ve been used to treat urinary tract infections for centuries. More recently, they’ve become a treatment for OAB. But there’s no research showing how well they work.
Ganoderma lucidum: For 2,000 years, this mushroom has been a staple of Chinese medicine. A Japanese study showed it lowered the urge to go after 8 weeks. Doctors think it lowers levels of the hormones that boost prostate growth — one cause of OAB in men.
Resiniferatoxin: Made from a Moroccan cactus-like plant, this remedy is known for its scorching-hot pepper-like burn. Experts believe it works by blocking nerves in the bladder that tell your brain you have to go. It may also help your bladder hold more, which means fewer trips to the bathroom.
Capsaicin: Chili peppers get their heat from this spicy compound. It probably acts the same way as resiniferatoxin, Chughtai says. A small trial in Thailand found that it helps you go less and controls leaks. One downside: It can cause side effects like pain and irritation.
Saw palmetto: People in Europe use this extract, made from the berries of the dwarf palm tree, to treat problems caused by an enlarged prostate. Research suggests that compounds in saw palmetto may work with nerves in your urinary tract to ease OAB.
Always contact your doctor first before trying any herbal or alternative remedies.
Thank you for reading
Michael
Comments are welcome
Hello there!
Wow! that is an incredible and a very helpful article you have there. I’m also a victim of Bladder Incontinence but I’ve never come accross a write-up or discussion that have addressed the challenge so well like this article have done. I’m glad i just learn the causes and how it can be attended to.
Thanks for that
Hi Caro,
Thank you for your comments. It is unfortunate but there are people who feel embarrassed to talk about this situation. It is a medical condition and when addressed can be cured.
Best wishes,
Michael